- EHR Implementation Framework for Enterprise Healthcare Providers
- Essential Features and Non-Functional Requirements for a Successful EHR Implementation
- How Much Does EHR Implementation Cost? Total Analysis
- EHR Implementation ROI: TCO Model and Break-Even Analysis
- Common EHR Implementation Challenges and How to Solve Them
- How to Drive EHR Adoption and Measure Success
- Evaluating the Right EHR Partner: Vendor Criteria and RFP Checklist
- Why Appinventiv Is the Right EHR Implementation Partner
- Frequently Asked Questions
Key takeaways:
- A clear EHR implementation guide keeps teams on track and prevents delays.
- The full EHR implementation process includes planning, setup, moving data, training staff, and regular updates.
- The right features handle clinical work, billing, reports, and compliance for large healthcare organizations.
- EHR implementation costs vary based on design, integrations, data migration, training hours, and maintenance.
- A clear roadmap with assigned roles and deadlines helps organizations manage change with fewer problems and stronger outcomes.
Healthcare providers must run systems that support safe care, rapid decision-making, and smooth daily operations. Many still rely on outdated tools that slow teams down and create gaps in patient data. This is why more hospitals and large provider groups are now planning structured EHR implementations to support long-term growth.
In fact, research shows that EHR implementation can reduce data-entry errors by 20–30% and improve documentation accuracy by 15–25%, helping healthcare teams maintain more reliable patient records.
However, a successful rollout is not just installing new software. It needs a clear plan, strong teamwork, and a realistic view of cost. Leaders want to know how the EHR system will support patient care, reduce clinical workload, and comply with regulatory requirements. They also need to see how the system fits into their healthcare digital transformation roadmap.
This guide explains the EHR implementation process in a simple and practical way. It covers key stages, feature needed, common barriers, and a clear cost analysis. The goal is to help leaders plan a stable transition and support their teams with a system that meets clinical and business needs.
Appinventiv’s structured EHR implementation roadmap is designed to avoid these failures and delays.
EHR Implementation Framework for Enterprise Healthcare Providers
A successful EHR rollout follows a clear and repeatable structure. Large healthcare organizations depend on this structure to reduce risk, avoid delays, and maintain safe clinical operations. The framework below reflects the steps most high-performing provider groups follow when implementing an EHR system at scale.
1. Governance and Discovery
Every strong EHR implementation for healthcare providers starts with a solid governance model. Leaders form a steering committee that includes clinical, operational, IT, and compliance heads. This group drives decisions, sets priorities, and removes roadblocks.
During this first stage, teams define their goals. These include clinical, reporting, billing, and healthcare compliance expectations. They also review current workflows to understand what is working and what needs improvement.
This stage sets the tone for the entire rollout. Clear direction early on helps control cost, timelines, and system expectations across the organization.
2. Requirements Gathering and Vendor Selection
This step builds the base for the final EHR implementation plan. Teams prepare a structured RFP or RFI. They document what the system must do, how it should support each department, and the required integrations.
Leaders also review vendors through a scoring model. This includes product strength, usability, and ONC-Health IT Certification (under the 21st Century Cures Act). For enterprise security, verify SOC 2 Type II reports to ensure operational controls are validated over time, not just a point-in-time audit.
A strong IT outsourcing selection for healthcare reduces the risk of gaps later in the rollout.
3. System Design and Workflow Configuration
Once a vendor is selected, the next step is to design the system. Teams map clinical and administrative workflows. They create custom EHR implementation plan templates, order sets, and user roles. They also set rules for documentation, patient flow, and specialty needs.
This phase requires close support from clinical staff. The goal is to make sure the system matches real-world practice, not the other way around.
A well-designed system reduces the burden on clinicians and supports higher adoption during Go-Live.
4. Data Migration Strategy
Data migration is one of the most sensitive parts of implementing EHR in healthcare. Teams start with data mapping. They define what needs to be moved, how clean the data is, and how it should appear in the new system.
Multiple rounds of cleansing, testing, and validation follow. This prevents errors, missing data, or mismatched records.
Smooth data migration protects patient safety and supports continuity of care when the new system goes live.
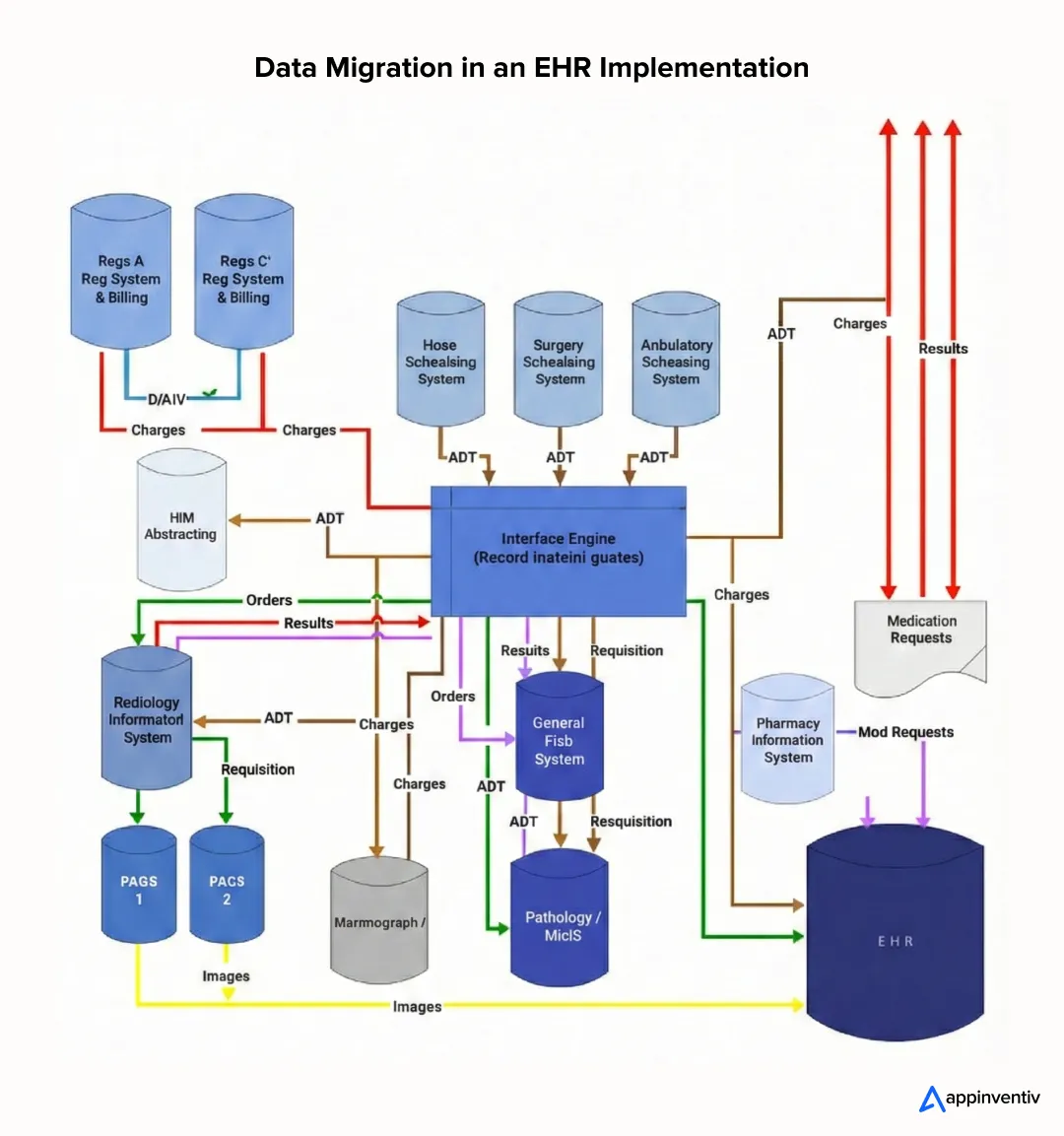
5. Interoperability and Integrations
Healthcare today runs on connected systems. This stage links the EHR with labs, imaging tools, billing software, HIEs, and other clinical platforms.
Most enterprise teams use integration standards like HL7 and SMART on FHIR. The goal is fast, two-way data exchange with no manual entry. Good interoperability helps clinicians make better decisions and cuts down on admin tasks.
This stage affects both the budget and schedule. Plan it early.
6. Training, Pilot, and Change Management
Training is one of the most important stages of the entire EHR implementation process. Teams follow a clear plan that includes super-user programs, department-level training, and simulation sessions. This helps staff feel confident before Go-Live.
Change management in EHR implementation matters just as much as the technology. Leaders need to prepare teams for new workflows, new tools, and new routines. Clear communication lowers stress and helps clinicians adjust without major problems.
A pilot program lets the organization test the system in a limited setting before going live across all locations.
7. Go-Live and Post-Go-Live Optimization
The Go-Live stage needs tight coordination. Teams often run both the old and new systems at the same time for a brief period to lower risk. Support teams remain on-site to address issues fast.
After Go-Live, the work shifts to EHR optimization for better efficiency and performance. Teams watch how the system runs, collect user feedback, and refine workflows. Reporting tools, security settings, and integration points get reviewed on a regular schedule.
This continuous process keeps the EHR aligned with patient care, business goals, and compliance requirements. Organizations should also define EHR downtime procedures before Go-live so clinicians can continue care during temporary system outages.
Also Read: EHR Software Development: A Complete Guide
Essential Features and Non-Functional Requirements for a Successful EHR Implementation
A strong EHR system must handle clinical work, business operations, compliance, and future growth. Healthcare providers often focus only on basic clinical features when planning an EHR implementation.
Large organizations need more than that. They require healthcare interoperability, security, reporting tools, and workflow support. The points below cover the features and technical requirements that make up a solid EHR implementation plan.
1. Clinical Modules
Healthcare teams need clear and fast documentation. A good EHR system should allow simple note-taking, structured templates, and quick updates during patient visits. Order entry, e-prescribing, and result tracking must work without friction. This cuts down on errors and delays in care.
These clinical features must automate high-stakes administrative tasks, such as ICD-10-CM/PCS and CPT/HCPCS coding. Advanced systems use NLP-driven computer-assisted coding (CAC) to match clinical documentation with the correct medical codes, reducing claim denials.
These are the core of any EMR or EHR implementation in healthcare. They support safer care, more accurate records, and faster decisions across all departments.
2. Administrative and Revenue Cycle Functions
Clinical work is only one part of the full care journey. Hospitals and multi-site healthcare groups also need strong administrative and billing tools.
A complete system should include:
- Scheduling for single or multi-site operations
- Patient registration and insurance checks
- Coding and documentation support
- Claims management
- Billing and payment tracking
These features help reduce manual steps and improve the organization’s financial health.
3. Interoperability Capabilities
Healthcare today runs on smooth data sharing. During EHR implementation for healthcare providers, leaders must confirm that the system can connect with labs, imaging tools, pharmacy systems, and third-party platforms.
Modern interoperability relies on HL7 FHIR (Fast Healthcare Interoperability Resources). For secure third-party app integration, prioritize SMART on FHIR protocols, which use OAuth2 for identity management. This ensures your EHR can securely connect to specialized ‘bolt-on’ applications without compromising the core database.
A system with strong API support reduces barriers and helps teams avoid common integration issues later.
4. Security, Compliance, and Reliability
Security is a core concern when implementing an EHR system in any healthcare environment. Patient data security is essential and it should meet the healthcare compliance requirements of national and regional standards. HIPAA and EHR implementation often go hand in hand, as both focus on protecting patient information.
Important controls include:
- Role-based access
- Encryption using AES-256 (at rest) and TLS 1.3 (in transit)
- Detailed audit logs
- HITRUST-aligned data backups and disaster recovery (DR) protocols
- Regular SOC2 Type II attestation and HIPAA Security Rule audits
- Testing for reliability and uptime
Regulatory compliance in EHR implementation is required. It protects the organization, keeps trust intact, and makes audits easier.
Also Read: Cost to Build a HIPAA-Compliant Platform
5. Population Health, Analytics, and Reporting
At the enterprise level, data informs decisions. Leaders need dashboards and reports that show trends, performance gaps, and patient outcomes. A strong analytics module serves clinical teams, finance departments, and operations.
This includes:
- Quality measure reporting
- Clinical outcome tracking
- Departmental performance insights
- Operational and financial dashboards
- Support for external reporting needs
These insights help leaders plan improvements and track the benefits of a successful EHR implementation.
6. Usability and Adoption Features
Even the strongest system fails without user adoption. This is why usability should be a core part of every EHR implementation guide and roadmap.
Key usability needs include:
- A clean, easy-to-navigate interface
- Mobile access for on-the-go teams
- Shortcuts and custom workflows
- In-app help and training content
- Tools that reduce clicks and manual work
- Seamless telehealth access that saves visit notes, consent, and billing details to the chart.
These elements help users adapt quickly and reduce challenges during Go-Live. They also support the larger goal of improving clinical work and strengthening adoption across teams.
These features and technical requirements build the foundation of a stable EHR system. They help healthcare providers run efficient operations, lower risks, and stay compliant across all departments.
How Much Does EHR Implementation Cost? Total Analysis
Planning the cost of EHR implementation in healthcare is often a major concern for healthcare leaders. The price varies widely because each organization has different needs, workflows, and system expectations. A clear view of cost drivers helps CEOs, CTOs, CMIOs, and other decision-makers prepare an accurate budget and avoid unexpected delays.
EHR implementation involves more than software purchase. It includes design, data migration, change management, ongoing support, and long-term system upgrades. Below is a breakdown of the major cost areas that shape the total effort of implementing an EHR system.
1. Main Cost Drivers in an EHR Implementation
These cost drivers apply to most healthcare providers, whether they are planning their first EMR–EHR implementation or modernizing an older system.
Software Licenses or Subscriptions
This includes the core EHR platform and any specialty modules. Costs can be per user, per provider, or per facility. Cloud systems usually run on subscription models.
Implementation Services
These costs include system setup, workflow design, customization, and project management. A large part of the EHR implementation process depends on the quality of these services.
Hardware and Infrastructure
Hospitals may need new computers, scanners, tablets, printers, servers, or network upgrades. Cloud systems may reduce hardware needs, but they still require strong connectivity.
Data Migration
This covers data mapping, cleansing, migration tools, testing, and validation. Good data quality prevents major issues during Go-Live.
Integrations
Many organizations connect their EHR to labs, imaging systems, HIEs, billing tools, and external partners. High levels of integration often increase both time and cost.
Plan a separate line for telehealth integration costs. These cover secure video platforms, API work, RPM device feeds, and tele-billing setup.
Training and Change Management
Training is one of the most important stages of EHR implementation. Hands-on sessions, super-user programs, and department training add to the overall cost. Change management in EHR implementation also requires communication support and leadership involvement.
Ongoing Support and Maintenance
Support includes customer service, system updates, security patches, and new feature releases.
Indirect or Hidden Costs
These may include lost productivity during Go-Live, overtime pay, or temporary staffing support.
2. Sample Cost Breakdown by Organization Size
The table below shows typical ranges for the cost of EHR implementation. These numbers are general industry ranges. Actual costs depend on the level of customization, number of integrations, and system complexity.

These ranges reflect common EHR implementation strategies and patterns found in many projects. Enterprises with advanced reporting, high-volume clinical work, and strict compliance needs often fall on the higher side of the range.
3. Practical Budgeting Guidelines for Healthcare Leaders
Planning early saves time and avoids unnecessary rework. Below are simple budgeting rules that help large healthcare providers set a stable financial base for the project.
Allocate 15–25% of the Budget for Training and Change Management
Many teams under-plan this part of the rollout. Strong training reduces implementation challenges and improves user comfort.
Set Aside 10–20% of the Budget for Integrations
Integrations can introduce unexpected delays. Early planning prevents cost spikes later in the project.
Keep a 10–25% Contingency Fund
Large EHR implementation approaches often reveal hidden needs once the system design begins. A contingency buffer protects the project timeline.
Plan a 5-Year Total Cost of Ownership (TCO)
This helps leaders compare vendors, calculate long-term costs, and build a realistic roadmap. A complete TCO includes licenses, maintenance, upgrades, and support.
Review Compliance and Security Costs Separately
Regulatory compliance in EHR implementation often requires extra tools, audits, or upgrades. This cost should be tracked as a separate line item.
4. What Drives Costs Higher?
Healthcare organizations may see higher costs if:
- They run multi-site networks with different workflows
- They require custom modules or deep reporting
- They depend on many third-party integrations
- They need high-volume data migration
- They face strict compliance or security needs
- They roll out the system in stages rather than all at one time
A clear EHR implementation roadmap reduces these surprises and keeps the project within budget.
5. Why Accurate Cost Planning Matters
A detailed cost plan protects the organization from delays, workflow disruptions, and compliance risks. It helps leaders see the bigger picture of the effort, time, and resources needed to implement EHR in healthcare. It also makes it easier to compare vendors and choose a system that meets long-term clinical and business goals.
Our healthcare technology experts help organizations plan scalable EHR implementations with predictable cost and ROI outcomes.
EHR Implementation ROI: TCO Model and Break-Even Analysis
Below is a sample structure showing how a healthcare provider (hospital or large clinic) might estimate the total cost of EHR implementation and project potential return on investment over time.
| Cost / Benefit Component | Typical Range / Estimate | Notes / Assumptions |
|---|---|---|
| Upfront Software / Licensing | $300,000 – $1,000,000+ (for medium-to-large facilities) | Varies by whether using off-the-shelf or custom EHR; number of users; modules required. |
| Initial Setup & Configuration | $10,000 – $50,000+ | Includes installation, workflow adaptation, regulatory compliance setup. |
| Integration & Data Migration | $5,000 – $100,000+ | Depends on number of legacy systems, complexity of integrations (labs, billing, imaging, etc.). |
| Training & Onboarding | $1,000 – $20,000+ | Based on number of users (clinicians, admin staff) and depth of training required. |
| Testing, QA & Go-Live Support | $10,000 – $50,000+ | Includes performance testing, bug fixes, compliance audits. |
| Annual Maintenance & Support | $10,000 – $100,000+/year | Covers software updates, user support, compliance upkeep, infrastructure costs for on-premise. |
| Compliance & Security Overheads | $5,000 – $50,000+ (initial/recurring) | Related to regulatory compliance (e.g. data protection, audits) depending on region requirements. |
| Ongoing Operational Costs (staff/time) | Varies based on staffing changes; may include an initial productivity dip | Some decrease in clinical productivity often occurs during first 1–2 years. |
Expected Returns & Savings (over time)
Some studies show that EHR implementation can lead to a 5–10% reduction in operational costs through workflow efficiency and process automation.
A long-term study at a tertiary hospital reported a positive net present value, with savings and efficiency gains outweighing costs over about 6 years.
In a broader hospital-level sample, facilities with advanced EHRs had ~9.7% lower per-patient admission costs than those without advanced EHRs, indicating improved cost efficiency in care delivery.
What This Means for Decision-Makers
Upfront investment is substantial, but spread over 5–8 years (or more), long-term operational savings and better care delivery can offset the cost.
The break-even point varies: hospitals that manage workflows and user training well tend to see ROI in 3–6 years, according to published cost-benefit studies.
Health systems that adopt EHRs tend to benefit through lowered per-patient costs, fewer errors, improved care coordination, better billing accuracy, and reduced administrative burden.
Common EHR Implementation Challenges and How to Solve Them
Even with a solid plan, healthcare providers may face issues during an EHR implementation. These issues often occur in groups, particularly with many sites, complex workflows, or older systems. When leaders understand these risks early, they can set the right controls and avoid delays.
Below are the most common barriers and the steps leaders can take to manage them.
1. Data Quality Issues
Poor data quality is a major risk in any EHR implementation process. Older records may be incomplete, repeated, or saved in different formats. If this data moves into the new system without cleaning, it can create errors and affect patient care.
How to reduce this risk:
- Run a detailed data audit before migration
- Remove duplicates and fix incomplete entries
- Test data in smaller batches
- Validate records before final Go-Live
A strong data plan reduces the chance of errors in patient files.
2. Workflow Mismatch
Every department works differently. If the new EHR system does not match real workflows, teams may find it slow or confusing. This can reduce adoption and create frustration.
How to reduce this risk:
- Map current workflows in detail
- Involve clinical staff during system design
- Run small pilots before a full rollout
- Adjust templates and rules based on real feedback
This step supports the importance of a successful EHR implementation across all units.
3. Integration Problems
Many provider groups depend on several systems for labs, imaging, billing, and pharmacy. If these systems do not connect smoothly, teams face delays and manual work.
How to reduce this risk:
- Identify all systems early in the EHR implementation plan
- Review technical standards such as HL7 and SMART on FHIR
- Test integrations with real-case scenarios
- Monitor connection performance after Go-Live
Review technical standards and participation in nationwide frameworks like TEFCA (Trusted Exchange Framework and Common Agreement) or Carequality. This ensures your integration strategy supports data sharing beyond local labs and reaches the broader Health Information Network (HIN). Good integration planning prevents major gaps later.
4. User Resistance and Low Adoption
Teams may resist change due to fear of new tools or concern about increased workload. This slows down the EHR rollout and affects the value the system can offer.
How to reduce this risk:
- Use clear communication from leadership
- Start change management in EHR implementation early
- Build a super-user group that supports training
- Offer hands-on practice before Go-Live
A strong change plan reduces stress and supports faster adoption.
5. Compliance and Security Risks
New systems must follow strict rules for patient data protection. Security gaps during EHR rollout can lead to compliance failures and operational risk.
How to reduce this risk:
- Review HIPAA and EHR implementation controls
- Set role-based access and audit logs
- Test backup and recovery plans
- Run security checks before and after Go-Live
This ensures the new system meets regulatory needs from day one.
6. Budget Overruns and Timeline Delays
Large EHR projects often involve many teams and steps. Without strong oversight, tasks can drift, and costs may rise.
How to reduce this risk:
- Build a clear EHR implementation roadmap
- Define milestones and responsibilities
- Review budgets at every stage
- Keep a contingency fund for unexpected needs
This approach protects the project and keeps it on track.
7. Performance Issues During Go-Live
Systems may slow down if the load exceeds expectations. This can disrupt clinical work and frustrate staff.
How to reduce this risk:
- Test system performance before Go-Live
- Prepare backup workflows for critical areas
- Add extra support during the early days
- Monitor the system closely and fix issues fast
Stable performance supports safer patient care.
Sample Risk Register (Simple Format)
Healthcare leaders can use the template below to track risks before and during rollout.
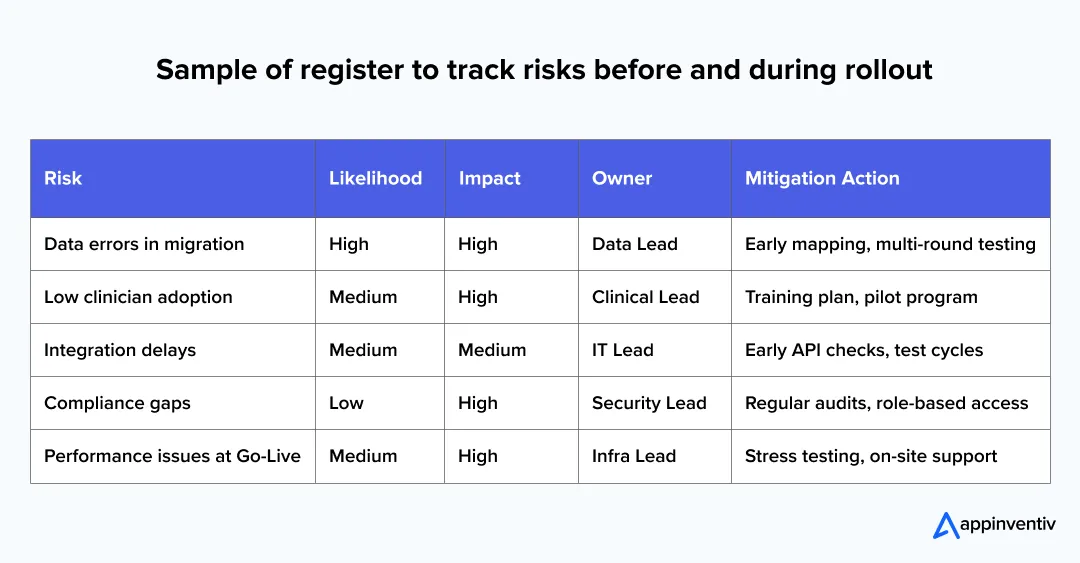
A register like this creates visibility and helps teams solve issues before they grow.
Having challenges during EHR implementation is common, but good planning helps control them. When leaders understand these risks early, they can build a stronger system that supports both clinical needs and business goals.
How to Drive EHR Adoption and Measure Success
An EHR rollout is only successful when the system fits well into daily clinical work. This depends on how easily users learn the system and how fast they adjust to new steps. A clear adoption plan helps leaders manage early issues and track the real benefits of EHR implementation over time.
Below are the steps and indicators that support strong adoption across large healthcare networks.
1. Build a Structured Training Plan
Training should follow a simple, clear sequence that supports different user groups. It should not overwhelm clinicians or staff.
A good plan includes:
- Super-user training for department champions
- Hands-on sessions for clinicians and nurses
- Telehealth simulations in training. Test video visits, consent capture, charting, and billing in the pilot.
- Step-by-step guides for billing and administrative staff
- A clear EHR implementation plan template for training timelines
- Access to in-app help and quick tips
Strong training reduces the common barriers and improves user comfort before Go-Live.
2. Prepare a Go-Live Readiness Checklist
Large healthcare providers need a clear readiness checklist before turning on the system. Provide an AI-based EHR readiness checklist for streamlined healthcare operations. This reduces last-minute delays and keeps the transition stable.
A readiness checklist covers:
- Completed user training
- Tested workflows
- Validated data migration
- Confirmed integrations (lab, imaging, billing, HIE)
- Support teams are assigned for immediate issue handling
This approach keeps operations smooth during the early days of Go-Live.
3. Use a 30–60–90 Day Adoption Roadmap
This simple timeline helps teams follow a step-by-step path after Go-Live.
First 30 Days
- Resolve early issues
- Gather user feedback
- Monitor productivity dips
60 Days
- Adjust workflows based on feedback
- Review reporting needs
- Improve templates and shortcuts
90 Days
- Stabilize operations
- Track early results of the EHR implementation benefits
- Prepare long-term optimization steps
This roadmap guides teams through the expected learning period.
4. Track Key Metrics (KPIs) to Measure Success
Healthcare leaders should track measurable indicators to see if the EHR system is performing well.
Common KPIs include:
- Time to complete clinical documentation
- Patient throughput per provider
- User satisfaction and feedback scores
- Medication order turnaround time
- Patient safety alerts and documentation errors
- System uptime and response speed
- Claim denial rates
Also Read: How to Implement Denial Management Automation in Healthcare
These KPIs show whether the system supports clinical care, business operations, and compliance goals.
5. Communicate Early Wins
Small wins build confidence across teams. They help reduce the challenges of EHR implementation and remind clinicians that the effort leads to better workflows.
Examples of early wins:
- Faster access to patient histories
- Fewer duplicate tests
- Reduced time spent searching for orders or reports
- More accurate billing codes
Highlighting these improvements helps strengthen overall adoption.
Adoption is the stage where the EHR system becomes part of daily work. With clear training, steady communication, and simple KPIs, leaders can guide teams through the early transition. This helps the system settle in and creates a strong base for future improvements and better patient care.
Evaluating the Right EHR Partner: Vendor Criteria and RFP Checklist
Choosing the right vendor is the most crucial step for any EHR implementation process. They can reduce risks, support smooth adoption, and help your teams follow a clear EHR implementation roadmap. A poor vendor match, on the other hand, can increase delays, raise costs, and add new challenges to an already complex project.
Let’s see the vendor selection criteria healthcare providers should review before making a final decision. It also includes a simple RFP checklist that business and technology leaders can use during evaluation.
1. Technical and Functional Evaluation
Healthcare leaders should start by evaluating if the system supports all required clinical and administrative functions. This includes core clinical workflows, reporting, billing, and specialty needs.
Key points to assess:
- Ease of clinical documentation
- CPOE and e-prescribing features
- Scheduling and billing tools
- Quality reporting and analytics
- Interoperability with labs, imaging, and HIEs
- Support for HL7 and FHIR
- Flexibility to adjust workflows as needs change
These factors help ensure the system fits daily operations without forcing teams to change their entire work style.
2. Compliance and Security Standards
Regulatory compliance in EHR implementation is not optional. Healthcare organizations must confirm the vendor follows strict standards for protecting patient data.
Important checks include:
- HIPAA-compliant controls
- Role-based access
- Encryption in transit and at rest
- Audit logs and activity tracking
- Backup and recovery plans
- Clear uptime commitments
Security gaps raise risks during Go-Live and increase the long-term cost of EHR implementation. A compliant vendor reduces these concerns from day one.
3. Integration and Interoperability Readiness
Hospitals and provider groups depend on smooth data flow between systems. The vendor must support a wide range of integrations and be able to manage complex data exchange patterns.
Review the vendor’s ability to connect with:
- Lab systems
- Imaging platforms
- Pharmacy systems
- Billing and claims tools
- External clinical systems
- HIE networks
Strong interoperability reduces barriers to EHR implementation and supports clinical decision-making.
4. Implementation Experience and Support Model
The strength of the vendor’s implementation team matters as much as the software itself. Healthcare providers should review the vendor’s past EHR implementation steps, support quality, and the documentation process.
Look for:
- Experience with similar-sized organizations
- Clear onboarding and training plans
- A defined change management process
- Dedicated project managers
- On-site and remote support options
- Structured Go-Live and Post-Go-Live support
A good partner will guide teams through each stage of the rollout and help reduce the implementation challenges.
5. Total Cost of Ownership (TCO) Transparency
Vendors should clearly explain:
- Licensing models
- Implementation fees
- Integration costs
- Training and ongoing support
- Upgrade costs
- Long-term operating expenses
Transparent pricing helps leaders compare systems, plan budgets, and avoid unexpected spending later.
6. RFP Checklist for Healthcare Providers
Below is a simple list of questions and checks that CIOs, CTOs, CMIOs, and procurement teams can add to their RFP process.
RFP Questions to Ask Vendors
- What clinical and administrative features come in the base system?
- How does your EHR support data sharing and system integrations?
- Can you show an EHR implementation plan from clients like us?
- What security and compliance controls does your system include?
- How do you manage data migration and testing during rollout?
- What is your timeline for implementing an EHR system of our size?
- How does your system support telehealth integration with EHR, remote monitoring, and tele-billing workflows?
- How do you support training and change management during Go-Live?
- What SLAs do you provide for uptime, response time, and issue handling?
- What are the estimated five-year costs, including updates and support?
- How do you help improve the system after the initial rollout?
7. Weighted Scoring Model (Optional but Helpful)
Organizations can score each vendor using a simple model that assigns weight to areas such as:
- Functionality
- Security and compliance
- Interoperability
- Implementation strength
- Cost
- Training and support
- Long-term roadmap
This helps remove guesswork and create a data-driven vendor comparison.
Choosing the right EHR partner is key to a smooth rollout and strong system performance. A clear evaluation process helps leaders compare vendors with confidence and avoid costly problems later.
If you are ready to assess your current systems or plan the next stage, our team can guide you.
Why Appinventiv Is the Right EHR Implementation Partner
Healthcare providers need more than a development team when planning an EHR implementation. They need a partner that understands clinical workflows, complex integrations, data security, and the realities of running multi-site operations.
Appinventiv offers healthcare software development services that support these needs with technical depth, hands-on experience, and a proven record across large enterprise programs.
What sets us apart
- Strong technical expertise in healthcare systems
- Experience with complex system modernization
- Compliance-first development approach
- Cross-functional delivery teams
- Support for long-term improvements
The focus of our EHR integration services stays on stable operations, smooth adoption, and measurable value across departments.
By partnering with Appinventiv, healthcare providers gain a stable path to integrating EHRs, with a team that understands technology, clinical operations, and long-term system performance.
If you are planning an EHR rollout or evaluating system upgrades, our team can help you assess the right approach.
Frequently Asked Questions
Q. How long does it take to implement an EHR system?
A. The time depends on your organization’s size, the number of systems you need to connect, and how much data must be moved.
- Most healthcare providers complete the main stages of the EHR implementation process in 6 to 18 months.
- Large networks may need more time because they require deeper testing, wider training, and stricter compliance checks.
Q. How to build an EHR system?
A. You start by defining what your clinical and administrative teams need from the system. Then you design the structure, map key workflows, and set the rules for data and compliance. After this, development teams build modules for notes, orders, billing, reports, and system connections. A complete plan also includes testing, user training, data migration, and regular updates after the system goes live.
Q. What are the four steps to a successful EHR implementation?
A. While every organization has its own approach, four common steps include:
- Planning and governance
- System design and configuration
- Data migration and workflow testing
- Training, Go-Live, and Post-Go-Live optimization
These steps help healthcare providers manage changes smoothly and reduce the EHR implementation challenges.
Q. How to measure the success of EHR implementation?
A. Success is measured through clear KPIs. These include documentation time, clinical throughput, claim accuracy, user satisfaction, system uptime, and data quality. Leaders can also track improvements in patient safety, reporting speed, and billing performance. A strong EHR implementation roadmap makes these results easier to measure.
Q. How do I choose the right EHR system for my healthcare institution?
A. To choose the right EHR for your healthcare institution, follow the process below:
- Start by listing the clinical and administrative needs of your organization.
- Check if the EHR system can support your reporting needs and connect with the tools you already use.
- Make sure it offers strong security, simple workflows, and reliable data exchange.
- Review each vendor’s cost, support model, and long-term product plan.
This helps to work with a partner with hands-on experience in EMR–EHR implementation and who understands the needs of large healthcare teams.


- In just 2 mins you will get a response
- Your idea is 100% protected by our Non Disclosure Agreement.

Healthcare Kiosk Software Development – Benefits, Use Cases, Features, Costs, Process
Key takeaways: The healthcare kiosks streamline administrative processes, enhance patient flow, improve staff productivity, reduce costs, and enhance the patient experience. Healthcare kiosks enhance efficiency and personalized care through EMR/EHR-integrated kiosk software with AI, delivering real-time data updates. Scalable kiosk solutions lower operations expenses, enhance patient throughput and improve service delivery in healthcare organizations. Patient…

How To Develop a Sustainable Healthcare System?
Key Takeaways Rising costs and climate pressure make building a sustainable healthcare system a core business and risk strategy decision. Learn the key principles of sustainable healthcare system development, including prevention, efficiency, equity, and social sustainability. See how AI, data platforms, and a sustainable digital system in healthcare cut waste, improve outcomes, and stabilize workforce…

Medical Device Software Integration: A Strategic Buyer’s Guide for Healthcare Enterprises
Key takeaways: Medical device software integration is a governance decision first. Define data ownership, clinical workflows, and regulatory scope before writing a single API. Build on recognized standards from the outset. FHIR, DICOM, and IEEE 11073 reduce ambiguity and simplify long-term scaling. Expect validation and security to drive real cost. Documentation, testing, and firmware controls…