- Step-by-Step Roadmap to Integrate AI with EHR/EMR Systems
- AI-Integrated EHRs vs Traditional EHRs: What Really Changes
- Integration Architecture: How AI, EHR, and Data Systems Connect
- Interoperability in Practice: How Systems Actually Connect and Share Data
- Compliance, Security, and Governance in AI Integration
- Key Use Cases of AI in EHR Integration
- Cost and ROI of AI Integration with EHR
- Real Challenges of AI–EHR Integration and How to Overcome Them
- Best Practices for Integrating Artificial Intelligence with EHR Systems
- What Are the Future Trends in AI in EHR Integration?
- How Appinventiv Helps Build AI-Powered EHR Systems
- FAQs
Key Takeaways
- Start with a focused use case: Pick one problem with a clear outcome. This keeps implementation practical and measurable
- Validate EHR readiness early: Understand API access, data availability, and system limits before building anything
- Prioritize data quality first: Clean, structured data is the foundation for reliable AI outputs
- Embed AI into workflows: Insights must appear inside the EHR at the right moment to drive real usage
- Scale step by step: Launch in phases, track usage, and refine based on what actually works in practice
Step into a busy clinic for a minute. There’s a doctor scanning through tabs, with lab results on one screen and patient history on another, trying to connect everything before the next appointment starts. Nothing is missing, but it still takes time to piece it all together.
That’s where things are starting to shift. Healthcare teams aren’t looking at AI as something extra anymore. The conversation has moved to how it fits inside the systems they already use, especially EHRs and EMRs. The goal isn’t to add more tools. It’s to make the current ones easier to work with when time is tight.
You can see this shift clearly in the numbers. According to Grand View Research, the global AI in healthcare market is projected to reach over $187 billion by 2030, growing at a CAGR of more than 37%, with a significant share driven by clinical systems like EHRs and decision support tools.
In healthcare, it comes down to small but meaningful improvements. Less time searching, fewer clicks, quicker clarity. Instead of just storing patient data, systems begin to actually support decisions as they’re being made.
That’s why integrating AI with EHR and EMR systems matters. It helps turn routine workflows into smoother, more useful ones, especially in moments when every second counts. Let’s explore this in detail.
If your teams are still switching screens and chasing data, it’s costing time and care quality. Let’s identify quick wins you can implement now.
Step-by-Step Roadmap to Integrate AI with EHR/EMR Systems
If you walk into a hospital IT discussion mid-week, there’s usually a whiteboard full of arrows, systems, and a lot of “this won’t connect.” That’s where most conversations around AI integration in EHR actually begin. Not with models, but with whether the system can handle what you’re trying to build.
The difference between a pilot and a real deployment usually comes down to how well you handle integration. That’s what makes or breaks AI Integration in EHR Systems in practice.
Here’s how teams approach implementing AI in EHR systems when they want it to work beyond a demo.
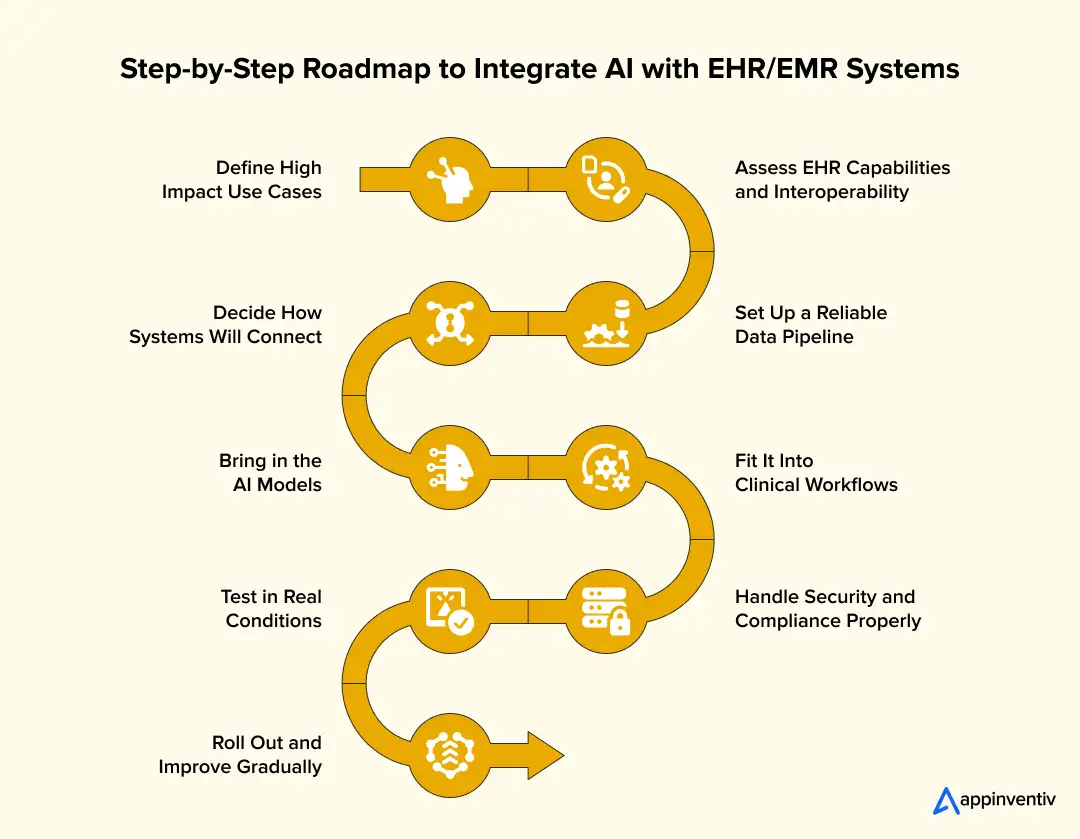
Step 1: Define High-Impact Use Cases
Start with a problem you can clearly measure. Instead of saying “we want AI,” narrow it down. Maybe your clinicians are spending too much time on documentation. Maybe high-risk patients aren’t being flagged early enough. That’s where AI starts to make sense, when it solves something specific.
Pick one use case and tie it to a clear outcome:
- Reduce documentation time
- Improve early diagnosis
- Catch anomalies faster
This keeps your Integration of AI with EHR focused and avoids unnecessary complexity early on.
Step 2: Assess EHR Capabilities and Interoperability
Now look at what your system can actually support. Some EHRs are flexible and allow API-based access. Others are far more restrictive. You might only get batch data, or limited access windows.
This matters more than it seems. Your entire integration with EHR depends on:
- Whether you can access data in real time
- Whether you can push insights back into the system
- How frequently can data be pulled
A lot of teams discover these limitations late. It’s better to surface them early before moving deeper into AI integration.
Step 3: Set Up a Reliable Data Pipeline
This is where most of the effort goes, and where things usually slow down. EHR data isn’t clean. It’s spread across systems, formatted differently, and often incomplete.
To make AI integration with electronic health records work, you need a pipeline that can:
- Pull data from different sources
- Standardize it into a usable structure
- Clean inconsistencies
- Store it securely for use
And then there’s clinical notes. A lot of important context sits in free text. If you’re integrating AI into EHR software, you’ll need a way to extract meaning from that, not just rely on structured fields.
Step 4: Decide How Systems Will Connect
At this point, you’re figuring out how everything fits together. Some setups are straightforward and use APIs for real-time interaction. Others need a middleware layer to handle multiple systems and data transformations.
You also need to decide:
- Do you need instant insights or is scheduled processing enough?
- How will data move between systems without delays?
These decisions shape how smoothly integrating artificial intelligence with EHR systems works over time.
Step 5: Bring in the AI Models
Now you add the intelligence layer. You can start with pre-built models if your use case is common. If it’s more specific, custom models may make more sense. Many teams at this stage also explore AI development services to accelerate model selection, customization, and deployment without overloading internal teams.
But here’s what teams often underestimate. The model is only as good as the data behind it. Many AI in EHR examples fail not because of the model, but because the data wasn’t ready.
So focus on:
- Using clean, representative data
- Testing outputs in real scenarios
- Making sure results are understandable
If clinicians don’t trust the output, they won’t use it.
Step 6: Fit It Into Clinical Workflows
This is where most systems quietly fail. If your solution sits in a separate dashboard, it won’t get used. Clinicians don’t have time to switch tools. For AI–EHR/EMR Integration to work:
- Insights should appear inside the EHR
- Alerts should show up at the right moment
- The system should feel like part of the workflow, not an extra step
Also, avoid overload. Too many alerts and everything starts getting ignored.
Step 7: Handle Security and Compliance Properly
This isn’t something you bolt on later. From the start, implementing AI needs:
- Controlled access to patient data
- Clear audit trails
- Secure data storage and transfer
It’s also important to make outputs explainable. When clinicians understand why something is flagged, they’re more likely to trust it.
Step 8: Test in Real Conditions
Before rolling anything out widely, see how it performs in real use.
- Does data move without delays?
- Do outputs make sense in actual clinical scenarios?
- Are clinicians using it or ignoring it?
This stage tells you whether integrating AI with EHR is actually useful, not just technically correct.
Step 9: Roll Out and Improve Gradually
Once things are stable, expand carefully. Start with one team or department. Learn what works, what gets ignored, and what needs adjustment.
Over time:
- Track usage and performance
- Watch for changes in data patterns
- Adjust how insights are delivered
This is where the real benefits of AI in systems start to show up: less manual work, faster decisions, and smoother operations.
Most teams think the challenge is building the AI layer. It isn’t. The real work is getting systems, data, and workflows to align without adding friction.
When that happens, the integration of AI with EHR stops feeling like a feature. It becomes something that just works in the background, quietly supporting better decisions without getting in the way.
AI-Integrated EHRs vs Traditional EHRs: What Really Changes
Most EHR systems were built to store information rather than actively support decision-making. As care environments get more complex, that gap becomes harder to ignore. This comparison highlights how AI-integrated EHRs shift from passive records to real-time systems.
| Area | Traditional EHRs | AI-Integrated EHRs |
|---|---|---|
| Core Role | Stores patient records and history | Actively analyzes data and supports decisions |
| Data Usage | Static requires manual review | Dynamic, surface insights automatically |
| Clinical Decision Support | Limited, rule-based alerts | Context-aware recommendations and predictions |
| Documentation | Manual entry, time-consuming | Automated notes and summaries using NLP |
| Workflow Integration | Often fragmented, multiple screens | Embedded insights within existing workflows |
| Speed of Access | Slower, requires searching | Real-time insights at the point of care |
| Error Detection | Reactive, issues found later | Proactive, flags risks and anomalies early |
| Interoperability | Often limited, depending on the system | API-driven, designed for connected ecosystems |
| User Experience | High cognitive load | Reduced friction, fewer clicks |
| Scalability | Hard to adapt to new use cases | Continuously improves with data and usage |
Why Do Traditional EHRs Fail?
Walk into a busy clinic mid-day, and you’ll notice the pattern. Tabs open, data scattered, and clinicians piecing things together under time pressure. Traditional systems weren’t built for how care actually happens today.
Here’s where they fall short:
- Data sits in silos: Information exists, but it’s spread across modules and hard to connect quickly
- Too much manual work: Documentation, validation, and follow-ups take up valuable clinical time
- Limited intelligence: Rule-based alerts don’t adapt to context or patient history
- Poor workflow fit: Systems interrupt instead of supporting the natural flow of care
- Low interoperability: Legacy setups struggle to exchange data smoothly with other systems
- Delayed insights: By the time issues are flagged, intervention windows may already shrink
In practice, the shift isn’t about replacing EHRs. It’s about making them work smarter in the moments that matter.
Integration Architecture: How AI, EHR, and Data Systems Connect
In most real implementations, the challenge isn’t adding AI. It’s connecting systems in a way that keeps data reliable and workflows uninterrupted. That’s what a solid AI architecture is designed to handle.
Here’s how AI Integration in EHR Systems typically comes together in practice.
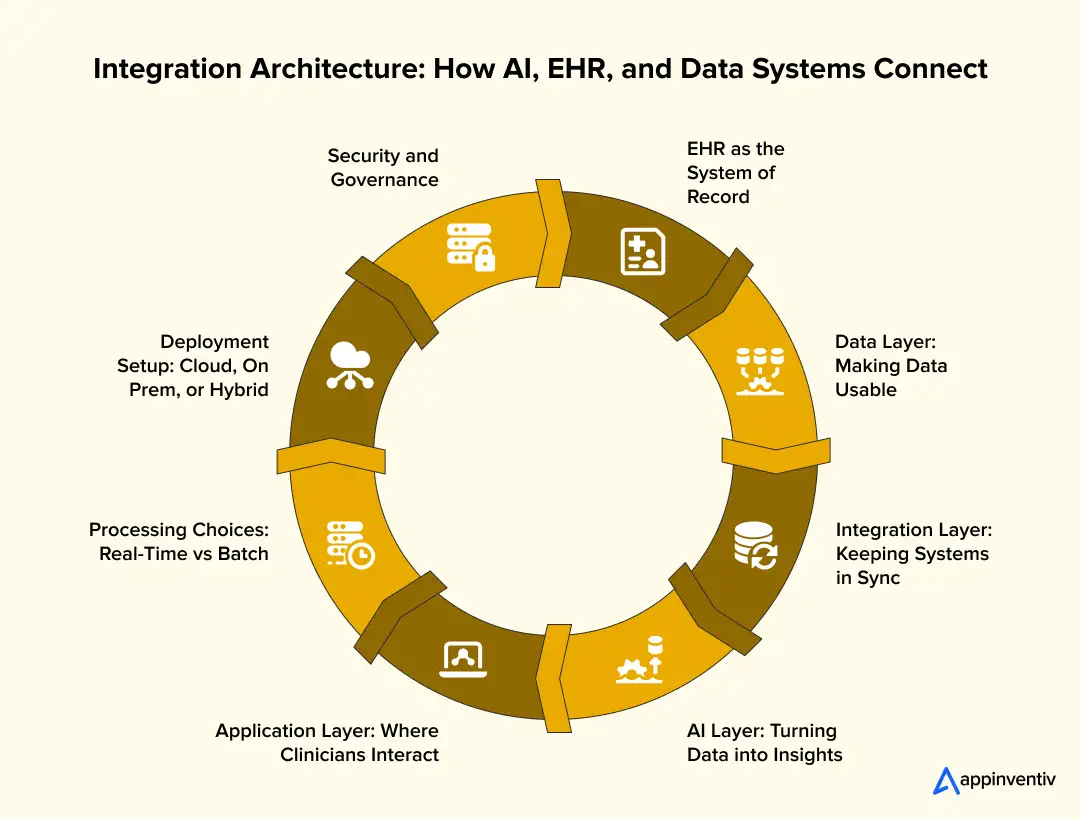
1. EHR as the System of Record
The EHR remains the central system where all clinical data is stored and managed. To make this work within integration with EHR, the role of each layer stays clearly defined:
- The EHR stores and governs patient data
- AI reads and analyzes that data without disrupting core records
- Any updates are routed through controlled, auditable workflows
This ensures stability while still enabling intelligent insights.
2. Data Layer: Making Data Usable
Before any AI processing begins, data needs to be standardized and reliable. In AI integration with electronic health records, this layer is responsible for preparing inputs by:
- Ingesting data from EHR modules, labs, and external systems
- Converting it into standardized formats like FHIR
- Cleaning inconsistencies and resolving duplicates
Additionally, unstructured data such as clinical notes, is processed using healthcare NLP pipelines, making it usable for downstream models. This step directly impacts the accuracy of implementing an AI system in EHR.
3. Integration Layer: Keeping Systems in Sync
Once data is prepared, systems need a consistent way to exchange and process it. For effective AI integration with EHR, this layer manages communication through:
- APIs for real-time data exchange
- Middleware for transformation and orchestration across systems
- Event-driven triggers that initiate actions when new data is recorded
This setup ensures that data moves efficiently and insights are generated at the right time.
4. AI Layer: Turning Data into Insights
With structured and accessible data in place, AI models can process and generate outputs. In real AI in EHR examples, this layer focuses on:
- Predicting risks and identifying patterns
- Supporting clinical decisions with contextual insights
- Detecting anomalies in patient data
To maintain reliability, models are version-controlled, monitored for drift, and continuously evaluated for clinical relevance.
5. Application Layer: Where Clinicians Interact
Insights only deliver value when they are accessible within existing workflows. When integrating AI into EHR software, outputs are:
- Embedded directly within the EHR interface
- Triggered at clinically relevant moments
- Designed to be concise and actionable
This reduces friction and increases adoption without requiring additional tools.
6. Processing Choices: Real-Time vs Batch
Different use cases require different processing approaches. In AI–EHR/EMR Integration, this is typically handled by:
- Real-time processing for alerts and decision support
- Batch processing for analytics and reporting
Choosing the right approach helps balance performance, cost, and system load.
7. Deployment Setup: Cloud, On-Prem, or Hybrid
Infrastructure decisions influence scalability, performance, and compliance. When integrating artificial intelligence with EHR systems, organizations typically choose:
- Cloud for scalable AI workloads
- On-prem for stricter data control
- Hybrid models to balance both requirements
The right setup depends on regulatory and operational needs.
8. Security and Governance
Security is embedded across every layer of the architecture. For implementing AI with EHR systems, security needs:
- Role-based access control (RBAC)
- Encryption for data in transit and at rest
- Audit logs for traceability
Additional safeguards, such as model explainability and bias monitoring, ensure trust and compliance over time.
At a technical level, this architecture connects systems. In practice, it ensures that insights are delivered reliably without disrupting care delivery.
When designed well, implementing AI with EHR systems becomes part of the system itself, supporting decisions in the background without adding complexity.
Avoid costly rebuilds. Design a system that handles real-time data, scales with demand, and fits your existing setup.
Interoperability in Practice: How Systems Actually Connect and Share Data
If you’ve worked with hospital systems, you’ve probably seen this firsthand. Two systems are technically “connected,” but the data doesn’t flow when you need it, or it shows up incomplete. That’s where interoperability in healthacre becomes a real issue, not in theory, but in daily use.
Here’s what it takes to make integration with EHR work the way teams expect.
- Standard formats matter: Using frameworks like FHIR helps different systems understand the same data without constant rework
- APIs keep things moving: Real-time healthcare APIs allow systems to send and receive updates without delays
- Legacy systems need support: Older EHRs often require middleware to bridge gaps and translate data properly
- Consistency is key: Even small mismatches in formats or codes can break workflows
Interoperability isn’t just about connecting systems. It’s about making sure they actually communicate in a way that’s reliable and useful.
When done right, AI integration feels seamless, data flows where it should, when it should, without extra effort.
Compliance, Security, and Governance in AI Integration
This is the part teams get cautious about, and for good reason. You’re working with patient data, and even small gaps can create real problems. Most teams don’t treat this as a final checklist. It’s something they build into the system from day one so nothing slips later.
Here’s how it usually plays out in real setups.
| Area | What It Means in Practice | How Teams Handle It Day to Day |
|---|---|---|
| Data Privacy & Compliance | Patient data has to be handled within strict rules at all times | Teams limit what data is used, keep it traceable, and make sure access follows clear policies |
| Access Control (RBAC) | Not everyone should see everything | Permissions are set based on roles so clinicians, admins, and systems only see what they actually need |
| Data Encryption | Data needs to stay protected whether it’s moving or stored | Encryption technology is applied across APIs and storage so data isn’t exposed during transfer or at rest |
| Audit Logging | Every action should be traceable if needed later | Systems keep records of who accessed data, what was changed, and when it happened |
| Model Explainability | Outputs shouldn’t feel like a black box | Teams make sure there’s a clear reason behind alerts or suggestions so clinicians can trust them |
| Bias Monitoring | Outputs should stay consistent across different patient groups | Regular checks are done to spot patterns that may lead to unfair or skewed results |
| Data Governance | Data needs to stay clean, consistent, and well-managed | Ownership is defined, data is maintained properly, and rules are set for how long it’s stored and used |
Most of this doesn’t show up on the surface, but it’s what keeps the system stable over time.
When implemented correctly, integrating AI with EHR systems doesn’t just work; it stays secure, predictable, and easier to trust in everyday use.
Key Use Cases of AI in EHR Integration
If you stand next to a clinician wrapping up a long shift, you’ll see where the real pressure sits. It’s not only in complex decisions. It’s in the repetitive work, the small things that add up, notes, checks, follow-ups. That’s exactly where AI starts to help in a meaningful way.
Here are a few use cases that teams actually rely on in day-to-day AI integration.
1. Clinical Use Cases
These come into play right when care decisions are being made.
- Risk prediction: Reviews patient history and current inputs to flag cases that may need attention sooner
- Decision support: Offers possible next steps or diagnoses based on available data, especially when time is limited
- Pattern detection: Picks up subtle changes in labs or vitals that might not be obvious at first glance
These are some of the most practical AI in EHR examples, particularly in environments where teams are handling high patient volumes.
2. Operational Use Cases
This is usually where teams feel the difference first.
- Automated documentation: Turns conversations or rough notes into structured records, cutting down end-of-day admin work.
- Smart scheduling: Adjusts appointments and resources based on real demand, not just fixed slots.
- Claims and billing support: Catches small coding or billing issues early, before they turn into delays or rework.
These kinds of improvements ease daily workload, which is one of the more immediate benefits of AI with EHR system adoption.
3. Patient Experience Use Cases
These quietly improve how patients interact with the system.
- Virtual assistants: Handle reminders, simple queries, and routine follow-ups so staff can focus on more critical tasks.
- Personalized care suggestions: Align recommendations with a patient’s history, making care feel more consistent over time.
Individually, these may seem small. Together, they make the overall experience smoother for both patients and staff.
Most teams don’t try to do everything at once. They start with one area that’s clearly slowing things down, test it in a real setting, and build from there.
That’s what makes AI with EHR integration work in practice. It stays grounded, proves value early, and grows without adding unnecessary complexity.
Cost and ROI of AI Integration with EHR
If you bring this up in a planning call, the conversation usually comes down to two things: cost and payoff. For most AI initiatives, the initial investment typically ranges from $40,000 to $400,000, depending on scope and system complexity.
Here’s a clear breakdown of where that cost goes and what teams typically gain from integrating AI with EHR.
| Cost Component | What It Covers | Typical Range |
|---|---|---|
| Integration & Development | API connections, middleware, workflow embedding | $15,000 – $120,000 |
| Data Preparation | Cleaning, structuring, and standardizing EHR data | $10,000 – $100,000 |
| AI Models | Pre-built tools or custom model development | $10,000 – $120,000 |
| Infrastructure | Cloud, on-prem, or hybrid setup and compute costs | $5,000 – $60,000/year |
| Compliance & Security | Access control, audit logs, regulatory requirements | $5,000 – $40,000 |
Most teams don’t see ROI from one big change. It builds over time as small inefficiencies are removed across workflows.
When AI integration is done right, the gains show up in day-to-day operations, less time on admin, smoother processes, and more focus on patient care.
Also Read: How Much Does EHR Software Development Cost
ROI Drivers: Where You Actually Feel the Change
Once the system settles in, the difference shows up in everyday moments. A doctor finishing notes a little earlier. Fewer back-and-forths with billing. Less time spent fixing small things that pile up.
- Less time stuck on documentation: Notes and updates don’t drag on, especially at the end of a long shift
- Decisions come a bit easier: The right information is already there, so there’s less digging around
- Fewer fixes later on: Small errors get caught early instead of showing up as rework days later
- The day runs a little smoother: Schedules hold better, and things feel less rushed overall
- More time where it matters: Teams get to spend more time with patients, not screens
Real Challenges of AI–EHR Integration and How to Overcome Them
If you sit with a team halfway through implementation, this is usually where things get real. Not in the planning decks, but in the small blockers, data not lining up, systems not syncing, or something built that no one actually uses. That’s where most AI-EHR Integration challenges show up.
Here’s a simple breakdown of what teams run into and how they usually work through it.
| Challenge | What It Looks Like in Practice | How Teams Handle It |
|---|---|---|
| Data Quality & Fragmentation | Patient data is spread across systems, some fields are missing, and duplicates show up more often than expected | Teams start by cleaning and standardizing data, resolving duplicates, and setting up pipelines that can handle both structured and unstructured inputs |
| Legacy System Limitations | The EHR doesn’t support real-time access or modern APIs, slowing down AI in EHR capabilities | Instead of replacing the system, teams add middleware to bridge gaps and enable smoother AI integration with EHR |
| Interoperability Gaps | Systems don’t exchange data cleanly, leading to delays or incomplete records during integration with EHR | Using standards like FHIR and API-based connections helps systems communicate more reliably |
| Workflow Misalignment | Insights exist, but clinicians don’t use them because they sit in separate tools or show up at the wrong time | Teams embed outputs directly into EHR screens and align them with real workflows, so they feel natural to use |
| Compliance & Security Complexity | Concerns around data privacy, access control, and audit requirements slow down progress | Security and compliance are built in from the start with proper access controls, encryption, and tracking mechanisms |
None of these challenges are unusual. Most teams face them at some point. What makes the difference is addressing them early and keeping things simple. That’s how AI–EHR Integration moves forward without creating more friction than it solves.
Best Practices for Integrating Artificial Intelligence with EHR Systems
If you talk to teams after their first rollout, the takeaway is usually simple. What worked wasn’t the most advanced setup. It was the part that fit in without getting in anyone’s way. That’s what makes integrating artificial intelligence with EHR systems stick.
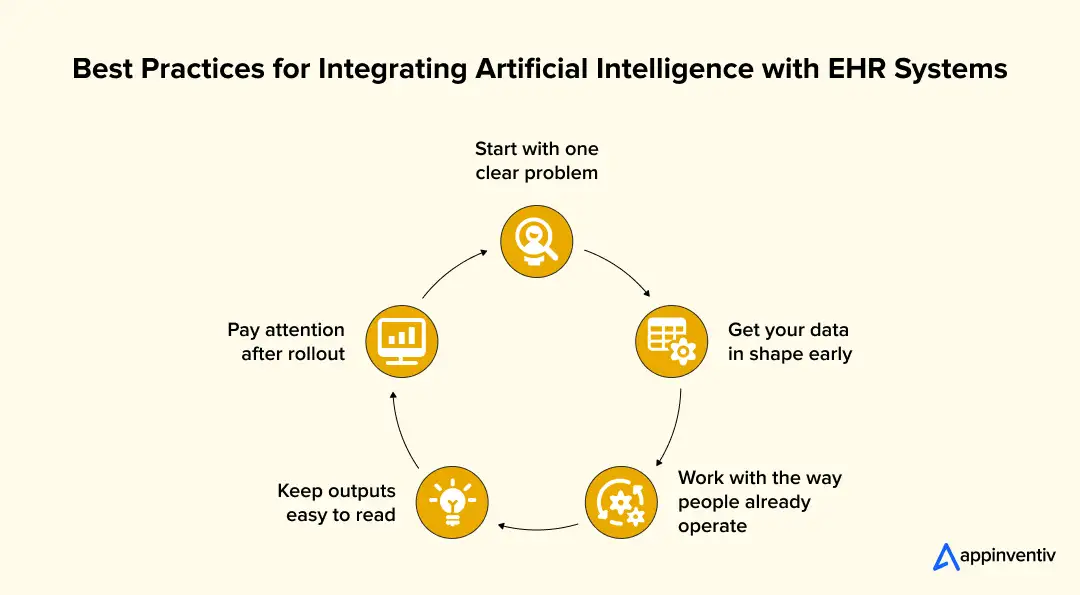
Here are a few things teams keep coming back to.
- Start with one clear problem: Don’t try to fix everything. Pick something that’s already slowing people down and solve that first
- Get your data in shape early: If the data is messy, everything else feels harder than it should
- Work with the way people already operate: If it forces new steps or extra clicks, it probably won’t get used
- Keep outputs easy to read: No one has time to interpret complex results during a shift
- Pay attention after rollout: What people ignore is just as important as what they use
The teams that get this right don’t overbuild. They keep things simple, fix what matters first, and improve as they go.
That’s what helps AI settle in naturally, rather than feeling like another system to manage.
Skip trial-and-error. Build a clear roadmap tailored to your systems, data, and use cases.
What Are the Future Trends in AI in EHR Integration?
If you look at how things are evolving, the change is subtle but important. Systems are no longer just helping teams find information. They’re starting to take on parts of the work itself. That’s where AI in EHR is heading: less searching, more doing.
Here’s how that shift is playing out, along with the technologies making it possible.
- Moving from alerts to actions (Generative AI + Automation): Instead of just highlighting an issue, systems will begin to complete tasks, draft notes, update records, or trigger follow-ups. Generative AI in healthcare is what makes this feel seamless rather than manual.
- Carrying context across every interaction (Knowledge Graphs + Context-Aware Models): Systems will connect patient history, preferences, and past visits so clinicians don’t have to piece things together each time. Knowledge graphs help link this information in a way that actually makes sense during care.
- Supporting decisions in real time (Machine Learning + Event-Based Processing): Insights will show up while care is happening, not after. Event-driven models will react to new data instantly, whether it’s a lab result or a change in vitals.
- Reducing background workload (NLP + Generative AI): A lot of the routine work, documentation, summaries and coordination will continue to move into the background. NLP and generative AI handle this quietly, without adding extra steps.
- Making systems work together more smoothly (APIs + FHIR): Data will move more cleanly between EHRs, labs, and external tools. Stronger API layers and standards, such as FHIR, will reduce the gaps teams face today.
This isn’t about adding more features or complexity. It’s about making systems feel easier to work with.
That’s where future AI trends in EHR integration are heading: systems that handle more in the background so teams can stay focused on patients rather than processes.
How Appinventiv Helps Build AI-Powered EHR Systems
If you’ve been through even one EHR upgrade, you know how it goes. Something small turns into a bigger change, and suddenly teams are adjusting to new screens, new steps, and more work. That’s usually the point where things start to slow down instead of improve.
That’s where Appinventiv steps in as an EHR Integration Company. The focus isn’t on adding more tools. It’s about getting what you already have to work better together. Cleaning up messy data, connecting systems that don’t talk to each other properly, and integrating AI into the flow clinicians already follow during a shift.
The goal is simple. Make things easier to use. Not perfect, not overengineered, just easier. Less time typing notes at the end of the day. Fewer clicks to find what you need. Information showing up when it actually helps, not five steps later.
That way of working has played out across projects over time. Appinventiv has delivered 500+ digital health platforms, worked with 450+ healthcare clients, and connected 300+ medical devices to existing systems. In many cases, hospitals have seen up to 45% improvement in operational efficiency, not because of one big change, but because small things stopped getting in the way.
If you’re looking at your current setup and thinking, “this should be smoother than it is,” it’s worth having a quick conversation. We can look at what’s working, what’s not, and where a few focused changes could make a real difference. Let’s connect!
FAQs
Q. What is AI integration with EHR systems?
A. Integration of AI with EHR systems means connecting intelligent models to electronic health records so the system can do more than store data. It can analyze patient information, detect patterns, and support decisions in real time.
In AI Integration in EHR Systems, data flows from the EHR into AI models, gets processed, and the output is returned directly into the workflow, such as alerts, summaries, or recommendations.
Q. How is AI being used in modern EHR software?
A. In modern setups, ai in ehr is used to handle both clinical and operational tasks.
Common ai in ehr examples include:
- Generating clinical notes from conversations
- Predicting patient risks like readmissions
- Supporting diagnosis with data-driven suggestions
- Detecting billing or coding errors
These are part of the broader Use Cases of AI in EHR integration, focused on saving time and improving accuracy.
Q. How does AI improve efficiency in EHR systems?
A. AI improves efficiency by reducing manual effort and speeding up access to information.
With ai integration with ehr, systems can:
- Automate documentation and routine updates
- Surface relevant patient data instantly
- Reduce manual checks in billing and records
These improvements lead to measurable benefits of ai in ehr system adoption, especially in high-volume environments.
Q. How much does it cost to implement AI in an EHR system?
A. The cost typically ranges between $40,000 and $400,000, depending on the scope and system complexity.
This includes:
- Data preparation and standardization
- Integration with EHR systems
- AI model development or licensing
- Infrastructure and compliance setup
The success of the implementation process of integration ai with ehr depends on how well the solution aligns with actual use cases and workflows.
Q. How AI integration works within EHR architecture
A. AI integration works through a layered architecture.
- The EHR acts as the system of record
- A data layer prepares and standardizes data
- AI models process the data and generate insights
- Outputs are delivered back into the EHR interface
This structure ensures AI in EHR integration works without disrupting existing systems or workflows.
Q. What interoperability standards are essential for AI–EHR integration?
A. Interoperability standards allow different healthcare systems to exchange data reliably.
Key standards include:
- FHIR for structured data exchange
- HL7 for system messaging
- APIs for real-time data access
These standards are essential when integrating artificial intelligence with EHR systems, as they ensure consistent communication across platforms.


- In just 2 mins you will get a response
- Your idea is 100% protected by our Non Disclosure Agreement.

How to use Google AI Studio to quickly build (or "vibe code") and deploy apps
Key takeaways: Building apps with AI Studio is fast, but mostly useful for prototypes, not public-ready products. AI Studio can generate Android app previews quickly, but complex features like maps, chat, and live data still break easily. Security and compliance remain major gaps, especially when apps handle users, locations, or sensitive data. Publishing through Play…

Key takeaways: Start with research before development. Map compliance before choosing the architecture. Build the data foundation before training the model. Cost can range from $100K to $5M+, depending on scope. The biggest challenge is keeping the AI accurate, explainable, and compliant after launch. Building a real estate investment AI means planning for two industries:…

What UAE CDS 2027 Means for Your Platform: Integration, Compliance, Systems, and What to Build
Key takeaways: UAE CDS 2027 age verification compliance mandates real-time, auditable systems integrated into identity, access control, and enforcement layers across platforms. Effective compliance requires risk-based, multi-layered verification combining biometrics, Emirates ID checks, device intelligence, and behavioral signals. Legacy KYC systems fail CDS expectations; enterprises must implement continuous verification with dynamic risk scoring and re-validation…