- Why Telehealth Is Now Core to Australian Healthcare Delivery
- Telehealth Market Signals in Australia: Adoption Trends, Investment, and Policy Direction
- Common Strategic Mistakes in Telehealth App Development in Australia
- How to Build a Telehealth App in Australia: Best Practices and Step by Step Process
- What Are the Core Features of a Telehealth App in Australia?
- The Australian Regulatory Terrain: What Compliance Actually Means for Your Telehealth App Architecture
- Architecture Blueprint for Secure and Scalable Telehealth Platforms
- Real-World Use Cases of Telehealth Apps, Gaining Traction in Australia Right Now
- Business and Clinical Benefits of Telehealth Platforms in Australia
- How Much Does It Cost to Develop a Telehealth App in Australia?
- Build vs Buy: What is the Right Approach for Telehealth Platform Adoption in Australia
- AI and Remote Monitoring: What Is Actually Production-Ready in Australia
- Future Trends in Telehealth: Australia 2026 and Beyond
- How Appinventiv Builds Compliant Telehealth Platforms in Australia
- FAQs
Key takeaways:
- Telehealth app development in Australia requires aligning compliance, clinical workflows, and integrations from the outset to avoid costly redesign and regulatory risk.
- Integration with national systems like My Health Record and Medicare determines real platform value, not just frontend features or consultation capabilities.
- Enterprises that treat telehealth as long-term digital infrastructure, not a short-term solution, achieve better scalability, adoption, and measurable clinical outcomes.
- The cost to build a custom telehealth app in Australia ranges from AUD 70,000 for a functional MVP to AUD 700,000 for enterprise platforms.
When bushfires swept through regional New South Wales in 2019 and 2020, thousands of patients in affected communities lost access to their regular GPs for weeks. Clinics closed, roads became impassable, and the public system absorbed a level of pressure it was never designed to handle. That moment exposed a structural limitation in Australia’s healthcare model. Access could not depend solely on physical proximity.
This incident was further validated in late 2024 by the Mid North Coast Local Health District, which proved that virtual care is now a permanent pressure valve for the system. By deploying the Mid North Coast Virtual Care (MNCVC) service, they achieved a 4.64% reduction in low-acuity emergency department presentations (Source: BMJ Open, 2025).
Telehealth app development in Australia has since evolved into a core healthcare infrastructure priority. Enterprises are now building platforms that integrate compliance, clinical workflows, and national health systems rather than standalone applications.
This blog covers what it takes to build a secure, clinically sound, and commercially viable digital health platform, from architecture decisions to the cost structures that separate platforms that scale from those that stall.
If you’re planning to build or modernise, aligning architecture and compliance early is critical.
Why Telehealth Is Now Core to Australian Healthcare Delivery
The shift from convenience to clinical necessity has changed the commercial and strategic calculus for health organisations. Telehealth is no longer a side channel; for significant patient cohorts, it is the primary access point, and platforms need to be built accordingly.
The Policy Signal Is Unambiguous
The Australian Government’s position here is not subtle. The National Digital Health Strategy 2023-2028, delivered through the Australian Digital Health Agency, explicitly centres telehealth as a pillar of long-term service delivery rather than a supplementary tool.
This policy direction is further cemented by the 1800MEDICARE service launch on 1 January 2026. Providing a free, nationwide, 24/7, nurse-led health advice and urgent GP telehealth line directly reflects the government’s commitment to integrated digital care.
For enterprises, this translates into a need for platforms that are interoperable, compliant, and scalable by design.
The Rural Access Gap Is a Commercial Opportunity
Australia’s geography creates a structural access problem that telehealth is uniquely positioned to address. AIHW data consistently shows that outer regional and remote areas have roughly half the GP-to-population density of major cities.
Any platform targeting meaningful market penetration in Australia needs to account for this reality. That means offline capability for intermittent connectivity, clinical workflows relevant to chronic disease management, and aged care, both of which are disproportionately represented in rural and remote populations.
Hybrid Care Is the New Standard
Most enterprise health organisations are no longer choosing between physical and digital care; they are managing patient journeys that move across both. A specialist consultation might begin via telehealth, require an in-person examination, and follow up digitally. Platforms that treat telehealth as a standalone channel rather than an integrated layer of care delivery are building for a model that the market has already moved beyond.
Telehealth Market Signals in Australia: Adoption Trends, Investment, and Policy Direction
Australia’s digital health market is projected to reach AUD 8.1 billion by 2028 (Statista, 2024), with growth concentrated in mental health, aged care, and chronic disease management.
Medicare telehealth expansion has moved from temporary to embedded policy, significantly widening the commercial opportunity for platforms that integrate billing and compliance natively.
What this means for enterprises:
Platforms built around specific clinical pathways, supported by Medicare-aligned billing, and designed for practitioner workflow rather than patient novelty, are better positioned commercially than general-purpose video consultation tools.
Common Strategic Mistakes in Telehealth App Development in Australia
Most telehealth platform failures in Australia are not caused by technical complexity. They stem from architectural assumptions made early in the process that collide with compliance requirements, integration realities, or clinical workflow needs discovered far too late.

Mistake 1: Treating Telehealth as a Video-Calling Problem
The most common error is teams that build around a consultation interface and later realise that a regulated healthcare platform requires identity verification, clinical traceability, system integration, and audit-ready data handling beyond basic interaction layers.
At that point, retrofitting compliance becomes expensive and architecturally awkward. The platform becomes a liability rather than an asset.
Mistake 2: Leaving Compliance Until QA
When regulatory requirements are not mapped at architecture stage, they surface during quality assurance, or worse, post-deployment. Remediation at that point can consume nearly 30-40% of the original build cost.
For any organisation considering telemedicine app development in Australia, compliance alignment must be embedded during architectural planning, as it directly shapes data models, infrastructure choices, and integration design.
Mistake 3: Underestimating Integration Complexity
Connecting to practice management systems, pathology platforms, My Health Record, and pharmacy dispensing networks requires careful API design and tolerance for inconsistent data standards across legacy systems.
Teams that treat integration as a sprint task rather than an architectural layer consistently miss timelines and budget. The integration layer is where the clinical value actually lives, and it deserves the same attention as the product layer above it.
Mistake 4: Applying Global Templates to an AU-Specific Problem
Australia’s Medicare billing structure, Privacy Act requirements, and data residency obligations create enough localisation overhead that starting from an offshore template usually costs more in adaptation than building fit-for-purpose from the outset.
Digital health platform development in Australia is a local problem that requires local architectural thinking.
How to Build a Telehealth App in Australia: Best Practices and Step by Step Process
Telehealth platform delivery follows a structured sequence where each phase builds on validated outputs from the previous one. The organisations that compress or skip phases to hit a faster launch date consistently encounter more costly remediation work downstream. Here are the key steps to build telehealth app in Australia, moving from a whiteboard concept to a nationally conformant, secure, and scalable clinical infrastructure.
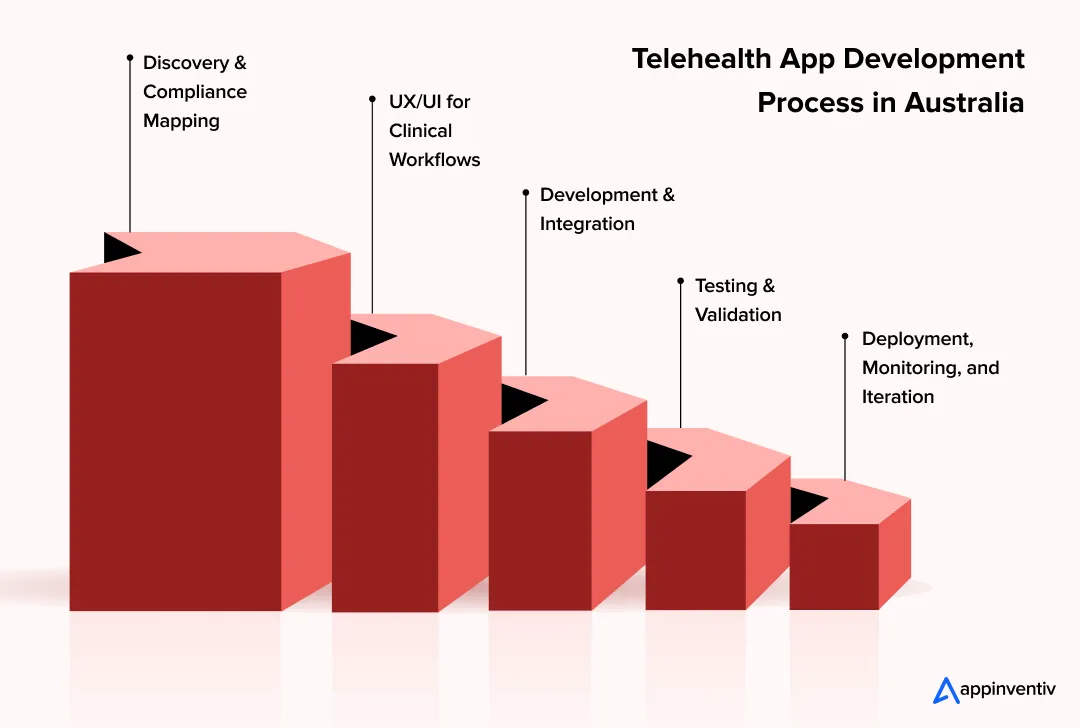
1. Discovery & Compliance Mapping
This is the initial stage where you need to pin down the platform’s “clinical intent.” It is about deciding whether the software is a simple wellness tool or sits under the Therapeutic Goods Administration (TGA) 2026 rules for Medical Devices.
You should map every feature against the latest exclusion lists to avoid a costly rebuild halfway through. This is also when you identify which “Modified Monash Model” zones you’re targeting, as rural connectivity and Medicare billing rules change the moment you move outside metropolitan areas.
2. UX/UI for Clinical Workflows
The primary barrier to telehealth adoption is “double-handling” data. Thus, this stage focuses on killing off “double-handling.” In the Australian context, if a doctor has to type a patient’s name twice because your app doesn’t talk to their practice software, they simply won’t use it.
You should prioritise “one-click” journeys where a booking instantly triggers a Medicare check and opens a secure room. At this point, ensure the interface meets WCAG 2.2 accessibility standards so that elderly patients or those with low digital literacy can navigate a consult without needing a tech support line.
3. Development & Integration
This is where developers turn the app into a working part of the national health grid. They use HL7 FHIR to make sure the platform can “talk” to My Health Record and the national Healthcare Identifiers Service. While the frontend takes shape, the team bakes in the Zero Trust security layers and complex Australian billing logic.
This allows the backend to automatically suggest the right MBS item numbers based on how long the consult lasts, saving the practitioner from manual coding errors.
4. Testing & Validation
Standard QA doesn’t cut it when patient safety is involved. At this stage, you should run “stress tests” to ensure the video stays crystal clear even on patchy regional NBN connections. The team then puts the platform through the Australian Digital Health Agency’s conformance engine.
This is where you verify that every digital script and pathology request uses SNOMED CT-AU terminology, ensuring they are instantly recognised by every pharmacy and lab across the country.
5. Deployment, Monitoring, and Iteration
Once you’re ready to go live, you need to deploy the platform into Australian-based cloud zones to keep patient data on home soil. But launch day is just the beginning; you should now shift into “Clinical Governance Monitoring” to see how doctors actually use the tool. Because MBS rules and TGA guidelines move fast, you’ll need an iterative maintenance plan. This ensures the platform gets “compliance patches” just as often as security updates, keeping your risk low and your clinical utility high.
Final Project Checklist
Before you hire a mobile application development company in Australia to build your custom and compliant telehealth platform, use this checklist to ensure your final project alignment meets 2026 Australian enterprise standards:
- Data Sovereignty: Ensure all “Sensitive Information” stays within Australian AWS/Azure zones.
- MBS Compliance: Confirm the platform automates 2026 Medicare billing logic.
- Interoperability: Validate that My Health Record syncing is native, not an add-on.
- Clinical Safety: Verify that the UI meets WCAG 2.2 and supports low-bandwidth regional use.
See how Appinventiv builds AU-compliant telehealth platforms from discovery to deployment before committing to development.
What Are the Core Features of a Telehealth App in Australia?
Feature completeness in a telehealth platform is not about how many things it can do. It is about whether each feature is clinically relevant, workflow-aware, and built to handle the compliance requirements of the Australian healthcare environment. Here we have listed the features of telehealth applications in three categories:
For Patients: Seamless Access and Autonomy
- Secure User Registration: Onboard patients using 100-point identity verification or myGovID to ensure digital profiles match a verified Individual Healthcare Identifier (IHI).
- Appointment Scheduling: Provide real-time booking that syncs with clinic management software, letting patients pick slots based on actual practitioner availability.
- Video Consultations: Use high-definition, encrypted video that stays stable even on regional NBN connections, meeting Ahpra’s “real-time” clinical standards.
- Digital Prescriptions: Send eScript tokens via SMS or email, fully integrated with the national Active Script List (ASL) framework for pharmacy pickup.
- Payment and Medicare Integration: Automate bulk-billing checks and process private payments or Medicare rebates instantly once the virtual consultation wraps up.
- Access to Medical Records: Offer a secure portal where patients view shared health summaries and pathology results synced from the national record.
For Healthcare Providers: Clinical Governance and Flow
- Patient Management Dashboard: Access a unified view of patient history, blending local clinic data with real-time uploads from the My Health Record system.
- ePrescribing & ASL Management: Issue digital scripts within the workflow, allowing practitioners to manage “Active Script Lists” without switching between different applications.
- Secure Messaging: Exchange encrypted clinical images or documents with patients, ensuring all communication strictly adheres to the Australian Privacy Principles.
- Billing & Claims Management: Automate the assignment of MBS item numbers, ensuring practitioners are paid correctly for telehealth services while cutting manual coding time.
- AI Analytics & Reporting: Track clinical outcomes and patient throughput with real-time data, helping you identify trends in chronic disease management or attendance.
For Administrators: Governance and Integration
- User Role Management: Set granular access levels so admin staff manage billing while sensitive clinical notes remain restricted to authorised medical practitioners.
- Compliance & Audit Logs: Keep tamper-proof records of every data access or consult, ensuring the organisation is always ready for a My Health Record audit.
- EHR/EMR Integration: Connect via HL7 FHIR APIs to major Australian systems like Best Practice or MedicalDirector to prevent fragmented patient data.
- Informed Consent Modules: Digitally capture and store patient consent for telehealth and financial arrangements before the consult starts, as required by Medicare.
Additional Critical Features Often Overlooked
- Consent Management: Structured capture of patient consent with clear records, supporting legal defensibility and transparent care delivery practices.
- Low-Connectivity Resilience: Ability to function in unstable network conditions, with data syncing once connections recover in remote areas.
- Standards-based Interoperability: Use of formats such as FHIR to ensure compatibility with national systems and third-party providers over time.
- Alerts and Notifications: Reminders for appointments, follow-ups, and care actions, reducing missed interactions and improving patient adherence.
- Pre-consult Triage Support: Optional intake assessments that help prioritise cases, allowing clinicians to focus attention where it is most needed.
The Australian Regulatory Terrain: What Compliance Actually Means for Your Telehealth App Architecture
Compliance in Australian digital health is not a checklist you run through at the end of a build. It is a set of architectural constraints that shape decisions about data storage, access control, audit logging, and third-party integrations from day one. The earlier you map it, the less it costs.

The Three Pillars of AU Clinical Governance
1. Ahpra & National Board Standards (2026 Update)
Following the October 2025 pivot, Ahpra mandates that telehealth must mirror in-person quality. Your architecture must natively support real-time video/audio; platforms relying on asynchronous “online questionnaires” for prescribing now face immediate regulatory de-registration and whistleblower risk under expanded National Law protections.
2. Privacy Act & APP 8 (Data Sovereignty)
Under the Australian Privacy Principles (APPs), health data is “Sensitive Information.” To satisfy APP 8, your platform should maintain sovereign data residency within Australian cloud zones (e.g., AWS Sydney). Using offshore analytics or storage without explicit, demonstrated safeguards now triggers mandatory audit flags.
3. My Health Records Act & ADHA Guidelines
Syncing with the national grid requires compliance with the My Health Records Act 2012. This isn’t just about security; it’s about interoperability. Your backend must support HL7 FHIR protocols and SNOMED CT-AU terminology to ensure clinical data flows accurately between your app and the national system.
Security and Sovereign Resilience
Zero Trust Architecture (ZTA)
In 2026, ZTA is the benchmark for the Notifiable Data Breaches (NDB) scheme. By eliminating “implicit trust,” ZTA minimises the “blast radius” of an incident. This allows you to demonstrate “effective remediation” to the OAIC, often avoiding the reputational damage of a public breach notification.
Virtual Care Provider Standards (March 2026)
The recently launched Australian Telehealth Standards establish new benchmarks for quality and safety. Compliance with these industry-led standards is becoming a prerequisite for enterprise health tenders and private health insurance (PHI) provider recognition.
ISO 27001 & ISO 27799
Standard ISO certification is no longer enough. Alignment with ISO 27799 (Health Informatics Security) is now a baseline requirement for procurement by State Health Departments and hospital networks.
Talk to our healthcare technology team about a structured discovery engagement before you commit to a build approach.
Architecture Blueprint for Secure and Scalable Telehealth Platforms
In telehealth app development in Australia, architecture needs to support both clinical workflows and regulatory expectations. This requires a layered approach where every layer, from data storage to real-time communication, carries clear responsibilities and governance controls.
| Layer | Component | AU-Specific Consideration |
|---|---|---|
| Frontend | iOS/Android apps + Web portals | Improves adoption and reduces support load |
| Backend | Microservices architecture | Handles fluctuating demand efficiently |
| Real-Time Comms | Encrypted WebRTC / TURN servers | Ensures AU-hosted endpoints for data sovereignty |
| Data Layer | Encrypted databases + RBAC | Ensures compliance and audit readiness |
| Integration | HL7 FHIR APIs for EHR/Medicare | Enables interoperability with health systems |
| Infrastructure | AWS Sydney / Azure Australia East | Supports compliance and reliability |
The tech stack choice for telemedicine app development in Australia should be selected based on these architectural needs rather than developer familiarity alone. Choices around frameworks, databases, and cloud services need to align with compliance, scalability, and integration goals.
At the backend, the tech stack for telemedicine app development in Australia typically includes:
- Node.js or Python-based microservices for API and business logic layers
- PostgreSQL or equivalent relational databases with field-level encryption
- Redis for real-time session management and caching
- Kubernetes-orchestrated containerised deployments for scalability and resilience
On the frontend, React Native is the most common choice for patient-facing mobile applications, primarily because it reduces the maintenance overhead of separate iOS and Android codebases without sacrificing performance at the level Australian health users expect.
Real-World Use Cases of Telehealth Apps, Gaining Traction in Australia Right Now
Seeing how telehealth app development in Australia translates into clinical outcomes helps you narrow your platform’s focus. In 2026, the “all-in-one” approach is being replaced by platforms that do one thing exceptionally well – whether that is managing chronic disease in the outback or providing 24/7 support for residential aged care facilities.
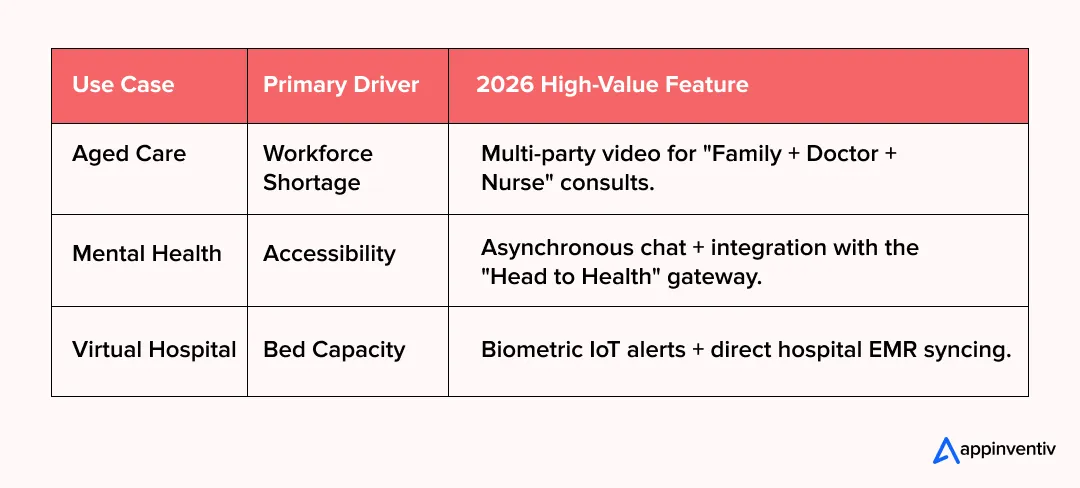
1. Virtual “Hospital in the Home” (HITH)
Public health districts, such as those in Queensland and NSW, have pioneered virtual HITH models to manage moderate-acuity patients at home. You should look at these as benchmarks for “High-Acuity Telehealth.”
2. Digital Mental Health Ecosystems
Mental health is the most established telehealth niche in Australia. Roughly 1 in 4 Australians who accessed mental health support in late 2024-2025 did so virtually.
3. Connected Aged Care Frameworks
With the 2026 “Aged Care Act” reforms, digital health is now considered basic infrastructure for facilities. You should view aged care as a prime market for integrated EMR and telehealth solutions.
Business and Clinical Benefits of Telehealth Platforms in Australia
The real value of telehealth app development lies in measurable gains across operational efficiency, clinician utilisation, and long-term cost control. When designed correctly, telehealth platforms improve care continuity while reducing system strain, making them a strategic investment rather than a tactical deployment. Some of the most remarkable benefits of telehealth applications include:
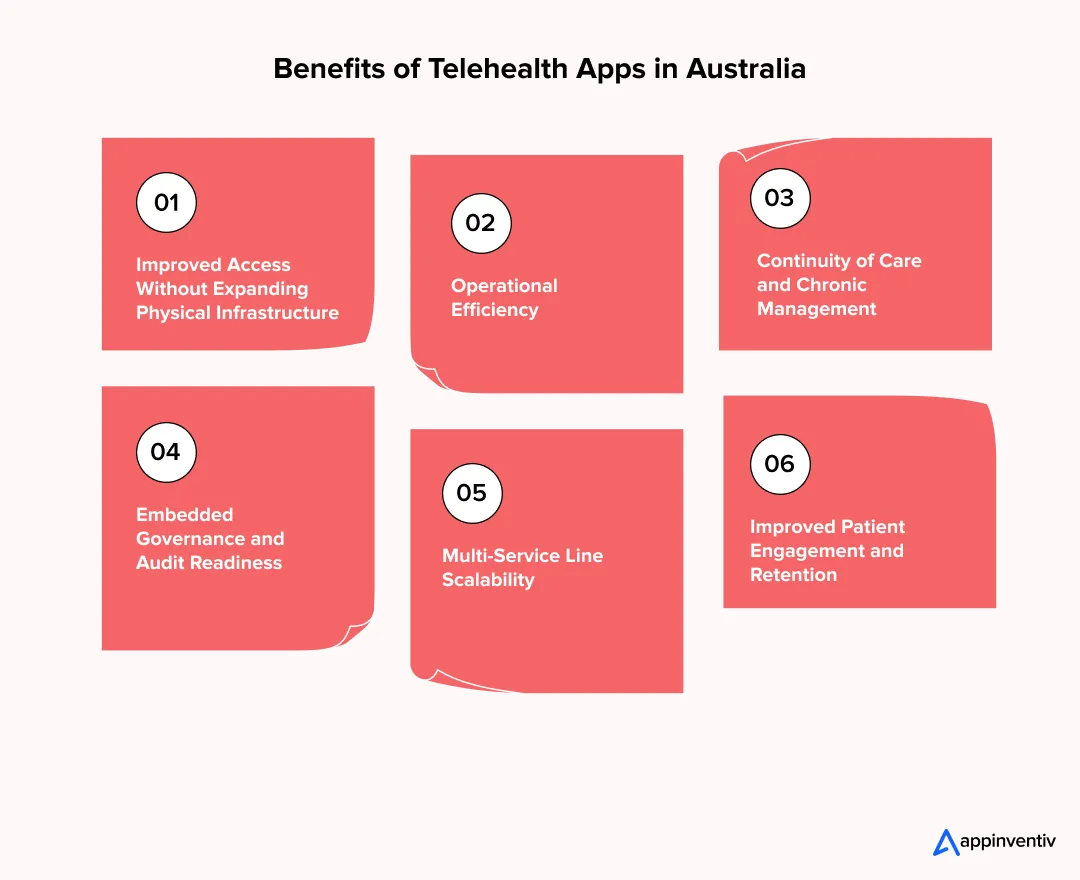
1. Improved Access Without Expanding Physical Infrastructure
Australian providers often struggle with geographic constraints that physical expansion can’t solve. Telehealth allows you to push services into regional MMM zones without the capital sink of new buildings.
2. Operational Efficiency
Telehealth platforms streamline scheduling, consultations, and follow-ups into a unified system. This reduces administrative overhead and improves appointment throughput.
3. Continuity of Care and Chronic Management
Traditional care models are episodic. Telehealth enables continuous engagement through follow-ups, remote monitoring, and digital communication. This is particularly relevant for chronic disease management, where ongoing interaction improves outcomes.
4. Embedded Governance and Audit Readiness
A well-engineered system bakes compliance into the architecture. Automated audit trails and role-based access make meeting Ahpra or Privacy Act requirements a background process. For enterprise boards, this reduces the manual reporting burden and drastically lowers the risk profile of the clinical operation.
5. Multi-Service Line Scalability
Once established, telehealth platforms can be extended across multiple service areas. Mental health, aged care, and specialist consultations can all operate within the same system framework. This scalability is a key advantage of digital health platform development in Australia.
6. Improved Patient Engagement and Retention
Digital access changes how patients interact with healthcare providers. Convenience, reduced wait times, and easier follow-ups contribute to higher satisfaction levels. Engaged patients are more likely to adhere to treatment plans and return for future consultations.
How Much Does It Cost to Develop a Telehealth App in Australia?
The cost to build custom telehealth app in Australia typically ranges between AUD 70,000 and AUD 700,000 or more. However, this is just a rough estimate. The actual cost of app development for Australian telehealth varies based on the compliance overhead, integration needs, and security infrastructure, feature complexity and so on.
Businesses that budget without accounting for these factors consistently underestimate total cost of ownership by 30-40%.
| Platform Tier | Estimated Cost (AUD) | What Is Included |
|---|---|---|
| Basic MVP | $70,000 – $150,000 | Video consult, scheduling, basic patient profile, core security |
| Mid-Level Platform | $150,000 – $400,000 | EHR integration, Medicare billing, analytics, mobile apps, full compliance layer |
| Enterprise Platform | $400,000 – $700,000+ | AI capabilities, multi-system integration, full audit framework, ongoing compliance tooling |
What Drives the Cost Up
The cost to build a custom telehealth app in Australia is shaped by several factors that are frequently underestimated in initial scoping:
- Compliance architecture adds 15-25% to development cost compared with a non-regulated platform of equivalent functional scope
- Integration complexity scales non-linearly; connecting to three or four different practice management systems, each at different API maturity levels, can double the integration budget
- AI capabilities add both build cost and significant ongoing compute cost that needs to be modelled in total cost of ownership projections
- Ongoing maintenance is a recurring cost commitment, which adds roughly 15-20% of your initial build cost annually.
- Using Australian-based cloud availability zones (like AWS Sydney) comes with a specific price point, especially when you add the “Zero Trust” security layers.
Our team can provide a structured cost breakdown based on your clinical requirements and compliance obligations.
Build vs Buy: What is the Right Approach for Telehealth Platform Adoption in Australia
Choosing the right approach impacts time-to-market, compliance readiness, and long-term cost of ownership. In Australia, where regulatory alignment and integration with national health systems are critical, this decision should be based on scalability, governance control, and execution risk rather than speed alone.
| Criteria | Build | Buy |
|---|---|---|
| When It Fits | Organisations with unique clinical workflows, multi-service delivery models, or long-term digital health infrastructure goals | Providers with standardised care models and limited integration or custom workflow requirements |
| Key Advantages | Full control over compliance architecture, data residency, and deep integration with My Health Record and Medicare systems | Faster deployment, predictable costs, minimal internal development overhead |
| Key Trade-offs | High upfront investment, longer delivery timelines, requires strong in-house governance and technical capability | Limited flexibility, potential misalignment with Australian compliance requirements, integration constraints with legacy systems |
| AU Compliance Risk Level | Low (if designed correctly with embedded compliance architecture from the outset) | Medium to High (depends on vendor alignment with Australian regulations and ability to support local compliance requirements) |
AI and Remote Monitoring: What Is Actually Production-Ready in Australia
The conversation around AI implementation in Australian healthcare has matured beyond chatbots. This shift is driven by a persistent healthcare workforce shortage and the need to manage chronic conditions more efficiently within the “Hospital in the Home” framework.
Here are the emerging AI capabilities in the Australian ecosystem:
AI-Assisted Virtual Triage
Modern platforms now use AI-driven intake bots to conduct initial clinical assessments. By the time a practitioner joins the video call, they are presented with a structured summary and a preliminary risk stratification.
For example, Australian insurers like nib have already begun integrating triage technology to guide members to the most appropriate care setting, effectively reducing unnecessary ED presentations.
Remote Patient Monitoring (RPM) & IoMT
RPM is no longer a niche for elite sports or clinical trials; it is a core operational requirement for chronic disease management. Integrating wearables (ECG, SpO₂, glucose monitors) with the platform allows for real-time data streaming into a central dashboard. Alerts are triggered only when metrics breach clinical safety ranges, significantly reducing “alert fatigue” for practitioners.
Predictive Analytics for Early Intervention
In Q2 2026, the most advanced AU platforms are utilising predictive models to detect subtle physiological declines before they become acute crises. These models analyse longitudinal data from My Health Record and connected IoT devices to identify patterns such as a specific combination of heart rate variability and respiratory changes that often precede hospital readmission.
Future Trends in Telehealth: Australia 2026 and Beyond
The Australian healthcare landscape is pivoting from reactive video calls to a “prevention-first” ecosystem. As we move toward 2030, the home will become the primary site for chronic disease management, supported by government-led “Hospital in the Home” (HITH) initiatives and integrated AI governance.
1. From Reactive to Proactive AI
The focus has shifted from administrative bots to “Agentic AI systems” capable of clinical orchestration. You should expect systems to move beyond simple triage into automated diagnostic support, which is already improving early detection rates for chronic conditions like heart disease by up to 64%.
2. The Unified National Medicines Record
Federal reforms are merging online prescribing with the My Health Record ecosystem. Future platforms will offer a “single source of truth” for medication history, ensuring every provider, from GPs to specialists, has a real-time, shared view of a patient’s active scripts and dispensing history.
3. “Hospital in the Home” as the Standard
State health departments (NSW and QLD) are rapidly scaling virtual ward models to manage moderate-acuity patients. Your platform must integrate with medical-grade wearables that stream continuous biometric data directly into hospital EMRs, effectively bypassing the need for physical bed occupancy.
4. Codified Clinical Governance
By 2027, governance will move from static manuals to live dashboards. Leading platforms will use “Proactive Governance” to track board-level KPIs such as data completeness and safety alert resolution, making compliance an automated, inseparable part of every consultation.
How Appinventiv Builds Compliant Telehealth Platforms in Australia
The Australian healthcare sector in 2026 demands more than just code; it requires a trusted healthcare software development company in Australia who understands the clinical gravity of a “Zero Trust” environment.
At Appinventiv, we don’t just build apps, we engineer high-performance clinical assets. Having delivered more than 3000 digital assets, including 500+ healthcare solutions, across the Australian landscape, our team of 1600+ tech architects brings 11+ years of APAC delivery experience to your project.
Our work with healthcare platforms like Health e People, DiabeticU, YouComm and Soniphi demonstrates our ability to handle complex biometric data and chronic disease management while maintaining a 99.50% security compliance SLA.
We ensure your platform isn’t just a siloed tool, but a connected node in the national grid. By bridging the gap between legacy Practice Management Systems and modern HL7 FHIR standards, we typically help our Australian enterprise clients achieve a 35% gain in operational efficiency.
With 5+ agile delivery centres across Australia, we provide the local oversight necessary to navigate Ahpra and TGA complexities. Our 90% client retention rate is a testament to our commitment to long-term clinical governance. Whether you are scaling a virtual hospital or a specialist niche, we provide the technical depth to turn your vision into a compliant, scalable, and commercially viable reality.
Planning telehealth app development in Australia? Start with a discovery engagement that maps your compliance obligations and integration requirements before committing to a build. Reach out to our team to get started.
FAQs
Q. What is telehealth app development in Australia?
A. Telehealth app development in Australia is the process of designing and building secure, clinically compliant digital platforms that enable remote consultations, integrate with national health infrastructure, including Medicare and My Health Record, and satisfy Australian regulatory requirements under the Privacy Act 1988, My Health Records Act 2012, and ADHA interoperability guidelines.
These platforms are not standalone applications. They function as extensions of the healthcare system, requiring interoperability, auditability, and clinical reliability.
Q. How long does it take to build a telehealth app in Australia?
A. A well-scoped MVP typically requires 3 to 6 months from discovery to production deployment. Mid-complexity platforms with EHR and Medicare integration usually run 6 to 9 months. Enterprise-grade platforms with AI capabilities and multi-system integration typically require 9 to 12+ months.
Q. How do you build a secure and compliant telehealth app in Australia?
A. To build a secure, compliant telehealth app in Australia, we architect for “Compliance by Design.”
- We start with a Zero Trust Architecture (ZTA) to verify every access request, neutralising the risk of a Notifiable Data Breach.
- We ensure all “Sensitive Information” must be hosted within Australian cloud regions (e.g., AWS Sydney) to satisfy APP 8 data residency requirements.
- For clinical interoperability, we implement HL7 FHIR protocols and SNOMED CT-AU terminology to ensure seamless data exchange with My Health Record.
- Finally, integrate myGovID for identity verification and automate MBS billing logic to meet strict 2026 Medicare and Ahpra regulatory standards.
Q. What are the biggest challenges in building a telehealth app in Australia?
A. The four most common challenge areas are:
- Regulatory complexity, best addressed through early compliance mapping rather than reactive remediation.
- Integration overhead with Australian health systems, including EHRs, Medicare, and My Health Record, which require careful API design and tolerance for legacy system variability.
- Rural connectivity requirements, which demand offline-first architecture that functions under poor or intermittent connections.
- Practitioner adoption, which is almost always a product design problem rather than a change management one. Platforms that mirror familiar clinical workflows and genuinely reduce administrative burden achieve the adoption rates that justify the investment.


- In just 2 mins you will get a response
- Your idea is 100% protected by our Non Disclosure Agreement.

Telehealth Business Ideas for 2026: Models, Technology Stack, and Growth Strategy
Key Takeaways Choose what people will keep using: The strongest telehealth models solve ongoing needs, not one-time problems. Integration matters more than features: Platforms that fit into real care workflows tend to scale without friction. Recurring care drives stable revenue: Chronic care, employer-led models, and guided programs create consistent usage. Partnerships accelerate growth: B2B and…
How Much Does EHR Software Development Cost? Enterprise Pricing, Hidden Costs, and ROI Analysis
Key Takeaways EHR implementation costs vary widely, from $20,000 for small clinics to $900,000+ for enterprise systems, based on scope, complexity, and customization. Whereas EHR software development costs between $30,000 to $1M+, depending on the complexity of development, choice of technologies and advanced features. Hidden costs like data migration, workflow disruption, training, and compliance can…

Key Takeaways Fitness app cost ranges from $40,000 to $400,000, based on features and scale Real cost includes build, scaling, maintenance, and integrations Business model drives backend complexity and overall pricing Strong retention matters more than downloads for ROI Early tech and monetization choices prevent costly rework If you’ve started putting numbers around your fitness…