- Types of EMR Software Every Healthcare Provider Should Know
- How to Build an EMR System That Actually Works
- Key Features of EMR Software Development
- Technology Stack Used in Developing EMR Systems
- What Does Custom EMR Software Development Really Cost?
- Compliances and Security Standards of EMR Development
- Challenges & Solutions of EMR Software Development and Implementation
- Applications of EMR System Development Across Healthcare Settings
- Benefits of Custom EMR System Development
- Future Trends of EMR Hospital Software Development
- How Appinventiv Supports EMR Software Development
Key takeaways:
- EMR software development is about removing daily friction, not just digitizing patient records.
- Custom EMR technology development supports long-term stability, especially for multi-location and enterprise healthcare networks.
- Cost ranges from $40,000 to $4,000,000, depending on the number of integrations, the depth of compliance, and system complexity.
- Enterprise EMR software implementation succeeds with strong planning, adoption strategy, and interoperability.
- Future-ready platforms combine secure architecture, scalability, and AI-powered EMR development capabilities.
Hospitals are not lacking software. Many systems simply no longer reflect how care actually works. Clinicians switch screens for basic tasks, billing teams recheck data, and leadership waits for clear numbers. In that context, EMR software development is about reducing daily friction, not just digitizing records.
Quick upgrades may seem easier, but they often create rigid workflows over time. Strategic custom EMR technology development allows teams to rebuild with a stronger structure and cleaner integration. When you build EMR software thoughtfully, it becomes a long-term stability move.
The broader healthcare market reflects this shift. Fortune Business Insights projects the global digital health market to reach nearly USD 492 billion in 2026, signaling sustained investment in electronic medical records software and advanced digital infrastructure.
As leaders evaluate how to create EMR software that supports growth, compliance, and innovation, the focus should remain grounded: build a system that works reliably for people today while remaining flexible enough for AI-powered EMR development and future expansion.
Replace fragmented systems with structured, scalable EMR software development built for clinical efficiency and long-term compliance.
Types of EMR Software Every Healthcare Provider Should Know
When healthcare leaders explore the different types of EMR software, the decision usually reflects the organization’s size, risk tolerance, and growth plans. There is no universally “best” structure. What works for a single specialty clinic may not hold up inside a multi-hospital network. The direction you take during EMR software development will influence how flexible the system feels five years from now, not just at launch.
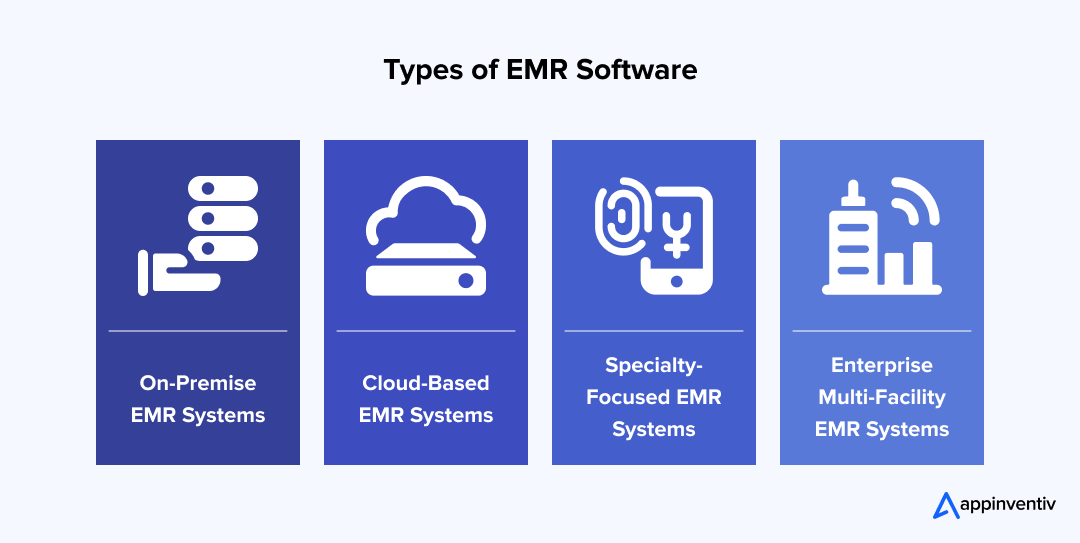
1. On-Premise EMR Systems
- Installed and managed within the hospital’s own infrastructure.
- Gives internal IT teams direct oversight of servers, storage, and security layers.
- Often chosen by organizations with strict internal compliance governance.
- Requires heavier upfront investment and ongoing hardware maintenance.
- Scaling usually means expanding physical infrastructure and internal resources.
Some institutions still prefer this route in healthcare EMR technology development when data control is a primary concern.
2. Cloud-Based EMR Systems
- Hosted on secure cloud environments rather than internal servers.
- Makes it easier to expand across locations without rebuilding infrastructure.
- Reduces the need for large in-house server management teams.
- Supports smoother updates and ongoing performance improvements.
- Frequently selected in modern EMR development projects focused on scalability.
For growing networks, this model often feels more practical and adaptable.
3. Specialty-Focused EMR Systems
- Built around the specific documentation and workflow patterns of a discipline.
- Includes templates and data fields tailored to clinical reality.
- Helps reduce unnecessary screens and manual adjustments.
- Often requires deeper customization during custom EMR software development.
When organizations think about how to create EMR software for focused services, specialty alignment can significantly improve clinician comfort.
4. Enterprise Multi-Facility EMR Systems
- Designed to support multiple hospitals, clinics, or care centers under one structure.
- Centralizes data while maintaining department-level controls.
- Requires strong integration planning and governance oversight.
- Demands experienced emr software developers due to system complexity.
This structure typically involves structured enterprise EMR software implementation and long-term architectural planning.
5. Modular or Hybrid EMR Systems
- Combines a core platform with optional modules that can be added over time.
- Allows phased adoption during EMR software implementation.
- Reduces the pressure of replacing every system at once.
- Helpful for organizations gradually modernizing fragmented tools.
Ultimately, choosing among the types of EMR software should feel deliberate rather than reactive. The model selected during EMR development will shape operational stability, integration effort, and overall custom EMR software development cost well beyond the initial deployment.
Also Read: EHR Software Development: A Complete Guide for 2025
How to Build an EMR System That Actually Works
When leaders ask how to build an EMR system, the instinct is to start listing features. In practice, successful EMR technology development begins with understanding daily clinical pressure. The system must support fast decision-making, accurate documentation, and clean billing data without slowing people down. Strong EMR development feels natural to users. If teams have to fight the system, something was missed early on.
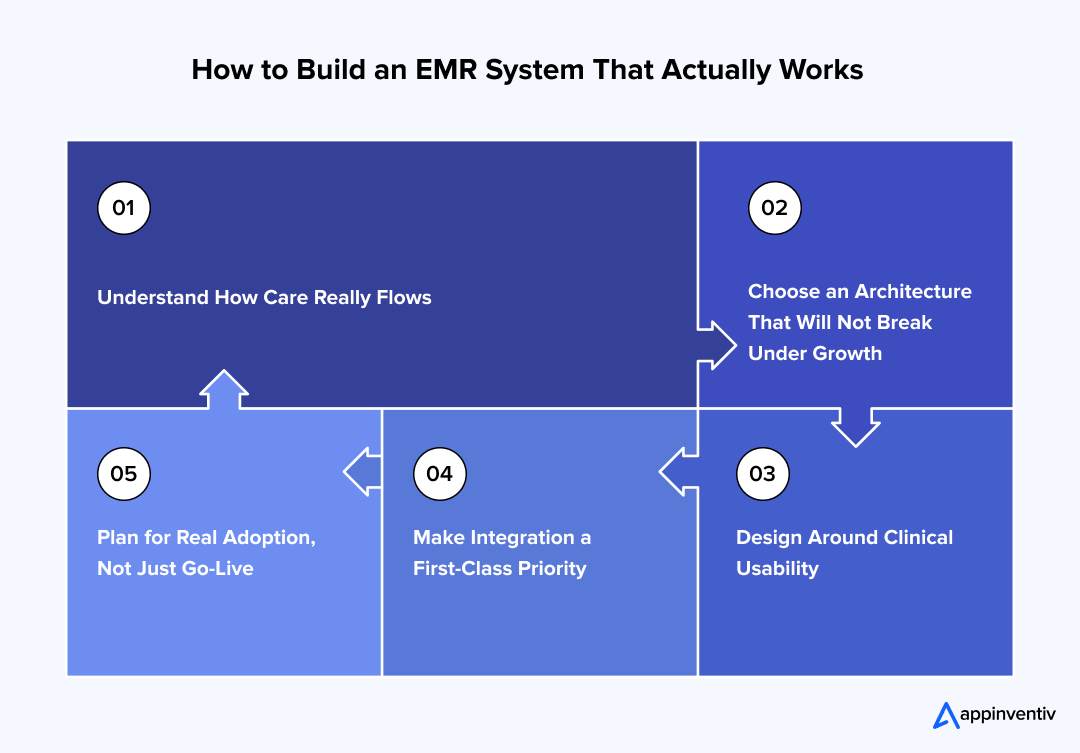
Step 1: Understand How Care Really Flows
Before writing code, spend time where care happens. Sit with clinicians. Watch how intake works. Review how claims move through billing. This discovery phase defines whether custom EMR technology development becomes a long-term asset or a recurring headache.
Focus areas should include:
- Real patient journey mapping from registration to discharge
- Specialty-specific documentation habits
- Coding and reimbursement dependencies
- Pain points that create delays or rework
When teams skip this step, they often rebuild the same inefficiencies in digital form.
Step 2: Choose an Architecture That Will Not Break Under Growth
Architecture is rarely visible to end users, but it determines performance and stability. When organizations decide to build EMR software, they must think about scale, not just launch day.
Important considerations include:
- Cloud or hybrid infrastructure based on projected growth
- Modular system design rather than rigid monolithic builds
- API-first planning to support interoperability
- Database structures that balance detailed records with reporting needs
Experienced EMR software developers know that long-term reliability matters more than short-term speed.
Step 3: Design Around Clinical Usability
A system may be technically advanced and still frustrate clinicians. Effective EMR development reduces clicks, simplifies templates, and keeps screens intuitive.
Core priorities often include:
- Specialty-driven documentation templates
- Streamlined e-prescribing workflows
- Smooth lab and imaging integration
- Revenue cycle alignment with billing teams
Electronic medical records software should make daily tasks easier, not heavier.
Step 4: Make Integration a First-Class Priority
Healthcare rarely operates in isolation. Labs, pharmacies, payers, and external providers all exchange data daily. Integrating EMR software in the healthcare industry requires structured planning, not quick connectors.
A strong integration plan addresses:
- HL7 and FHIR standards
- Secure API management
- Interface monitoring and error tracking
- Controlled third-party data access
Many EMR software implementation challenges surface here, which is why integration deserves early attention.
Step 5: Plan for Real Adoption, Not Just Go-Live
The technical launch is only one milestone. During enterprise EMR software implementation, change management determines long-term success.
Adoption planning should include:
- Phased rollouts by department or facility
- Internal champions and structured training programs
- Parallel validation before full transition
- Ongoing performance monitoring after launch
If you are exploring how to create EMR software for long-term sustainability, the Development Process of EMR Software must balance technical strength with human acceptance. Systems succeed when people trust them and rely on them without hesitation.
From architecture planning to enterprise EMR software implementation, build a platform designed for interoperability, performance, and growth.
Key Features of EMR Software Development
When healthcare leaders invest in EMR software development, the goal is rarely “more features.” It is usually something far more practical. They want doctors to finish notes before the next patient walks in. They want billing teams to spend less time fixing errors. They want fewer compliance headaches during audits.
Strong EMR system development supports daily work quietly in the background. The right features should feel natural, not technical.
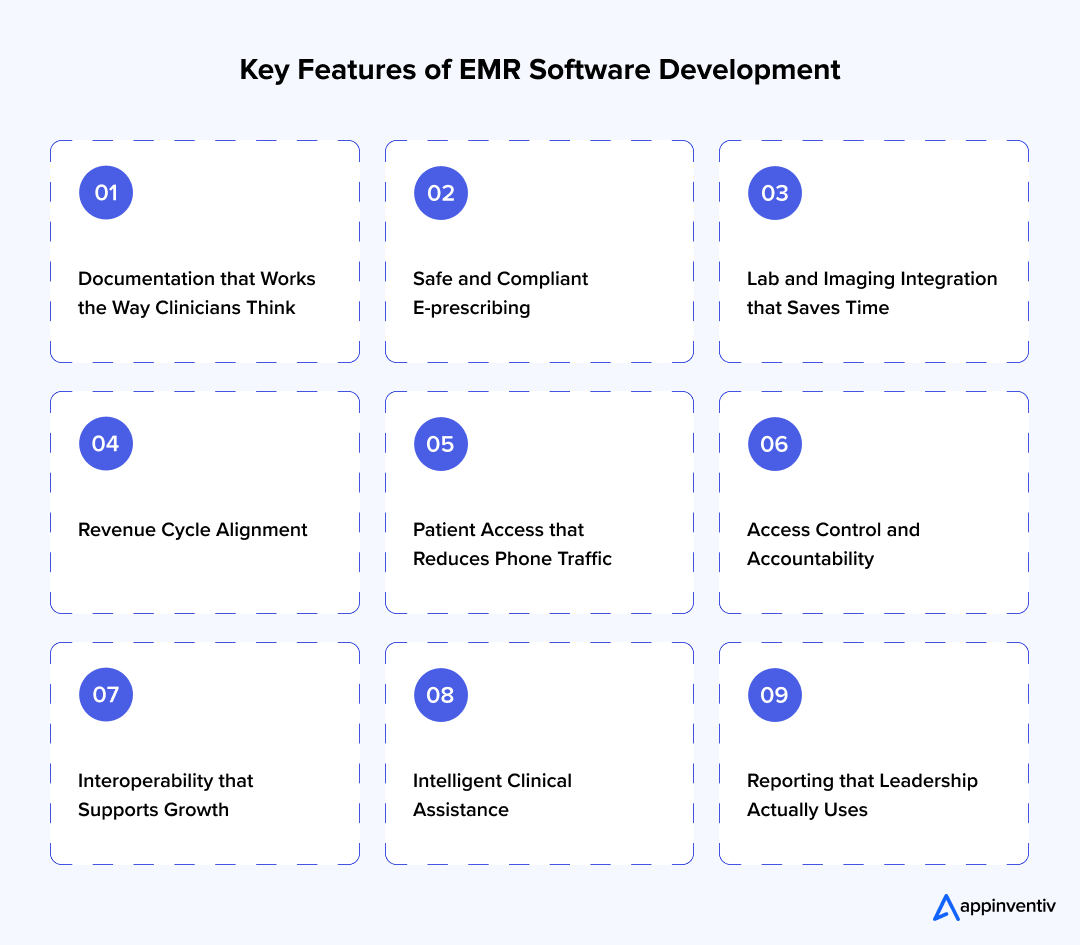
1. Documentation that Works the Way Clinicians Think
If teams decide to develop EMR software, documentation must come first. Poor note design slows everything down. A well-designed system offers:
- Specialty-based templates that match real workflows
- Smart suggestions that reduce repetitive typing
- Simple coding assistance for ICD and CPT
- Clean layouts that prevent clutter
Good documentation tools reduce after-hours charting. That alone changes clinician satisfaction.
Also read: The Power of AI in Intelligent Document Processing
2. Safe and Compliant E-prescribing
Medication errors are costly and dangerous. Reliable electronic medical records software includes:
- Drug interaction and allergy alerts
- Controlled substance safeguards
- Secure transmission logs
In HIPAA-compliant EMR development, every prescription action must be traceable. Security is built in, not layered on later.
3. Lab and Imaging Integration that Saves Time
Clinicians should not chase reports across systems. Practical custom EMR technology development ensures:
- Automatic syncing of lab results
- Clear abnormal result indicators
- Direct access to imaging reports
This is especially important when integrating EMR software in healthcare industry environments where multiple vendors are involved.
4. Revenue Cycle Alignment
One overlooked truth in EMR development is this: documentation quality affects revenue. Strong systems support:
- Automated charge capture
- Claim validation before submission
- Denial trend tracking
When clinical and billing workflows connect smoothly, organizations see fewer rejected claims and stronger financial control.
5. Patient Access that Reduces Phone Traffic
Patients now expect digital access. Modern healthcare EMR technology development includes:
- Secure portals for reports and prescriptions
- Online medical scheduling
- Messaging capabilities
- Telehealth support
These features become critical during enterprise EMR software implementation across multi-location networks.
6. Access Control and Accountability
Data protection cannot be vague. Enterprise-level systems include:
- Role-based permissions
- Detailed activity logs
- Encrypted storage and transmission
For enterprise EMR software development, audit trails are not optional. They protect both patients and institutions.
7. Interoperability that Supports Growth
Healthcare rarely operates in isolation. During enterprise EMR software implementation, systems must connect with:
- Labs and pharmacies
- Insurance platforms
- Billing and ERP systems
Without strong APIs and standards support, scalability becomes expensive.
8. Intelligent Clinical Assistance
With AI-powered EMR software development, systems begin to do more than store data. They can:
- Flag high-risk patients
- Suggest care pathways
- Identify readmission risk
These tools support faster decision-making while keeping clinicians in control.
9. Reporting that Leadership Actually Uses
Executives need clarity, not dashboards filled with noise. Well-designed systems provide:
- Operational performance metrics
- Revenue summaries
- Quality and compliance reports
That visibility transforms EMR technology development from a technical upgrade into strategic infrastructure.
Ultimately, custom EMR technology development succeeds when features support real work. The system should reduce friction, not introduce it. If clinicians barely notice the technology but feel their day runs more smoothly, the platform is doing its job.
Technology Stack Used in Developing EMR Systems
When people talk about EMR software development, the conversation usually focuses on features. Patient charts, billing, telehealth, analytics. But underneath all of that sits something far less visible: the technology stack.
That stack quietly decides whether the system feels reliable or frustrating. If a chart takes five seconds to open instead of one, clinicians notice immediately. If integrations fail between labs and the EMR, operations slow down. So the technology choices behind an EMR platform are less about trends and more about stability.
Below is the kind of stack most modern EMR platforms are built on.
1. Backend Technologies
The backend is the operational core of the system. It processes patient data, manages permissions, and connects the EMR to outside systems such as labs, imaging tools, and insurance platforms.
Most healthcare platforms rely on technologies that have been tested for years rather than newer frameworks.
- Java (Spring Boot) remains common in enterprise healthcare systems because it handles large workloads reliably.
- .NET Core is widely used in hospitals already operating within Microsoft enterprise environments.
- Node.js works well when systems rely heavily on APIs and real-time data exchange.
- Python frameworks such as Django or FastAPI often appear in analytics modules or AI-powered clinical tools.
None of these technologies is flashy. That is usually a good sign in healthcare systems.
2. Frontend Layer
Doctors and nurses spend hours inside EMR interfaces. If the system feels slow or cluttered, frustration shows up quickly. That is why modern EMR platforms rely on frontend technologies that keep screens responsive.
Common frameworks include:
- React.js, widely used for dynamic dashboards and modular clinical interfaces
- Angular, often chosen for large enterprise systems that need strict structure
- Vue.js, a lightweight option that works well for patient portals or telehealth modules
The real goal here is simple. Clinicians should reach the information they need without digging through multiple screens.
3. Database and Data Storage
EMR systems store years of patient history. Prescriptions, imaging references, treatment notes, billing records, and lab reports. The database layer must handle all of that without slowing down.
Most platforms combine a few different technologies:
- PostgreSQL for structured clinical records
- MySQL for scalable transactional data
- MongoDB when flexible record structures are needed
- Redis for caching frequently accessed information, so charts load faster
Large hospital networks often run multiple database layers together to balance speed and long-term storage.
4. Interoperability Standards
Healthcare software almost never runs alone. Patient information constantly moves between systems: laboratories, imaging platforms, insurance networks, and pharmacies.
To make that possible, EMR systems rely on a few widely accepted standards:
- HL7, the long-standing healthcare messaging standard
- FHIR, a newer API-driven framework designed for easier data exchange
- DICOM, which handles medical imaging files such as radiology scans
Without these standards, connecting healthcare systems would become extremely complicated.
5. Cloud Infrastructure
Many EMR platforms now run on cloud infrastructure rather than internal hospital servers. This makes it easier to scale systems across locations while maintaining uptime.
Common cloud environments include:
- Amazon Web Services (AWS)
- Microsoft Azure
- Google Cloud Platform
These platforms provide secure hosting, automated backups, and disaster recovery capabilities, all of which are important when patient data must remain accessible around the clock.
6. Security and Compliance Technologies
Security runs through every layer of an EMR system. Healthcare platforms handle some of the most sensitive data that organizations store.
To protect that information, most systems rely on several core safeguards:
- AES-256 encryption for stored data
- TLS protocols for secure data transmission
- OAuth 2.0 authentication frameworks
- Multi-factor authentication for privileged access
- Security monitoring tools that flag unusual activity
These controls help organizations meet regulatory standards such as HIPAA while still allowing clinicians to access patient information quickly when needed.
When the technology stack is chosen carefully, it rarely draws attention. The system simply works. Records load quickly, integrations run quietly in the background, and clinicians focus on patients rather than software.
That is usually the real sign that the EMR software development foundation was built correctly.
What Does Custom EMR Software Development Really Cost?
Cost is usually the first serious question leadership asks. Not because they want the cheapest option, but because they need clarity. The reality is simple. Custom EMR technology development costs depend on scope, integrations, the depth of compliance, and the number of workflows the system must support. A single-clinic platform will not cost the same as a multi-hospital network solution.
Below is a practical breakdown to help frame expectations.
Cost Range by Project Complexity
Here is the cost breakdown by project complexity level:
| Project Level | Typical Scope | Timeline | Cost Range |
|---|---|---|---|
| Basic / MVP EMR | Core documentation, scheduling, basic billing, and limited integrations | 4–6 months | $40,000 – $120,000 |
| Mid-Level EMR | Multi-department workflows, lab integration, patient portal, and advanced billing | 6–9 months | $120,000 – $400,000 |
| Enterprise EMR Platform | Multi-location support, complex integrations, AI modules, and advanced compliance controls | 9–18+ months | $400,000 – $4,000,000 |
Cost Breakdown by Development Phase
Here is the cost breakdown by development phase level:
| Development Phase | What Happens Here | Budget Allocation (%) |
|---|---|---|
| Discovery & Planning | Workflow analysis, compliance planning, and technical architecture | 10–15% |
| UI/UX Design | Interface design for clinicians and staff | 10–15% |
| Core Development | Module engineering, integrations, and database setup | 35–45% |
| Compliance & Security Implementation | Encryption, access control, audit trails, HIPAA alignment | 10–15% |
| Testing & Validation | QA, clinical UAT, performance testing | 10–15% |
| Deployment & Training | Go-live, onboarding, hypercare support | 5–10% |
What Drives the Cost Up or Down?
Several factors influence final investment:
- Number of integrations (labs, pharmacies, insurance, ERP systems)
- Level of AI-powered functionality
- Data migration volume
- Compliance documentation and audit readiness
- Custom workflow complexity
Organizations planning large-scale enterprise EMR software implementation should also factor in long-term maintenance, hosting, upgrade cycles, and ongoing security monitoring.
ROI of Implementing Custom EMR Software
When hospitals discuss the cost of custom EMR software, the conversation usually starts with the budget. But in practice, most leadership teams care more about what the system changes after it goes live.
In many organizations, a lot of time is lost in small ways. Doctors finish patient visits but still have notes waiting at the end of the day. Billing teams often correct missing details before claims go out. Administrators sometimes struggle to get clear operational numbers without digging through multiple systems.
A well-built EMR tends to ease those everyday pressures.
Over time, organizations usually notice a few changes:
- Fewer claim denials, because documentation and billing stay aligned
- Less after-hours charting, which helps clinicians finish records during the day
- More reliable billing data, reducing the amount of manual corrections
- Better coordination between departments, so staff spend less time tracking information
- Clearer reporting, making it easier for leadership to understand what is happening across the system
The impact rarely appears in a single moment. It builds gradually as teams come to rely on the platform every day.
That is where the ROI of implementing custom EMR software becomes visible. The system begins to remove small operational headaches, and those small improvements eventually translate into measurable efficiency and financial stability.
Compliances and Security Standards of EMR Development
Compliance in healthcare is rarely about passing an audit once. It is about building a system that protects patient data every single day.
In serious EMR software development, security is not an afterthought. It shapes architecture, access rules, hosting decisions, and even UI behavior from the beginning.
Below are the standards and practices that define responsible EMR system development.
1. HIPAA Compliance (For US Healthcare Systems)
For organizations operating in the United States, a HIPAA-compliant EMR system is non-negotiable. This includes:
- Role-based access control with clearly defined permissions
- Encryption of data at rest and in transit
- Detailed audit logs tracking user activity
- Secure hosting environments with signed Business Associate Agreements (BAAs)
- Regular risk assessments and vulnerability testing
HIPAA is not just a checklist. During enterprise EMR software implementation, compliance must be documented, monitored, and continuously reviewed.
2. Data Encryption and Secure Infrastructure
Strong enterprise EMR technology development ensures:
- AES-256 encryption for stored data
- TLS/SSL protocols for data transmission
- Secure cloud environments with isolation controls
- Multi-factor authentication for administrative access
Security should never slow down clinicians. The system must balance protection with usability.
3. Role-Based Access and Least-Privilege Design
In healthcare, not everyone should see everything. Effective healthcare EMR technology development limits data exposure by:
- Assigning permissions based on job role
- Restricting administrative overrides
- Logging all record access and edits
- Implementing emergency “break-glass” protocols
This reduces insider risk and strengthens audit defensibility.
4. Audit Trails and Monitoring
Every interaction within the system should leave a trace. A secure Custom-built EMR systems framework includes:
- Timestamped activity logs
- Record-level change tracking
- Automated anomaly detection
- Regular audit reviews
During investigations or compliance reviews, this visibility becomes critical.
5. Interoperability Security Controls
When integrating EMR software in healthcare industry ecosystems, external connections introduce new risks. Security standards must cover:
- Secure API authentication
- Token-based access
- Data exchange validation
- Vendor risk assessments
Interoperability without secure controls exposes compliance.
6. Disaster Recovery and Business Continuity
Downtime in healthcare affects patient safety. Enterprise-level systems include:
- Automated encrypted backups
- Geo-redundant infrastructure
- Defined recovery time objectives (RTO)
- Offline documentation workflows
In enterprise EMR software implementation, continuity planning is as important as feature development.
7. Ongoing Compliance Governance
Compliance is not static. Regulations evolve, and threat landscapes change. Sustainable EMR development includes:
- Scheduled security audits
- Patch management protocols
- Continuous monitoring tools
- Policy documentation updates
Security maturity is measured by consistency, not promises. Strong EMR technology development treats compliance and security as operational foundations. When designed properly, they protect patients, reduce legal exposure, and build trust across the organization.
Challenges & Solutions of EMR Software Development and Implementation
Most organizations assume the difficult part is building the platform. In reality, the real complexity often begins during EMR software implementation. Technology rarely fails on its own. Execution, adoption, and integration gaps are what slow projects down.
Here are the most common challenges in emr system development, along with grounded solutions that work in real environments.
1. Resistance to Change
Healthcare teams operate under pressure. When a new system changes documentation flow or billing steps, even small adjustments can feel disruptive.
What helps: Involve clinicians early in the development process of EMR Software, run workflow simulations before launch, and identify internal champions who support peers during rollout. Adoption improves when users feel heard, not instructed.
2. Workflow Disruption During Go-Live
Even well-designed platforms can temporarily slow productivity. Charting may take longer in the first few weeks. Staff double-check every step.
What helps: Phased rollouts instead of big-bang deployment, structured hypercare support, and leadership visibility during early stabilization. Enterprise EMR software implementation works best when performance expectations are realistic.
3. Interoperability Complexity
Integrating EMR software in healthcare industry ecosystems is rarely simple. Labs, pharmacies, billing platforms, and insurers all require clean data exchange.
What helps: API-first architecture, early interface testing, and continuous monitoring. Interoperability in healthcare must be planned during architecture design, not added later.
4. Data Migration Risk
Legacy systems often contain inconsistent formatting, duplicate patient records, or incomplete data. Migrating that data into a new system can introduce confusion if not handled carefully.
What helps: Structured data audits, defined mapping rules, and clinical validation before full transfer. Clean data protects trust in the new system.
Also read: Cloud Data Migration Strategy and Best Practices
5. Compliance and Security Pressure
Healthcare organizations operate under strict regulatory standards. During transition periods, vulnerabilities can surface if controls are not aligned with HIPAA-compliant EMR software development principles.
What helps: Role-based access configuration before launch, documented audit trails, and security testing prior to go-live. Security must evolve alongside development.
6. Budget and Scope Creep
As stakeholders see progress, new feature requests naturally emerge. Without governance, this expands timelines and increases cost.
What helps: Clear milestone planning, phased enhancement roadmaps, and disciplined change management. Structured oversight protects both delivery and budget.
7. Measuring Impact After Launch
Some teams complete Custom-built EMR systems but struggle to quantify results. Without baseline metrics, it becomes difficult to evaluate success.
What helps: Define performance indicators before launch, then measure documentation time, denial rates, and operational efficiency consistently after deployment.
Successful EMR technology development is not defined by feature count. It is defined by preparation, governance, and realistic rollout planning. When organizations anticipate challenges early, implementation becomes more controlled than reactive.
Applications of EMR System Development Across Healthcare Settings
When organizations invest in EMR software development, they are usually trying to address a practical problem. Notes take too long. Reports get lost between systems. Billing feels disconnected from clinical work.
The way applications of the EMR system development appear depends on where the system is used. A hospital does not operate like a small clinic. A diagnostic center does not move like a long-term care facility. The system has to fit the place’s rhythm.
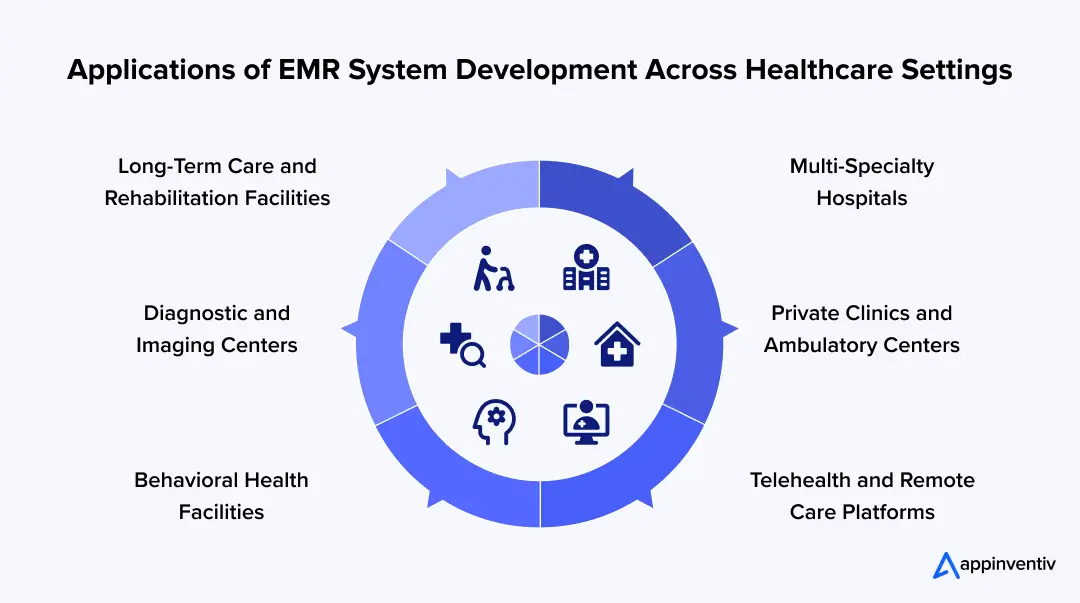
1. Multi-Specialty Hospitals
Hospitals are layered environments. Emergency teams move quickly. Surgical units plan carefully. Outpatient departments balance volume and detail. In these settings, enterprise EMR software development needs to:
- Let departments work differently without breaking coordination
- Provide fast access to labs and imaging
- Keep discharge planning organized
- Maintain a shared patient view across teams
If the system slows down one department, everyone feels it. Stability matters more than complexity.
2. Private Clinics and Ambulatory Centers
Clinics focus on steady patient flow. Appointments run back-to-back. Staff handles multiple tasks at once. Here, custom EMR solutions for hospitals and clinics often emphasize:
- Straightforward note templates
- Clear scheduling visibility
- Reliable billing workflows
- Fewer manual follow-ups
Small inefficiencies stand out quickly in smaller practices. Simplicity makes a difference.
3. Telehealth and Remote Care Platforms
Virtual care changed expectations. Providers now switch between in-person and digital visits within the same day. Through careful healthcare EMR software development, organizations can:
- Document virtual visits without duplicate entry
- Allow secure remote access
- Keep records consistent across channels
- Maintain compliance standards outside physical facilities
Patient Remote care highlights the importance of secure data exchange.
4. Behavioral Health Facilities
Behavioral health often relies on detailed notes and sensitive information. Privacy carries extra weight in these environments. Strong EMR system development supports:
- Flexible documentation styles
- Treatment tracking over extended periods
- Controlled access permissions
- Clear historical views of patient progress
When confidentiality is handled carefully, patient trust remains intact.
5. Diagnostic and Imaging Centers
These centers operate at a different pace. Reports move quickly, and physicians expect results without delay. Integrating EMR software in healthcare industry workflows helps by:
- Automatically uploading test results
- Connecting imaging systems directly
- Reducing manual communication steps
- Improving turnaround time visibility
Efficiency here directly affects clinical decision-making.
6. Long-Term Care and Rehabilitation Facilities
Long-term facilities focus on continuity. Care plans evolve gradually, not overnight. Scalable EMR platform development in these environments often supports:
- Ongoing medication monitoring
- Care coordination across multiple providers
- Clear documentation for compliance reviews
- Longitudinal patient history tracking
The system becomes part of routine care rather than a short-term project. Across all these settings, EMR technology development works best when it reflects how people already operate. Healthcare teams move differently depending on their environment. The system should adapt to that reality rather than forcing uniform processes. When the fit is right, the platform supports care quietly in the background.
Benefits of Custom EMR System Development
When organizations move toward Custom-built EMR systems, they are usually trying to solve everyday frustrations. Notes are taking too long. Billing teams are chasing corrections. Leadership lacks clear visibility. The benefits show up in small improvements that add up over time.
Here is what that often looks like in practice:
- Smoother clinical documentation: Providers spend less time navigating screens and more time focused on patients.
- Fewer billing surprises: Cleaner documentation supports accurate coding, which helps reduce claim rejections and payment delays.
- Better coordination across teams: Shared records reduce redundant testing, duplicate questions, and miscommunication between departments.
- More reliable data: Structured templates and validation checks lower the chance of incomplete or inconsistent records.
- Room to grow: Thoughtful enterprise EMR software development supports expansion into new locations without constant rework.
- Stronger compliance footing: Alignment with HIPAA-compliant EMR software development standards provides clarity during audits and reviews.
- Clearer operational insight: Built-in reporting helps leadership understand performance without having to dig through scattered spreadsheets.
- Less administrative strain: Automated reminders, scheduling workflows, and structured processes reduce repetitive manual tasks.
- Better long-term control over costs: While custom EMR software development cost varies, tailored systems often replace multiple disconnected tools and reduce hidden inefficiencies.
Well-executed EMR technology development does not change healthcare overnight. Instead, it makes daily operations steadier, clearer, and easier to manage.
Future Trends of EMR Hospital Software Development
Healthcare technology rarely changes overnight. It shifts gradually, shaped by real frustrations inside hospitals and clinics. Providers want fewer clicks. Administrators want clearer numbers. Patients expect easier access.
Here is where EMR technology development is heading.
- Systems that assist, not just record: Instead of acting like digital filing cabinets, newer platforms are beginning to highlight potential risks or missing details. AI-powered EMR software development is slowly becoming part of everyday decision support, without taking control away from clinicians.
- Voice becoming part of documentation: Typing long notes at the end of a busy day is exhausting. Voice technology is helping reduce screen time and making documentation feel less mechanical.
- Cleaner connections between systems: Hospitals are pushing for better communication between labs, insurers, pharmacies, and internal departments. Stronger interoperability means fewer phone calls and fewer repeated tests.
- Cloud infrastructure that grows with demand: As patient volumes increase, a scalable EMR platform enables systems to expand without constant technical overhauls.
- Reporting that makes sense: Leadership teams do not need more dashboards. They need clearer signals. Future systems focus on showing what matters rather than flooding teams with data.
- Stronger security habits: With rising cyber threats, enterprise EMR software development is placing more attention on continuous monitoring and controlled access.
- More natural patient interaction: Patients expect digital access to feel simple. Appointment booking, record viewing, and messaging are becoming smoother and more direct.
The direction of future trends of EMR hospital software development is not about adding layers of complexity. It is about removing small daily frustrations and making care delivery feel steadier and more connected.
Also Read: Top Healthcare Trends to Leverage in 2026
Prepare for AI-powered EMR software development, stronger integrations, and evolving compliance standards with a system designed to scale.
How Appinventiv Supports EMR Software Development
Every healthcare organization runs a little differently. Some struggle with documentation delays. Others deal with fragmented systems that do not communicate well. When teams begin planning EMR software development, those realities shape the build’s direction.
Through its custom healthcare software development services, Appinventiv works alongside healthcare teams to understand daily workflows before writing a single line of code. The conversations usually start with practical questions. Where does documentation slow down? Which integrations fail most often? What compliance pressure feels hardest? From there, the focus stays on building a system that supports real operations rather than adding complexity.
Integration is handled with the same mindset. Strong EMR integration solutions connect labs, billing platforms, telehealth systems, and internal tools so teams don’t constantly switch screens. Projects like YouCOMM Health, built to improve communication between patients and hospital teams, and Soniphi Vitality Health App, designed around structured health tracking and monitoring, reflect how thoughtful development can simplify coordination without compromising security.
If you are considering how to create EMR software that fits your environment instead of reshaping it, this is usually where the discussion begins. Let’s Talk!
FAQs
Q. What is EMR software development?
A. EMR technology development is the process of designing and building digital systems that manage patient records, documentation, billing, and clinical workflows.
It goes beyond storing data. It includes integrations, compliance planning, security controls, and long-term scalability. In larger organizations, enterprise EMR software development also covers structured rollout and governance planning.
Q. How long does electronic medical records software development take?
A. The timeline for electronic medical records software development depends on the scope.
- Basic system: around 4–6 months
- Mid-level system: 6–9 months
- Enterprise-scale platform: 9–18 months or more
Integrations, data migration, and AI-powered EMR software development features can extend timelines. Clear planning during the Development Process of EMR Software helps prevent delays.
Q. What is the total cost to develop a custom EMR system for a hospital network?
A. The Custom EMR software development cost typically ranges from $40,000 to $4,000,000, depending on complexity. Large networks requiring scalable EMR platform development, deep integrations, and full enterprise EMR software implementation fall toward the higher end. Ongoing maintenance and infrastructure should also be included in budgeting.
Q. Build vs buy EMR software – which is better?
A. When organizations choose to build EMR software, they gain flexibility and deeper workflow alignment. Off-the-shelf systems may be faster to deploy, but can limit customization. Custom EMR software development is often preferred when specialized clinical processes are required.
Q. How do modern EMR systems ensure secure clinical data sharing?
A. Modern healthcare EMR technology development protects data through:
- Role-based access controls
- Encrypted storage and transmission
- Secure API integrations
- Continuous monitoring and audit logs
Properly structured HIPAA-compliant EMR software development ensures that patient information remains protected while still supporting collaboration across departments and systems.
Q. What are some real-world examples of EMR systems used in healthcare?
A. Several EMR platforms are widely used across hospitals and clinics. Epic Systems is common in large hospital networks and academic medical centers. Cerner Corporation (now part of Oracle Corporation) supports many hospital and government healthcare systems. For clinics and ambulatory practices, cloud-based platforms like Athenahealth and eClinicalWorks are widely used to manage patient records, billing, and clinical workflows.


- In just 2 mins you will get a response
- Your idea is 100% protected by our Non Disclosure Agreement.

Telehealth Business Ideas for 2026: Models, Technology Stack, and Growth Strategy
Key Takeaways Choose what people will keep using: The strongest telehealth models solve ongoing needs, not one-time problems. Integration matters more than features: Platforms that fit into real care workflows tend to scale without friction. Recurring care drives stable revenue: Chronic care, employer-led models, and guided programs create consistent usage. Partnerships accelerate growth: B2B and…
How Much Does EHR Software Development Cost? Enterprise Pricing, Hidden Costs, and ROI Analysis
Key Takeaways EHR implementation costs vary widely, from $20,000 for small clinics to $900,000+ for enterprise systems, based on scope, complexity, and customization. Whereas EHR software development costs between $30,000 to $1M+, depending on the complexity of development, choice of technologies and advanced features. Hidden costs like data migration, workflow disruption, training, and compliance can…

Key Takeaways Fitness app cost ranges from $40,000 to $400,000, based on features and scale Real cost includes build, scaling, maintenance, and integrations Business model drives backend complexity and overall pricing Strong retention matters more than downloads for ROI Early tech and monetization choices prevent costly rework If you’ve started putting numbers around your fitness…