- The Strategic Role of APIs in Building Scalable Healthcare Ecosystems
- Types of Healthcare APIs
- Step-by-Step Guide to API Integration in Healthcare
- Common Challenges of API Integration in Healthcare and How to Overcome Them
- Point-to-Point Integration vs. API-Based Integration in Healthcare
- Architecture Behind High-Performing Healthcare API Ecosystems
- Security and Compliance Considerations for Healthcare APIs
- Real-World Use Cases Showing Business Impact of Healthcare API Integration
- Measuring ROI of Healthcare API Investments
- Where APIs Are Taking Healthcare Next?
- How Appinventiv Builds Scalable Healthcare API Ecosystems
- FAQs
Key takeaways:
- APIs in healthcare act as a control layer: They standardize how data is accessed, shared, and governed across EHRs, payers, and partner systems
- FHIR-led standardization reduces complexity: A consistent data model cuts rework, minimizes mismatches, and simplifies future integrations
- Event-driven, API-first architecture improves performance: Systems respond in real time, reduce dependency on synchronous calls, and scale more reliably under load
- Security and compliance must be built in early: HIPAA, GDPR, and access controls need to shape API design from day one, not after deployment
- Well-structured APIs drive measurable business outcomes: Faster partner onboarding, lower maintenance costs, and more predictable system scalability
It usually comes up right before a release. A patient app is almost ready, claims are slowing things down, and someone asks how these systems are actually going to work together without adding more delays. That’s where APIs in healthcare come into play. Today, API applications directly affect how fast services go live and how well systems hold up as usage grows.
On the ground, APIs keep data flowing between EHRs, payer systems, and external platforms without forcing everything into a single place. Eligibility checks, clinical data access, and cross-system sync all rely on this layer working quietly in the background. In enterprise setups, APIs also define how data is structured and accessed, so teams don’t have to constantly fix mismatches.
What’s changed is how central they’ve become. APIs now influence release speed, partner integrations, and overall system flexibility. According to Grand View Research, the global healthcare API market is expected to reach USD 1.72 billion by 2030, driven by demand for interoperability and real-time data.
For enterprise teams, this shifts APIs from backend support to a core layer that determines how efficiently systems scale and stay manageable over time.
While others streamline integrations and partnerships, legacy systems continue to slow you down
The Strategic Role of APIs in Building Scalable Healthcare Ecosystems
It usually holds up at first. A few integrations go live, data moves, nothing seems off. Then a small change lands, maybe an EHR field update or a slower payer response, and suddenly things start slipping across workflows. Not everything breaks, but enough does to slow teams down. That’s when it becomes clear. The issue isn’t connectivity, it’s control.
In production environments, these issues rarely appear as system outages. They show up as retries, latency spikes, and inconsistent data across systems.
This is where APIs in healthcare start doing the heavy lifting. They don’t just connect systems; they define how data is structured, who can access it, and how changes are handled without creating downstream issues. This is also where FHIR-based interoperability in healthcare becomes critical, providing teams with a consistent data foundation so integrations don’t become constant rework.
Teams that scale well don’t keep wiring systems together. They put a layer in place that keeps things consistent and contained.
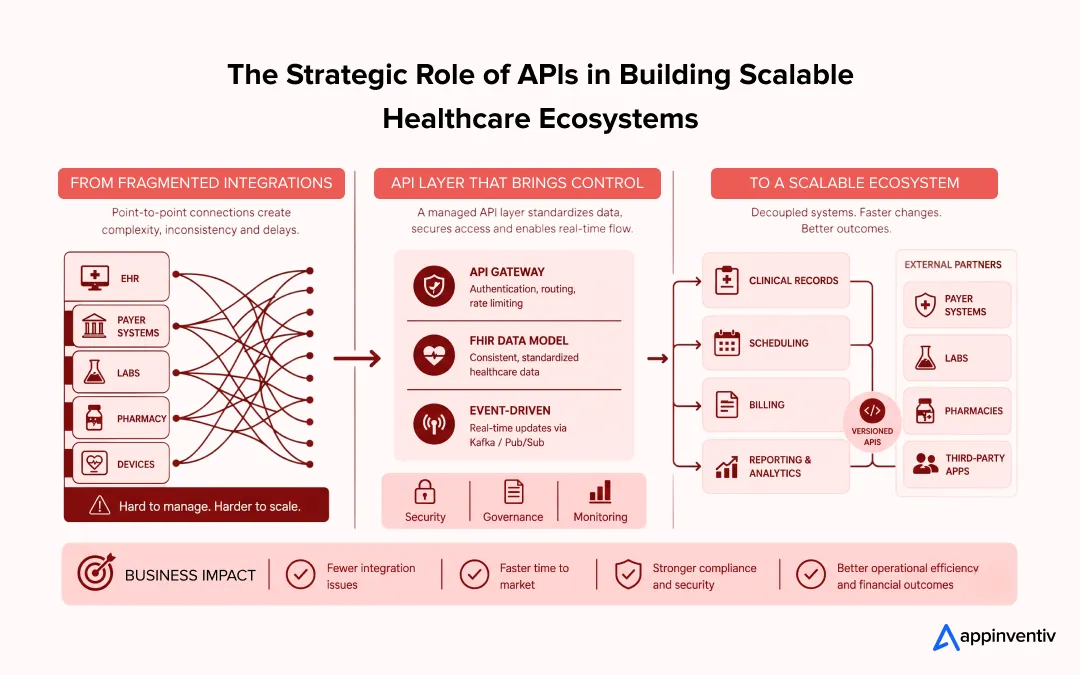
Here’s how that shows up:
- FHIR-based data model: Data follows a consistent structure, so teams aren’t remapping it for every integration
- Central API gateway: Authentication, routing, and rate limits handled in one place for consistent control.
- Event-driven updates: Systems react when something changes, rather than constantly checking for updates. Often implemented using message brokers like Kafka or Pub/Sub to handle high-throughput, asynchronous data flows without impacting response times.
- Domain-level isolation: Billing, scheduling, and records stay independent, so changes don’t spill over
- Versioned access for partners: External systems connect without breaking when APIs evolve
At this stage, healthcare API integration isn’t just about making systems talk to each other. It’s what keeps everything from getting harder to manage as you scale.
Types of Healthcare APIs
This usually isn’t planned up front. It comes up in working sessions. “We need eligibility here,” or “this has to reflect in building a scalable EHR system.” Over time, patterns start repeating, and these API categories become clearer. In enterprise setups, these APIs work together to support workflows like claims, onboarding, and care coordination.
Here’s how they typically show up:
| API Type | What It Handles | How It’s Actually Used Day To Day |
|---|---|---|
| EHR/FHIR APIs | Patient records, clinical data | Systems expose data using FHIR formats so downstream apps don’t need custom parsing every time. It’s less about standards on paper and more about avoiding constant remapping work |
| Payer/Claims APIs | Eligibility, claims, remittance | Teams wrap X12 transactions like 270/271 into APIs so checks happen instantly during workflows, not hours later through batch responses |
| Pharmacy & Lab APIs | Prescriptions, test orders, results | Orders and results move directly between systems, which cuts down the usual “has this come in yet?” back-and-forth |
| Device & Monitoring APIs | Wearables, remote patient data | Data from devices is cleaned up and structured before it reaches clinical systems, so it’s usable instead of just sitting in logs |
| Third-Party/Partner APIs | Telehealth, payments, external apps | External tools plug in through secured endpoints, usually with scoped access, without forcing changes inside core systems |
| Internal Service APIs | Scheduling, billing and identity | Core functions are split into smaller services, so when something changes, it stays contained instead of affecting everything else |
In practice, healthcare API integration doesn’t fit neatly into categories. They overlap, depend on each other, and evolve as systems grow. What matters is how well they fit together when the pressure increases.
If you’re building at scale, this step-by-step guide to healthcare API development breaks down how teams structure integrations without losing control.
Step-by-Step Guide to API Integration in Healthcare
It rarely starts with a clean slate. You’re usually dealing with an EHR that wasn’t built for open access, a billing system with its own schema, and a product team pushing for real-time features. A structured approach to API integration is less about wiring systems together and more about controlling how data flows across them without breaking compliance or performance.
Here’s how experienced teams approach it:
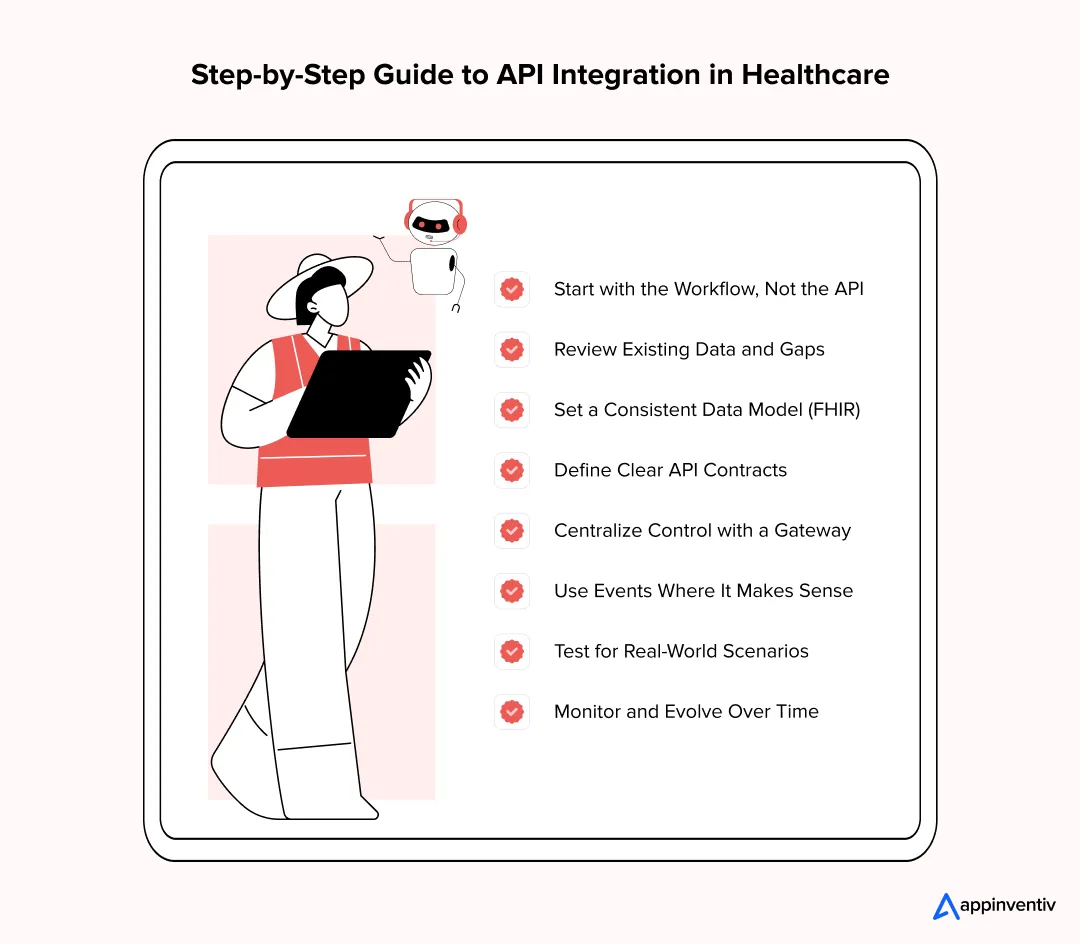
1. Start with the Workflow, Not the API
Instead of thinking in endpoints, look at what needs to happen step by step. Say a patient books an appointment, and insurance needs to be verified instantly. That flow involves multiple systems, timing constraints, and fallback paths.
At this stage, teams usually pin down:
- How fast does each interaction need to respond
- Which system holds the final, trusted version of data
- What the system should do if a dependency fails mid-process
This keeps API-driven healthcare integration tied to real operations, not just technical design.
2. Review Existing Data and Gaps
Most setups aren’t clean. You’ll find HL7 integration, partial FHIR support, and custom formats sitting side by side.
What matters here is understanding:
- Where data formats don’t align and need transformation
- Where identifiers don’t match across systems
- Which systems can handle real-time requests, and which still rely on batch processing
Catching these early prevents integration issues that only show up under load.
3. Set a Consistent Data Model (FHIR)
If every integration uses a different structure, things get messy fast. Teams that scale well usually define a single model upfront.
In practice, that means:
- Using FHIR resources as a base for clinical and operational data
- Converting incoming and outgoing data into that format
- Keeping all transformations in a dedicated layer, not scattered across services
This approach keeps the API in the healthcare industry manageable as new systems get added.
4. Define Clear API Contracts
Once APIs are live, changing them gets expensive. So teams spend time getting the contract right. That usually includes:
- Versioning endpoints so updates don’t break existing integrations
- Defining strict request and response formats
- Making critical operations repeatable without causing duplicate actions
Done well, this step makes API integration far more predictable, especially as more partners and services plug into the system.
5. Centralize Control with a Gateway
Instead of spreading logic across services, teams bring everything through a single control point. This is where requests are authenticated, routed, and monitored.
In practice, this means:
- Using an API gateway to handle routing, throttling, and request validation
- Implementing OAuth 2.0 or OpenID Connect for secure access
- Enforcing role-based permissions and encrypting all data in transit
For most API-driven healthcare integration, this layer becomes critical. It’s where you maintain visibility and enforce compliance without touching every service.
6. Use Events Where It Makes Sense
Synchronous APIs work, but they don’t scale well across all use cases. Constant polling adds load and delays updates.
So teams move certain workflows to events:
- Trigger updates when something actually changes, like a new admission or claim status
- Use message brokers or webhooks instead of repeated API calls
- Let systems react independently without waiting on each other
This reduces system strain and makes API in healthcare setups more responsive under real-world conditions.
7. Test for Real-World Scenarios
Basic testing catches obvious issues. It doesn’t prepare you for production. Teams that take this seriously simulate:
- Incomplete or inconsistent patient records
- High concurrency during peak hours
- Failures in dependent systems like payer APIs
- Unauthorized access attempts for compliance checks
This is where many API integration challenges show up early, rather than after deployment.
8. Monitor and Evolve Over Time
Once APIs are live, the work doesn’t stop. Usage grows, partners change, and systems evolve. Ongoing management usually includes:
- Tracking latency, error rates, and usage patterns
- Maintaining detailed logs for audits and troubleshooting
- Managing API versions without disrupting existing consumers
- Gradually optimizing performance and scaling infrastructure
At this stage, API integration in healthcare becomes an ongoing capability, not a one-time implementation. It’s what allows systems to grow without constant rewrites or operational risk.
Build secure, interoperable integrations that hold up as systems, partners, and data grow
Common Challenges of API Integration in Healthcare and How to Overcome Them
These issues don’t show up early. They start surfacing as usage grows, more partners connect, and small inconsistencies begin to add up. That’s when API-driven healthcare integration either holds steady or starts slowing teams down.
If not addressed, this leads to rising integration costs, delayed partner onboarding, and operational risk across systems.
Here’s what typically goes wrong at scale and how teams handle it:
| Challenge | What You’ll Notice On The Ground | How Teams Handle It |
|---|---|---|
| Data Doesn’t Match Across Systems | The same patient shows up differently in EHR, billing, and partner apps | Standardize on a FHIR-based model and use an MPI to clean up identity mismatches |
| Legacy Systems Slow Everything Down | Older HL7 systems can’t support real-time requests | Add a middleware layer to translate HL7 to FHIR and expose modern APIs without touching core systems |
| APIs Start Timing Out Under Load | Eligibility checks or record fetches lag during peak hours | Introduce caching, optimize queries, and shift frequent updates to event-driven flows |
| Small Changes Break Multiple Integrations | Updating one API disrupts partner systems or internal services | Use versioned APIs and roll out changes gradually with backward compatibility |
| Security Becomes Hard To Track | No clear visibility into who accessed sensitive data | Route everything through a gateway, enforce scoped access, and maintain audit logs |
| Too Many Custom Integrations | Every new partner requires a fresh build, increasing maintenance overhead | Move to reusable API layers instead of point-to-point connections |
| Issues Show Up Too Late | Problems are discovered only after users report them | Set up centralized monitoring, logging, and tracing from the start |
| Incomplete Data Breaks Workflows | Missing or inconsistent fields cause downstream errors | Add validation layers and define fallback handling for partial data |
At this stage, API integration isn’t about adding more connections. It’s about keeping the system stable as complexity grows.
Point-to-Point Integration vs. API-Based Integration in Healthcare
You don’t run into this on day one. It shows up a few integrations later, when a simple field change in one system suddenly breaks three others, and no one’s sure where.
| Aspect | Point-to-Point Integration | API-Based Integration |
|---|---|---|
| Architecture | Direct system-to-system links using HL7, flat files, or custom scripts | Central API layer with gateway, standardized endpoints, and service abstraction |
| Scalability | Grows as n(n-1)/2 connections, quickly becoming unmanageable | Linear scaling, where systems connect once to the API layer |
| Data Handling | Each connection maps data differently, often duplicating transformations | Canonical model (FHIR) with a dedicated transformation layer ensures consistency |
| Change Management | Tight coupling, small schema changes ripple across multiple integrations | Versioned APIs and contracts isolate changes and maintain backward compatibility |
| Performance | Often synchronous and chatty, leading to delays under load | Mix of synchronous APIs and event-driven patterns (Kafka, webhooks) for better throughput |
| Security & Access | Security handled per connection, inconsistent enforcement | Centralized via API gateway using OAuth 2.0, scoped tokens, and audit logging |
| Monitoring | Limited visibility, issues traced manually across systems | Observability through centralized logs, metrics, and tracing |
| Partner Onboarding | Each partner requires custom integration logic | Partners connect via standardized APIs with predefined contracts |
Early on, point-to-point feels faster because you’re just wiring things together. A few months in, it turns into a maintenance problem. API-based integration adds structure, so systems can evolve without everything breaking the next time you push a change.
Architecture Behind High-Performing Healthcare API Ecosystems
You only start thinking about architecture when things slow down. An API call takes longer than expected, a partner integration breaks after a small change, or data doesn’t line up across systems. That’s usually a sign the underlying structure wasn’t built to handle scale.
In high-traffic environments, APIs in healthcare depend on a few core layers working together quietly in the background. Nothing flashy, just well-defined pieces doing their job.
| Component | What’s Put In Place | What It Solves Day To Day |
|---|---|---|
| API Gateway Layer | A central gateway that handles routing, throttling, and authentication using OAuth 2.0 or OpenID Connect | Stops every service from doing its own thing. You get consistent control over traffic, access, and failures |
| Canonical Data Model (FHIR-Based) | A shared structure using FHIR resources like Patient or Encounter, with a mapping layer around it | Teams aren’t translating data differently for every integration. Less confusion, fewer mismatches |
| Microservices With Clear Boundaries | Separate services for billing, records and scheduling, each exposed through APIs | Changes stay contained. Updating one service doesn’t ripple across everything else |
| Event-Driven Communication Layer | Message queues or streaming tools that push updates when something changes | Cuts down on constant API polling. Systems react when needed instead of checking repeatedly |
| Security And Access Control Layer | Encrypted traffic (TLS), token-based access, and detailed audit logs | Sensitive data stays protected, and you know exactly who accessed what and when |
| Interoperability Layer (HL7 To FHIR) | Middleware that translates older HL7 data into FHIR-compatible formats | Let’s legacy systems stay in place while still connecting to modern applications |
| Observability And Monitoring Stack | Tracking latency, failures, and usage through logs and metrics | You catch issues early instead of hearing about them from users |
| Versioning And Lifecycle Management | Versioned APIs with clear upgrade and deprecation paths | Partners aren’t forced to update overnight when something changes |
At this level, API in healthcare isn’t something teams often talk about. It just works. Data moves where it should, systems don’t trip over each other, and adding a new integration doesn’t turn into a full rebuild.
Security and Compliance Considerations for Healthcare APIs
Security becomes real the moment an API touches patient or payment data. That’s where security features in healthcare API setups start shaping how data is protected and accessed. In the U.S., this also ties directly to regulatory mandates like the 21st Century Cures Act, ONC Cures Act Final Rule, and CMS Interoperability and Patient Access Final Rule, which enforce standardized, secure API-based data exchange.
At this point, it’s not just about moving data. It’s about controlling how it’s exposed and protected across systems.
Here’s how teams handle it in practice:
- Handle PHI at the entry point: Sensitive fields such as patient IDs or insurance data are detected as requests arrive and immediately masked or tokenized. Raw payloads are avoided unless there’s a strict audit need
- Encrypt data end to end: Data flows across multiple services, so TLS 1.2+ is enforced in transit, and strong encryption is applied at rest to prevent weak links
- Use scoped, token-based access: OAuth 2.0 is the baseline, but control comes from tightly scoped tokens. Each service or user only accesses what’s required
- Build compliance into the design: Standards like HIPAA, GDPR, PCI DSS, and SOC 2 shape how APIs are developed or structured, from access control to logging and data handling
- Maintain audit-ready logs: Every interaction with sensitive data is recorded with context, so issues can be traced without ambiguity
- Monitor and limit traffic: Rate limiting and anomaly detection help flag unusual behavior, especially on high-risk endpoints
- Apply zero-trust validation: Every request is verified, even internal ones. Trust is never assumed
- Define data retention upfront: Only essential data is stored, with clear policies on how long it stays
At this level, security doesn’t slow down API integration in healthcare. It’s built into how the system operates day to day.
Also Read: The top API security risks and how to mitigate them
Real-World Use Cases Showing Business Impact of Healthcare API Integration
In large environments, APIs in healthcare applications lead to fewer handoffs and more predictable outcomes. You don’t see APIs on a dashboard. You see them in your KPIs. Denials drop, A/R days tighten, and teams stop chasing updates across systems. In large environments, APIs in healthcare show up as fewer handoffs and more predictable outcomes.
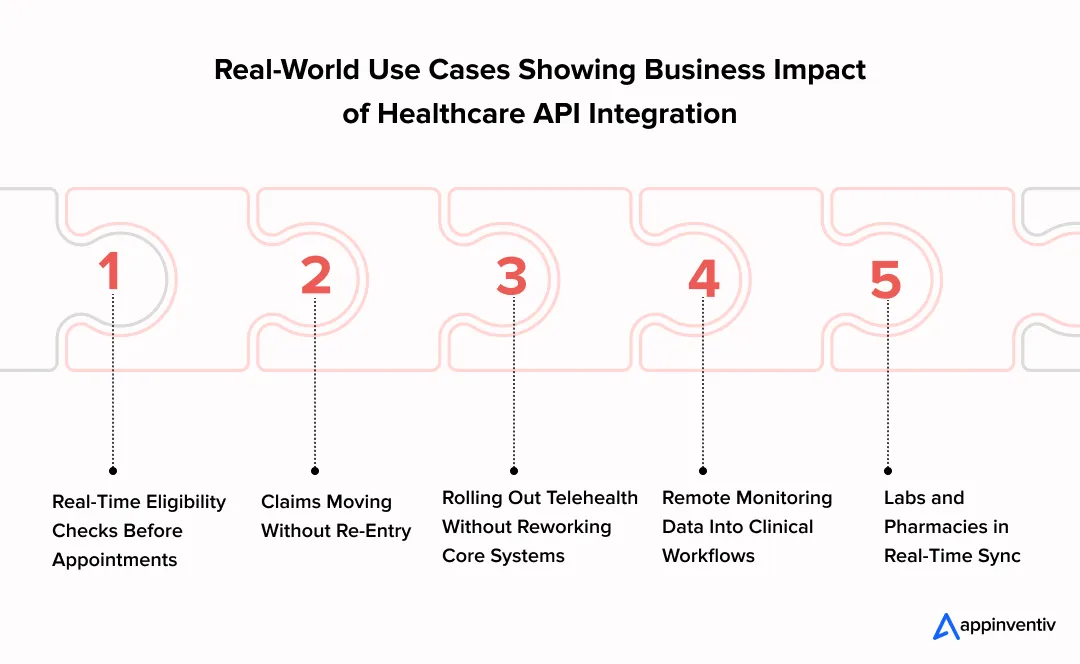
Here’s where that becomes visible:
Real-Time Eligibility Checks Before Appointments: Coverage is verified during booking using payer transactions (X12 270/271) exposed through APIs. If something doesn’t match, it’s flagged right there.
What changes: fewer eligibility-related denials, less front-desk rework, cleaner submissions on the first pass.
Claims Moving Without Re-Entry: Clinical data flows from the EHR into billing and payer systems via mapped formats (FHIR to X12) rather than being keyed in again.
What changes: shorter days in A/R, fewer touchpoints per claim and more stable cash flow.
Rolling Out Telehealth Without Reworking Core Systems: Video consult tools integrate with scheduling, identity, and documentation via APIs. The EHR stays intact.
What changes: new services go live faster, and engineering doesn’t get pulled into large backend changes.
Remote Monitoring Data Feeding Directly Into Clinical Workflows: Device data is ingested via APIs, normalized into FHIR Observations, and made available within the workflows clinicians already use.
What changes: earlier intervention signals and fewer unnecessary visits.
Labs and Pharmacies Staying In Sync In Real Time: Orders, results, and prescriptions move with callbacks and status updates, not batch files.
What changes: faster turnaround, fewer status checks, tighter coordination with external partners.
In these setups, API integration isn’t something users notice. It’s the reason processes don’t stall when volumes go up and why operations feel more controlled instead of reactive.
For enterprise teams, these use cases are less about functionality and more about reducing operational friction and improving financial outcomes.
Measuring ROI of Healthcare API Investments
You don’t usually sit down and say, “Let’s calculate API ROI.” It comes up later, in budget reviews or when someone asks why integration costs haven’t spiked despite adding new partners. With API-driven healthcare integration, ROI shows up in how efficiently systems scale and how much control you retain as complexity grows.
Here’s how enterprise teams tend to evaluate it:
- Cost of Maintaining Integrations Over Time: Instead of tracking the initial build cost, teams look at the effort required to maintain integrations. Stable API contracts and versioning reduce the ongoing engineering hours spent on fixes and updates.
- Time Spent Managing Exceptions: When integrations are brittle, edge cases pile up. ROI improves when fewer manual interventions are required to handle failed transactions, data mismatches, or retries.
- Dependency on Vendor-Specific Logic: APIs reduce tight coupling with specific vendors. The less custom logic tied to one system, the easier and cheaper it becomes to switch or upgrade later.
- Engineering Bandwidth Allocation: Teams measure how much time is spent on new development versus maintaining old integrations. A well-structured API integration in a healthcare setup shifts effort from building to fixing.
- Integration Reusability Across Use Cases: APIs built once can be reused across multiple workflows. ROI increases when the same integration layer supports new services without additional build effort.
- Operational Stability Costs: Fewer outages, retries, and incident escalations translate into lower operational risk and reduced hidden costs over time.
At this level, ROI isn’t about immediate gains. It’s about how much complexity your systems can absorb without increasing cost at the same rate. In mature systems, the cost of maintaining integrations often exceeds the cost of building them. That’s where structured API strategies deliver long-term value.
Reduce integration overhead, stabilize your systems, and scale without adding more operational pressure
Where APIs Are Taking Healthcare Next?
If you sit in on a product or ops meeting today, the tone feels different. AI isn’t being discussed as a side project anymore. It’s getting wired into scheduling, claims, and even clinical workflows. And almost every time, healthcare API integration makes that connection possible.
Here’s what’s starting to take shape:
API-First Architecture Is Becoming The Default
Most organizations have moved past experimentation. Around 83% of companies have adopted some level of API-first approach, but only a fraction have fully operationalized it. That gap matters. The next phase is not adoption, it’s maturity, building systems where APIs are treated as core infrastructure, not add-ons.
Investment Is Scaling Fast, And It’s Not Slowing Down
The market is moving quickly. Healthcare AI is projected to grow from $36.7B in 2025 to over $505B by 2033. Growth at that pace only works if data can move across systems without friction, and that’s where API-first setups come in.
Remote Care And Device Data Are Driving API Usage
Remote patient monitoring alone is expected to account for nearly 30% of API-driven applications by 2026. That means more real-time data flowing from devices into clinical systems, and APIs handling that ingestion and normalization at scale.
Standardized Data Exchange Is Becoming Mandatory, Not Optional
Interoperability in healthcare is no longer driven only by innovation. It’s being enforced at the regulatory level. By 2027, U.S. payers will be required to support FHIR-based APIs for prior authorization and data exchange.
How Appinventiv Builds Scalable Healthcare API Ecosystems
You see it early in most projects. Connecting systems isn’t the hard part. Keeping data consistent across EHRs, devices, and partner platforms as usage grows is where things start to strain. That’s where Appinventiv steps in, structuring APIs in healthcare so they hold up under real-world load, not just initial rollout.
We do this through end-to-end custom Healthcare software development services, covering API architecture, FHIR-based data models, secure integrations, and connected device ecosystems. The focus stays on building systems that scale without constant rework. To date, Appinventiv has delivered 500+ digital health platforms, served 450+ healthcare clients, and integrated 300+ connected medical devices across enterprise environments.
Here’s how that translates into real implementations:
If you’re planning to scale your healthcare platform or modernize existing systems, this is usually the point where the right architecture makes all the difference. Connect with Appinventiv to build a healthcare API strategy that holds up in real-world conditions.
FAQs
Q. Why Are APIs Essential In Healthcare Apps?
Q. APIs in healthcare are standardized interfaces that enable secure, real-time communication between systems such as EHRs, billing platforms, and patient applications.
For enterprise teams, this usually shows up in day-to-day operations. Fewer handoffs, less back-and-forth between systems, and the ability to roll out something new without touching the entire backend.
Q. What Are The Security Concerns When Integrating Third-Party APIs In Healthcare Apps?
A. The moment a third-party API is involved, control becomes the issue. Data no longer stays within your system. It moves across services, and not all of them are under your oversight.
That’s why teams lock things down early. Access is tightly scoped, data is encrypted at every step, and compliance with frameworks like HIPAA and SOC 2 is built into the integration, not added later.
Q. How Are Technological Advancements Boosting Healthcare API Adoption?
A. You can see the shift happening across teams. More AI models, more connected devices, more systems that expect real-time data rather than delayed updates.
APIs sit right in the middle of all of this. They’re what allow data to move fast enough for these systems to actually work. In most enterprise setups now, they’re no longer optional; they’re just part of how systems are built.
Q. What Are The Key Benefits Of API Integration In Healthcare?
A. You don’t notice it right away. It becomes clear when your systems scale and things keep running without constant fixes.
- Changes stay contained, avoiding ripple effects
- Data flows cleanly with fewer mismatches
- Performance holds steady under load
- Less time spent fixing integrations
- Faster partner and system onboarding
- Stronger control over data and compliance
- Reduced operational friction
At scale, APIs don’t just add features. They keep everything running smoothly as complexity grows.
Q. How do APIs work in healthcare?
A. API-driven healthcare integration acts as a secure intermediaries that allow different software systems like electronic health records (EHRs), lab systems, patient apps, and billing platforms to communicate with each other in real time. Using industry standards such as HL7 FHIR, APIs allow for structured, permissioned data sharing. They ensure that data flows seamlessly between stakeholders while adhering to strict privacy and access controls.
Q. What are APIs used for in healthcare?
A. APIs are used across the healthcare ecosystem to enable core digital functions. These include accessing EHR data, booking appointments, exchanging lab results, processing claims, enabling remote patient monitoring, integrating wearable health data, and powering mobile health apps. They serve patients, providers, payers, and vendors alike – each relying on APIs to enable faster, more informed, and automated workflows.
Q. How are APIs improving efficiency in healthcare?
A. Integrating APIs into healthcare workflow improves efficiency by automating manual tasks, reducing redundancies, and enabling real-time access to critical data. For example, appointment APIs eliminate scheduling bottlenecks, while EHR access APIs allow clinicians to retrieve patient history without delays. APIs also power backend operations like claims adjudication or inventory management, allowing care teams to focus on delivery instead of administration.
Q. What are some common healthcare API examples used in the industry?
A. Healthcare API examples include FHIR (Fast Healthcare Interoperability Resources) APIs for standardized data exchange, EHR (Electronic Health Record) APIs like those from Epic or Cerner for accessing patient records, and telehealth APIs like Doxy.me for virtual care integration. These APIs enable seamless data sharing and interoperability across healthcare systems.
Q. How do healthcare APIs improve patient experience?
A. By enabling services like digital appointment booking, on-demand access to medical records, personalized treatment updates, and remote monitoring, APIs in healthcare help patients stay engaged and informed. They reduce wait times, increase transparency, and give patients more control over their care journeys – ultimately improving satisfaction and health outcomes.
Q. How do healthcare APIs drive business innovation?
A. APIs unlock innovation by making healthcare systems more modular and flexible. Organizations can experiment with new features, integrate external platforms, and scale digital services quickly. Whether it’s launching a virtual care platform, connecting to a pharmacy network, or building predictive care models, API-driven healthcare integration shortens development cycles and reduces integration complexity, making it easier to innovate without overhauling core systems.
Q. Why are healthcare APIs considered the future of digital health businesses?
A. As the industry moves toward consumer-centric care, value-based models, and nationwide interoperability, APIs are becoming foundational to digital health strategy. They enable organizations to adapt faster, partner more broadly, and personalize care at scale. For digital health businesses, APIs are no longer just technical infrastructure – they are strategic levers for growth, compliance, and differentiation.


- In just 2 mins you will get a response
- Your idea is 100% protected by our Non Disclosure Agreement.

Key Takeaways A single application flaw can expose millions of records and trigger fines reaching $16 million or more. Most HIPAA violations trace back to preventable gaps in identity, APIs, monitoring, and cloud configuration. Breach impact is rising faster than incident count, with exposure scaling to hundreds of millions of records. Delayed detection increases financial…

Telehealth Business Ideas for 2026: Models, Technology Stack, and Growth Strategy
Key Takeaways Choose what people will keep using: The strongest telehealth models solve ongoing needs, not one-time problems. Integration matters more than features: Platforms that fit into real care workflows tend to scale without friction. Recurring care drives stable revenue: Chronic care, employer-led models, and guided programs create consistent usage. Partnerships accelerate growth: B2B and…
How Much Does EHR Software Development Cost? Enterprise Pricing, Hidden Costs, and ROI Analysis
Key Takeaways EHR implementation costs vary widely, from $20,000 for small clinics to $900,000+ for enterprise systems, based on scope, complexity, and customization. Whereas EHR software development costs between $30,000 to $1M+, depending on the complexity of development, choice of technologies and advanced features. Hidden costs like data migration, workflow disruption, training, and compliance can…