- The Pediatric Clinical Gap: Why "Generic" Fails
- How to Build a Pediatric EMR and EHR System?
- Key Features of Pediatric EMR and EHR Systems
- Key Technologies and Considerations in EHR Integration for Pediatric Practices
- Challenges in Building Pediatric EMR and EHR Systems
- Cost Considerations for Custom Pediatric EMR and EHR System Development
- How Appinventiv Can Help Build Your Custom Pediatric EMR and EHR Solution?
- FAQs
Key takeaways:
- Clinical Precision: Custom systems accommodate pediatric-specific data points like percentile curves and weight-based longitudinal dosing.
- Interoperability: Seamless data exchange via HL7 FHIR ensures your practice stays connected to pharmacies, labs, and state registries.
- Regulatory Resilience: Built-in compliance with HIPAA, HITECH, and MACRA/MIPS reduces legal friction.
- Enhanced Engagement: Parent portals reduce administrative overhead by automating routine queries and scheduling.
In pediatric care, the medical record is more than documentation. It supports medication safety, immunization tracking, growth interpretation, and communication with families. While most physicians use electronic records today, in pediatric practices, many pediatricians still don’t fully use EHR systems, leaving many clinicians without software optimized for child-specific workflows.
That is why pediatric EMR software development is not simply a technology upgrade. Pediatric workflows require built-in logic for growth percentiles, immunization lifecycle management, weight-based dosing, adolescent privacy transitions, and parent or guardian proxy access. These elements influence clinical safety, reporting accuracy, and daily efficiency.
At scale, expectations expand further. A modern pediatric patient management system must integrate with labs, pharmacies, registries, and hospital networks while supporting role-based access, audit trails, consent management, and governance controls. The system becomes part of the operational infrastructure, not just a clinical tool.
This blog explains how enterprise teams approach pediatric EMR and EHR system development, so organizations can implement custom pediatric EHR software that performs reliably in real clinical environments.
Ready to join them? Build your custom pediatric EMR/EHR system with Appinventiv.
The Pediatric Clinical Gap: Why “Generic” Fails
In pediatric care, the medical record is a longitudinal safety tool. Most off-the-shelf EHRs are built on adult medicine frameworks, essentially “billing-first” systems. However, pediatric clinicians operate in a world of weight-based calculations, proxy consent, and developmental milestones.
At an enterprise scale, a pediatric EMR is not just a digital filing cabinet; it is a high-stakes decision support engine. Custom development allows practices to own their IP and data pipeline while eliminating the “workarounds” that lead to clinical burnout.
How to Build a Pediatric EMR and EHR System?
To build a pediatric EMR and EHR system that performs in production, you need more than feature lists. You need a controlled build process that makes clinical workflows explicit, makes risk measurable, and makes interoperability in healthcare predictable.
The steps below follow a delivery approach that works for enterprise-grade healthcare software businesses while staying practical for pediatric clinic realities.
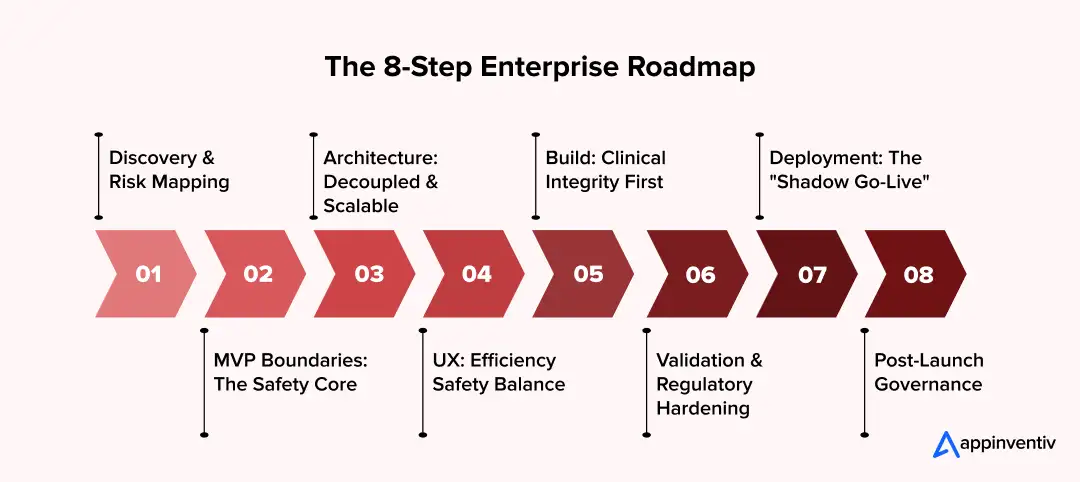
Step 1: Discovery & Risk Mapping
Discovery fails when it stops at “requirements.” In pediatric environments, success depends on whether you capture the non-obvious workflows and safety controls early, before design decisions lock you into rework.
What to do in this phase:
- Map pediatric care workflows by visit type: well-child, immunization-only, acute visits, chronic condition follow-ups, developmental screening, and care coordination.
- Document pediatric safety dependencies: weight-based dosing logic, allergy handling, contraindications, and standardized growth chart interpretation.
- Define family access models: parent or guardian proxy, multi-caregiver households, and controlled access transitions as adolescents mature.
- Confirm operational governance: who approves template changes, who controls clinical content, how new workflows are introduced, and how exceptions are handled.
Enterprise-grade output you should expect:
- A workflow map for clinical, administrative, and family experience pathways.
- A risk register with mitigation controls that translate into product requirements.
- A “decision rights” model for ongoing configuration and change control.
- An integration inventory that includes required exchange partners and data flows.
This is also the point where you decide whether you are building a system to replace an existing EHR or building a net-new system. Migration complexity changes nearly every downstream decision.
Enterprise Note: Map clinical risks, not just clicks. Identify where manual weight conversion could lead to dosing errors. Create a Clinical Safety Matrix.
Also Read: EHR vs EMR in Healthcare: Key Differences
Step 2: MVP Boundaries: The Safety Core
MVP planning in healthcare is not about shipping a stripped product. It is about shipping a product that can safely carry clinical workflows without creating shadow processes.
A pragmatic MVP for EHR software development for pediatrics typically includes:
- Structured pediatric charting with configurable templates for common visit categories.
- Growth chart tracking with percentile visibility and longitudinal trend views.
- Immunization management workflows and reminder logic that fit practice operations.
- Medication workflows with weight-based dosing support and safety checkpoints.
- A minimal parent-facing layer that reduces inbound administrative load and improves follow-through.
What not to do in MVP:
- Before your data model and workflow capture are stable, avoid bundling advanced analytics, AI decision support, and deep automation.
- Avoid over-indexing on UI polish without proving end-to-end workflows and integrations.
Your MVP is successful when it reduces staff friction and supports clinicians without forcing workarounds. That is the standard you should hold.
Enterprise Note: An MVP must include weight-based dosing, immunization tracking, and age-specific templates.
Step 3: Architecture: Decoupled & Scalable
Architecture is where many initiatives quietly accumulate debt. In pediatric workflows, the real risk is not “slow software.” It is mis-modeled clinical concepts that become expensive to fix once adoption begins.
For the technology stack for pediatric EMR and EHR development, the “right” answer depends on your constraints, but the decision framework stays consistent.
Key architecture decisions:
- Deployment model: cloud, on-premise, or hybrid based on governance, integration environment, and internal IT posture.
- Modularity: separate clinical core, family portal, integrations, and reporting pipelines, so changes do not break the whole system.
- Auditability and traceability: treat audit logs, event trails, and role-based access as core architecture, not afterthoughts.
- Interoperability strategy: design for standardized exchange rather than one-off point integrations.
Data model requirements that matter in pediatrics:
- Growth observations that support time series analysis and percentile interpretation.
- Immunization events that include schedule logic, consent, and provenance.
- Medication and dosing logic that respects pediatric variability.
- Family relationships and proxy access rules that withstand operational edge cases.
If the data model is wrong, every downstream feature becomes fragile. That is why architecture and clinical informatics alignment must happen early.
Enterprise Note: We recommend a Microservices Architecture. Update the “Parent Portal” without touching the “Prescription Engine,” ensuring zero clinical downtime.
Step 4: UX: Efficiency-Safety Balance
UX in clinical systems is a throughput decision. Poor UX does not just irritate users. It increases documentation time, slows visit flow, and pushes staff into parallel workflows.
A pediatric system also has multiple user contexts:
- Clinicians need speed, structured capture, and safety cues.
- Front desk and billing staff need clean scheduling, eligibility cues, and documentation completeness.
- Parents need clarity, minimal friction, and trusted communication.
What enterprise teams should insist on:
- Role-based interfaces with task-driven navigation.
- Minimal clicks for common pediatric visit patterns.
- Guardrails that feel supportive, not obstructive, especially for dosing and immunizations.
- Mobile-first parent experience design because families operate on phones.
This is not the stage for opinion-based design. Prototype key workflows, test them with real users, and let usage patterns drive decisions.
Enterprise Note: Prioritize high-density data for clinicians and mobile-first, jargon-free interfaces for parents.
Step 5: Build: Clinical Integrity First
In pediatric electronic medical record software development, the build phase should prioritize clinical integrity and operational reliability over breadth.
Build a sequence that reduces rework:
- Clinical documentation, growth tracking, immunization workflows, and medication handling.
- Role-based access, audit trails, and core reporting.
- Portal capabilities that reduce administrative loops.
- Integration endpoints and interface handling.
- Additional modules such as telemedicine, remote patient monitoring, and advanced analytics.
How to avoid fragile delivery:
- Use iterative releases with production-like test environments.
- Introduce integrations via standardized patterns rather than custom scripts.
- Implement clear schema versioning and API governance to prevent breaking changes.
This is also where you define “done.” In healthcare, “done” includes validation evidence, security checks, and workflow acceptance, not only feature completion.
Enterprise Note: Utilize CI/CD pipelines with automated unit testing for clinical calculations (e.g., if a code change breaks a dosing formula, the build fails).
Step 6: Validation & Regulatory Hardening
Testing in pediatric systems has one job: ensure you do not create hidden clinical risk.
For HIPAA-compliant pediatric EMR and EHR software, validation should cover:
- Authentication and authorization behavior across roles and proxy access.
- Audit log completeness, integrity, and searchability.
- Data accuracy across charting, immunizations, growth, and medication.
- Integration accuracy, including message mapping and reconciliation.
- Resilience testing: downtime behavior, backup restore, and incident workflows.
Clinical validation must include:
- Realistic pediatric scenarios, not generic demo scripts.
- Medication edge cases where weight or age dramatically changes dosing logic.
- Immunization schedule variations, catch-up logic, and exception handling.
- Documentation completeness checks tied to operational and billing processes.
This is the phase where compliance becomes real. Treat it as a gating milestone.
Enterprise Note: Go beyond HIPAA. Ensure compliance with ONC-Health IT certification standards to qualify for federal incentives.
Step 7: Deployment: The “Shadow Go-Live”
Deployment is not a switch flip; it is operational change management.
For pediatric environments, a controlled rollout typically looks like:
- A pilot group that represents real clinic variation.
- Parallel workflows for limited time windows where safety is validated.
- Training focused on workflows, not screens.
- Feedback loops that feed directly into short release cycles.
If you are replacing an existing system, deployment must also include:
- Data migration strategy and validation.
- Cutover planning with rollback conditions.
- A support model that handles peak questions without degrading clinic operations.
This is where adoption is earned. If deployment is chaotic, even a good product will be rejected by the organization.
Enterprise Note: Run the new system in parallel with legacy systems for a pilot group to ensure data parity.
Step 8: Post-Launch Governance
Go-live is the start of ownership. A sustainable operating model for pediatric healthcare software development includes:
- Scheduled releases with change control for templates and clinical content.
- Monitoring and incident response practices aligned with clinical operations.
- Continuous improvement based on usage signals, not anecdotal complaints.
- Regular security posture reviews and policy updates.
This is also where leadership sees value. When reporting, audit readiness, and operational flow improve over time, the system becomes a trusted infrastructure rather than a recurring project.
Enterprise Note: Establish a Clinical Advisory Board to review and approve updates to visit templates.
Key Features of Pediatric EMR and EHR Systems
When planning EHR software development for pediatrics, feature decisions should reflect how pediatric care is delivered in real clinical settings. The following capabilities form the operational core of effective custom pediatric EHR software.
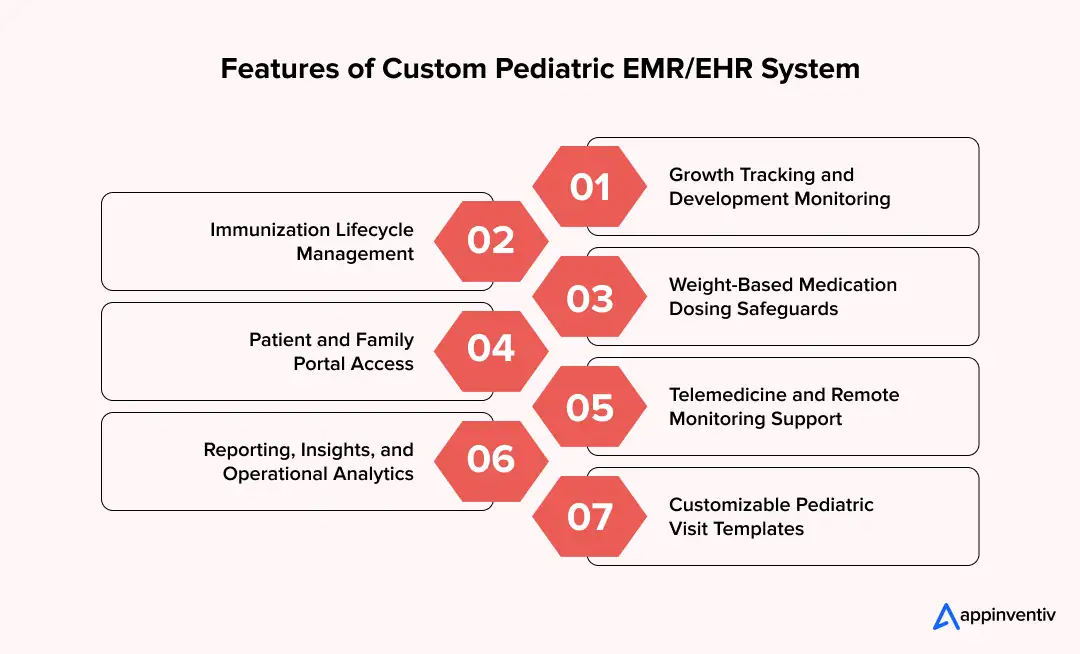
Growth Tracking and Development Monitoring
Growth assessment is a foundational element of pediatric care. A pediatric system must support longitudinal growth evaluation rather than isolated measurements.
Essential capabilities include:
- Age-appropriate growth charts that map weight, height, BMI, and head circumference against standardized percentile curves
- Longitudinal trend visualization to help clinicians detect deviations over time
- Developmental milestone tracking to support early identification of speech, motor, or cognitive delays
- Visual presentation of growth patterns that clinicians can interpret quickly and families can understand easily
When growth data is structured and clearly visualized, clinical interpretation is faster, and documentation remains consistent across visits.
Standard EMRs track height and weight; a pediatric system must interpret them through the lens of clinical informatics.
- Standards-Based Logic: Built-in support for CDC (2–20 years) and WHO (0–2 years) standardized percentile curves.
- The Enterprise Edge: Enable “Gestational Age Correction” for premature infants to prevent misdiagnosis of developmental or cognitive delays.
- Longitudinal Visualization: Trend mapping for BMI and head circumference to help clinicians detect deviations over time.
Immunization Lifecycle Management
Vaccination workflows drive a significant portion of pediatric visit scheduling, follow-ups, and compliance reporting. Immunization management must be embedded directly into the workflow.
The challenge in pediatric care is that State Immunization Information Systems (IIS) often use fragmented protocols.
- Bi-Directional Interoperability: Use an HL7 FHIR-based interface that does not just “push” data but also queries the registry to automatically reconcile “outside” vaccinations (from pharmacies or other clinics).
- Schedule Logic: Automated reminders for upcoming vaccines and catch-up schedules based on ACIP guidelines.
- Registry-Ready Documentation: Structured data capture that meets national public health reporting requirements without manual staff intervention.
A structured immunization workflow reduces administrative workload while supporting regulatory compliance and population health reporting.
Weight-Based Medication Dosing Safeguards
Medication dosing in pediatric care is a high-risk workflow where “generic” adult logic leads to errors.
- The Safety Matrix: Automatic dose calculation pulled directly from the most recent weight entry in the vitals module.
- Configurable Thresholds: Safety alerts that flag potential dosing errors (mg/kg) before the order is signed.
- Audit Transparency: Documentation of calculated doses and clinician overrides for forensic audit trails.
Embedding dosing safeguards within the workflow supports medication safety while maintaining clinical efficiency.
Also Read: Guide to Medication Management App Development
Patient and Family Portal (with Adolescent Privacy Governance)
Parents and guardians play a central role in pediatric care. A secure family portal improves transparency, reduces administrative inquiries, and strengthens follow-through on care plans.
A pediatric portal must manage complex proxy relationships that change as the patient matures.
- Proxy Access Governance: Secure access for multiple caregivers (parents, guardians, or foster care) with defined “decision rights.”
- Adolescent Privacy Filters: Implement Role-Based Access Control (RBAC) that triggers automatic privacy filters when a patient reaches specific age milestones (e.g., 12, 15, or 18) to protect sensitive behavioral or reproductive health data in accordance with local laws.
- Engagement Tools: Seamless appointment scheduling, prescription refills, and secure messaging to reduce administrative overhead.
A well-designed portal reduces front-desk workload and improves parent engagement without compromising privacy controls.
Also Read: Medical Scheduling Software Development Cost Estimation
Telemedicine and Remote Monitoring Support
Virtual care has become an expected component of pediatric services, especially for follow-ups, minor consultations, and chronic condition monitoring.
Core telemedicine capabilities include:
- Secure video consultations for routine visits and follow-up care
- HIPAA-compliant communication channels and documentation workflows
- Remote Vitals: Support for parent-reported data (temperature, symptoms, or glucose levels) within the patient profile.
- Integrated Documentation: Telehealth sessions that flow directly into the clinical record without fragmented data silos.
Telemedicine expands access while maintaining continuity of care.
Reporting, Insights, and Operational Analytics
Structured data enables better operational visibility and clinical insight. Pediatric practices benefit from reporting tools that support both care delivery and practice management.
Reporting capabilities should include:
- Population Health: Track immunization compliance rates across the entire patient base.
- Operational Performance: Dashboards for visit frequency, utilization patterns, and documentation completeness to identify care gaps early.
When data is structured and accessible, leadership can identify care gaps and operational inefficiencies early.
Customizable Pediatric Visit Templates
Pediatric visits vary widely by age group and clinical need. Flexible documentation templates support consistency while preserving clinician efficiency.
Template capabilities should include:
- Configurable templates for well-child visits, acute visits, chronic care, and developmental assessments
- Age-specific documentation workflows for infants, toddlers, school-age children, and adolescents
- Specialized forms for respiratory conditions, behavioral assessments, and developmental screenings
- Governance controls to manage template changes and maintain consistency
Template flexibility reduces documentation variability while supporting standardized care delivery.
Why These Features Matter in Practice
Including these capabilities in pediatric EMR and EHR system development ensures the system reflects real pediatric workflows rather than forcing clinicians to adapt their processes. Structured growth tracking, immunization lifecycle management, medication safety safeguards, and family engagement tools improve care coordination while reducing administrative friction.
When thoughtfully implemented, these features support clinical accuracy, operational efficiency, and a better experience for both providers and families.
Implementation Pattern: Registry Integration and Workflow Standardization
In multi-location pediatric environments transitioning from paper-based or fragmented digital systems, integrating immunization workflows with registry-compatible documentation and standardized visit templates often produces measurable operational improvements. Practices commonly experience smoother check-in workflows, fewer documentation corrections, and improved reporting readiness once workflows are standardized and registry integration is streamlined.
The key takeaway is not the metric itself but the operational alignment: when workflows, documentation standards, and integrations are designed together, administrative burden decreases, and clinical throughput improves.
Key Technologies and Considerations in EHR Integration for Pediatric Practices
Selecting the right architecture and integration strategy at the outset is critical to successful pediatric EMR and EHR system development. Technology choices affect interoperability, compliance, scalability, and long-term operational stability.
The benefits of custom pediatric EHR and EMR software are not limited to clinical function, but it also operates reliably within a broader healthcare ecosystem.
| The Pediatric Tech Stack | ||
|---|---|---|
| Component | Recommended Technology | Why it Matters |
| Backend | Node.js / Python (Django) | Handles complex growth/dosing logic. |
| Interoperability | HL7 FHIR / Redox | Seamless data flow to labs and state registries. |
| Database | PostgreSQL (Relational) | Essential for complex parent-child relationships. |
| Cloud | AWS HealthLake / Azure for Health | Built-in HIPAA compliance and analytics. |
Interoperability Across Healthcare Systems
Effective EHR integration for pediatric practices depends on standardized data exchange and clear ownership of clinical information.
Key considerations include:
- Support for integration of HL7 and SMART on FHIR standards to enable structured data exchange
- Integration with laboratories, pharmacies, immunization registries, and hospital networks
- Standardized data mapping to prevent duplication and reconciliation errors
- Consistent patient identity matching across systems
- Audit continuity when data flows between providers
Integration design should prioritize reliability and traceability rather than one-off interface builds.
Cloud vs. On-Premise Deployment Models
Infrastructure decisions influence governance, cost, and scalability.
Cloud deployment offers:
- Remote accessibility
- Rapid scalability
- Reduced upfront infrastructure investment
- Managed reliability and uptime
On-premise deployment provides:
- Direct infrastructure control
- Internal governance alignment
- Suitability for highly regulated environments
Hybrid models allow sensitive workloads to remain on-premise while leveraging cloud scalability for analytics, portals, and interoperability services.
The optimal model depends on compliance posture, integration landscape, and internal IT governance.
Data Security and Compliance Architecture
Security is foundational in pediatric EMR software development services due to the sensitivity of minors’ health data and family access pathways.
A robust security posture includes:
- Encryption of data in transit and at rest
- Role-based access control with least-privilege principles
- Multi-factor authentication for privileged access
- Comprehensive audit logs and access traceability
- Secure session management and timeout controls
- Backup, disaster recovery, and resilience planning
Compliance alignment should support HIPAA requirements and any regional regulatory obligations while maintaining operational usability.
Scalability and Performance Planning
Pediatric systems must scale without architectural redesign as practices expand.
Design considerations include:
- Support for multi-location deployment
- Performance stability during peak visit periods
- Modular expansion for telemedicine, reporting, or analytics modules
- Infrastructure capable of handling increasing data volume and concurrent users
Cloud-native or modular architectures are typically best suited for long-term growth.
Also Read: How to Develop a White-Label Telemedicine Platform?
Workflow-Centered UX Design
User experience in pediatric systems is a throughput decision, not merely a usability preference.
Effective UX should:
- Support rapid documentation during high-volume clinic sessions
- Reduce navigation complexity for common pediatric workflows
- Present safety prompts clearly without interrupting workflow
- Provide role-specific interfaces for clinicians, staff, and families
- Support mobile access for parent engagement
Well-designed workflows reduce training time and minimize adoption resistance.
AI and Automation Readiness
Artificial intelligence is not a prerequisite for launch, but systems should be designed to support future intelligence layers.
Practical applications include:
- Identifying upcoming immunization needs and follow-up gaps
- Operational forecasting for appointment demand
- Automated reminders and administrative workflow reduction
- Decision-support insights that highlight potential care gaps
AI deployment must remain explainable, governed, and carefully tuned to avoid alert fatigue or workflow disruption.
Also Read: The Impact of AI in Healthcare Industry
Implementation Pattern: Pediatric Analytics Supporting Preventive Care
Large pediatric systems increasingly use structured growth, immunization, and visit data to improve preventive care follow-through. When data is standardized and reporting workflows are consistent, care teams can identify gaps earlier and coordinate outreach more effectively.
The value comes from data structure and workflow alignment rather than analytics alone. Without standardized capture and governance, predictive insights cannot be trusted.
Getting these technology choices right ensures that custom pediatric EHR software remains secure, interoperable, and adaptable as care delivery evolves. Systems designed with integration standards, governance controls, and scalability in mind are far more resilient than those built around immediate functional needs alone.
Appinventiv delivers secure, scalable healthcare software tailored to your needs.
Challenges in Building Pediatric EMR and EHR Systems
Most pediatric EHR initiatives do not fail because of missing features. They struggle because workflow logic, governance, integration sequencing, and operational ownership are misaligned. In pediatric EMR software development, the risks are subtle but structural.
Below are the challenges that materially affect delivery outcomes.

1. Pediatric Workflow Variability Is Underestimated
Pediatric care is not a single workflow. It spans newborn care, immunization-only visits, developmental screenings, chronic disease management, adolescent confidentiality transitions, and parent communication cycles. Many initiatives treat pediatrics as “primary care with growth charts,” which creates hidden fragmentation.
Where programs struggle:
- Visit templates drift between providers.
- Growth tracking is captured inconsistently.
- Immunization documentation varies by location.
- Edge cases are handled outside the system.
What differentiates successful builds:
- Workflow modeling by visit category before design begins.
- Clinical informatics involvement in data modeling.
- Explicit documentation standards governed centrally.
- Clear ownership of template change control.
Without workflow discipline, custom pediatric EHR software becomes configurable chaos.
2. Immunization and Registry Logic Becomes Operationally Fragile
Immunization workflows are one of the most underestimated components of EHR integration for pediatric practices. Schedules evolve, catch-up logic varies, and registry interfaces have specific formatting and reconciliation rules.
Common failure patterns:
- Manual reconciliation when registry data conflicts with internal records.
- Incomplete documentation causes compliance exposure.
- Staff rely on external reference tools instead of the system.
How high-performing programs approach it:
- Immunization lifecycle logic embedded into the data model.
- Registry compatibility is defined early in the integration scope.
- Exception handling workflows for mismatches.
- Structured fields enforce clear documentation requirements.
Immunization reliability is not a feature. It is a compliance and workflow stability requirement.
3. Proxy Access and Adolescent Privacy Are Poorly Governed
Pediatric systems introduce access complexity that adult systems do not. Parents, guardians, and adolescents may require differentiated access levels over time. Without structured access governance, organizations risk privacy exposure.
Typical issues:
- Overexposure of sensitive adolescent information.
- Inconsistent proxy rules across providers.
- Manual workarounds for consent transitions.
What sets enterprise implementations apart:
- Role-based access models that account for age transitions.
- Explicit policy alignment between legal, clinical, and IT teams.
- Audit visibility into access changes and overrides.
- Controlled workflows for revoking or modifying proxy permissions.
This is where pediatric EHR data security becomes more nuanced than standard access control.
4. Integration Is Designed as a Technical Task Instead of a Governance Decision
Connecting labs and pharmacies is straightforward in theory. The complexity emerges in data ownership, reconciliation rules, and exception handling.
In pediatric EMR and EHR integration with hospital systems, challenges often include:
- Duplicate patient identity across systems.
- Inconsistent medication lists.
- Partial data synchronization.
- Unclear responsibility for correcting mismatches.
Organizations that succeed treat integration as:
- A governance discussion before a technical build.
- A master data ownership decision.
- A reconciliation workflow with defined escalation paths.
- A monitored process with audit traceability.
Integration is not simply about HL7 or FHIR; it is about accountability.
5. Alert Fatigue Undermines Safety Goals
Weight-based dosing alerts, immunization reminders, and compliance prompts are essential. However, when poorly tuned, they generate alert fatigue.
Observed risks:
- Clinicians override alerts reflexively.
- Important warnings become indistinguishable from noise.
- Productivity declines.
Mature pediatric electronic medical record software development includes:
- Tiered alerting logic.
- Clear differentiation between advisory and critical alerts.
- Override justification capture.
- Ongoing review of alert effectiveness.
Safety mechanisms must support workflow rather than disrupt it.
6. Change Management Is Treated as Training Instead of Cultural Transition
Resistance rarely stems from interface difficulty. It stems from disrupted routines and unclear expectations.
Common patterns:
- Shadow documentation outside the system.
- Inconsistent template usage.
- Partial adoption across locations.
Effective programs:
- Pilot with representative clinics.
- Tie training to real patient scenarios.
- Measure adoption metrics post-go-live.
- Enforce governance for template and workflow consistency.
In custom pediatric EHR software initiatives, cultural alignment matters as much as system design.
7. Long-Term Ownership Is Undefined
Post-launch sustainability is often overlooked. Systems degrade when ownership of updates, template control, integration monitoring, and compliance review is unclear.
Programs weaken when:
- No structured release cadence exists.
- Clinical changes are applied inconsistently.
- Audit logs are collected but not reviewed.
- Integrations break silently.
Enterprise-ready pediatric healthcare software development requires:
- Defined product ownership roles.
- Scheduled governance reviews.
- Integration monitoring dashboards.
- Controlled enhancement cycles.
The difference between a successful system and an unstable one often emerges after go-live.
8. Cost Escalation from Scope Creep and Integration Drift
Budget overruns rarely occur because features are expensive. They occur because the scope is undefined.
In pediatric programs, scope creep often appears through:
- Expanding integration targets mid-build.
- Adding complex analytics before workflow stabilization.
- Underestimating migration cleanup requirements.
- Retroactively fixing data model limitations.
Clear MVP boundaries, phased releases, and documented integration sequencing protect pediatric EHR development costs from uncontrolled expansion.
The Real Differentiator
The challenge is not building functionality, it is aligning:
- Pediatric clinical logic
- Data structure
- Access governance
- Integration accountability
- Operational ownership
When those layers are designed together, pediatric EMR and EHR system development becomes a stable infrastructure. When they are designed separately, the system becomes a recurring remediation project.
Cost Considerations for Custom Pediatric EMR and EHR System Development
There is no single price tag for pediatric EMR and EHR system development. The final investment depends less on how many features you list and more on how deeply the system must integrate with clinical workflows, external platforms, and compliance controls.
A focused build for a single pediatric clinic will sit at the lower end of the range. A multi-location system with registry integrations, structured governance, and reporting layers will move significantly higher. In most cases, projects fall between $30,000 and $400,000+, depending on complexity.
Factors That Affect the Cost
Several factors influence the pediatric EHR development cost.
Feature Set
A basic system with essentials like growth charts and immunization tracking costs less. Add more features, such as telemedicine, advanced analytics, and detailed reporting, and the price goes up.
System Integration
Connecting your EMR to labs, pharmacies, or health registries adds complexity. More connections mean higher costs.
Customization
Tailoring workflows and user roles to meet how your clinic operates takes extra development time. That costs more.
Security & Compliance
Meeting HIPAA, GDPR, and other regulations isn’t cheap. But cutting corners here isn’t an option.
Development Time and Team Expertise
Complex systems take longer to build. More hours from experienced developers mean a higher price tag.
Typical Investment Bands
A custom pediatric EMR/EHR investment depends on the depth of integration and the strength of compliance controls.
| Scope Level | Estimated Range |
|---|---|
| Core pediatric workflows, limited integrations | $30,000–$80,000+ |
| Portal, registry integration, structured reporting | $80,000–$150,000+ |
| Multi-site, advanced integrations, analytics layer | $150,000–$400,000+ |
Ongoing Costs
Plan for ongoing expenses such as hosting, integration maintenance, security updates, and regulatory adjustments. Many organizations allocate 15–20% of the initial build cost annually for maintenance and support.
ROI Perspective
The return from custom pediatric EHR software typically appears in:
- Reduced manual reconciliation
- Fewer documentation inconsistencies
- Lower audit remediation effort
- Improved workflow stability
The real financial benefit often comes from avoiding rework and compliance exposure rather than immediate revenue increases.
A disciplined scope definition and phased rollout protect both budget and long-term system reliability.
Appinventiv delivers secure, scalable healthcare software tailored to your needs.
How Appinventiv Can Help Build Your Custom Pediatric EMR and EHR Solution?
Delivering reliable pediatric EMR and EHR system development requires more than coding expertise. It demands a structured approach to clinical workflows, interoperability, and compliance.
Appinventiv brings over a decade of experience in healthcare software development services, having delivered projects for organizations such as Dr. Reddy’s, Health-e-People, Soniphi, DiabeticU, and YouComm. Our work spans patient engagement platforms, interoperable healthcare systems, and secure clinical applications.
Focused Pediatric Execution
We design custom pediatric EHR software aligned with real clinical workflows, including growth tracking, immunization management, medication safeguards, and structured documentation standards.
Compliance and Security Built-In
Our pediatric electronic medical record software development follows a security-first model, with role-based access controls, encryption, and audit-ready logging to support HIPAA-aligned environments.
Integration-Ready Architecture
We structure EHR integration for pediatric practices to ensure compatibility with labs, registries, pharmacies, and hospital systems, reducing long-term integration risk.
If you are evaluating custom EMR and EHR solutions for pediatric clinics, we focus on building systems that remain stable, secure, and scalable as your organization grows.
Let’s discuss your pediatric EMR roadmap.
FAQs
Q. What are the key functionalities of pediatric EMR software?
A. Pediatric EMR software should have features that are built specially for kids. Including:
- Growth charts, immunization tracking, and dosing calculators based on age and weight.
- Should be able to easily pull up patient history and manage vaccination schedules.
- Secure parent portal that lets families check records and communicate with your office.
- Should handle scheduling and billing
- Templates for different visit types, like well-child checkups or sick visits.
Q. How do you ensure HIPAA compliance in pediatric EHR systems?
A. HIPAA compliance starts with strong data security. The pediatric EHR systems should:
- Use encryption, maintain audit trails, and require secure authentication for all users.
- Set up role-based access so staff only see what they need to.
- Run regular security audits and maintain robust data backup protocols.
These steps protect patient privacy and keep you compliant with HIPAA requirements.
Q. Why is weight-based dosing critical in pediatric EMRs?
A. Unlike adults, pediatric medication is calculated per kilogram. A custom EMR automates this by pulling weight directly into the e-Prescription module, eliminating manual calculation errors that account for nearly 37% of pediatric medication mistakes.
Q. How does a custom EMR handle adolescent privacy?
A. High-end systems utilize “Sensitive Data Filters.” These allow parents to see immunization records while automatically restricting access to confidential visits (e.g., behavioral health) once the child reaches the legal age of consent in their state.
A. How can AI and analytics improve pediatric EHR functionality?
A. AI can spot patterns you might miss otherwise. It can flag potential health risks and handle routine tasks, freeing up your staff.
Analytics tools show you trends in your practice. This helps you make better decisions about patient care.
Q. What technology stack is best for pediatric EHR software development?
A. For the back-end, frameworks like .NET, Node.js, or Python work well. React or Angular are solid choices for the front-end.
Follow FHIR/HL7 standards. Cloud solutions like AWS or Azure give you scalability and security. React Native works great for building mobile-friendly parent portals.
Q. How much does it cost to develop a pediatric EMR and EHR system?
A. Expect to spend anywhere from $30,000 to $400,000, depending on what you need. It will cost less with basic features and increase as per the complexity. Additionally, you need to pay for ongoing maintenance.
Q. How long does it take to develop and deploy a pediatric EMR system?
A. Most projects take 6 to 12 months from start to finish. The timeline depends on how complex your system is and how many features you want.
A simpler system moves faster. Highly customized solutions with AI or telemedicine take longer.


- In just 2 mins you will get a response
- Your idea is 100% protected by our Non Disclosure Agreement.

Healthcare Kiosk Software Development – Benefits, Use Cases, Features, Costs, Process
Key takeaways: The healthcare kiosks streamline administrative processes, enhance patient flow, improve staff productivity, reduce costs, and enhance the patient experience. Healthcare kiosks enhance efficiency and personalized care through EMR/EHR-integrated kiosk software with AI, delivering real-time data updates. Scalable kiosk solutions lower operations expenses, enhance patient throughput and improve service delivery in healthcare organizations. Patient…

How To Develop a Sustainable Healthcare System?
Key Takeaways Rising costs and climate pressure make building a sustainable healthcare system a core business and risk strategy decision. Learn the key principles of sustainable healthcare system development, including prevention, efficiency, equity, and social sustainability. See how AI, data platforms, and a sustainable digital system in healthcare cut waste, improve outcomes, and stabilize workforce…

EHR Implementation for Healthcare Providers: Process, Features, and Total Cost Analysis
Key takeaways: A clear EHR implementation guide keeps teams on track and prevents delays. The full EHR implementation process includes planning, setup, moving data, training staff, and regular updates. The right features handle clinical work, billing, reports, and compliance for large healthcare organizations. EHR implementation costs vary based on design, integrations, data migration, training hours,…