- Key Principles of Sustainable Healthcare Systems
- Business Benefits of Building a Sustainable Healthcare System
- Sustainable Healthcare System Cost: What Should Enterprises Plan For?
- Challenges and Solutions in Sustainable Healthcare Development
- The Role of Technology in Sustainable Healthcare Systems
- Strategic Roadmap for Enterprises for Building a Sustainable Healthcare System
- Future Trends of Sustainable Healthcare Systems Leaders Should Track
- How Appinventiv Can Help in Building a Sustainable Healthcare System?
- Frequently Asked Questions
Key Takeaways
- Rising costs and climate pressure make building a sustainable healthcare system a core business and risk strategy decision.
- Learn the key principles of sustainable healthcare system development, including prevention, efficiency, equity, and social sustainability.
- See how AI, data platforms, and a sustainable digital system in healthcare cut waste, improve outcomes, and stabilize workforce capacity.
- Get a step-by-step roadmap to redesign care models, infrastructure, and technology around long-term healthcare sustainability goals.
Every quarter, your finance team signs off on bigger healthcare bills. Outcomes, however, are not growing at the same pace.
According to WHO and OECD estimates, sustainability in healthcare is critical as the sector already consumes close to a tenth of global GDP, and costs are still climbing. Yet many systems still rely on energy-hungry buildings, manual workflows, and episodic care that reacts late instead of acting early. These models are expensive to maintain and fragile in a world of aging populations and climate risk.
A sustainable healthcare system looks very different. It aligns clinical outcomes, financial performance, environmental impact, and social responsibility in one operating model.
These efforts also align with global frameworks such as SDG 3 (Good Health and Well-being), reinforcing healthcare sustainability as both a business and societal priority.
It treats prevention, smart infrastructure, and workforce well-being as balance sheet issues, not side projects. For an enterprise leader, that is not a branding conversation. It is a long-term risk and profitability decision.
Digital sustainability in healthcare and AI-enabled systems sit at the center of this shift. The way you design software, data flows, and care journeys will decide whether sustainability becomes a real capability or another presentation slide.
In this blog, we will unpack the core principles, business benefits, key challenges, enabling technologies, and a practical digital transformation roadmap for sustainable system development with the right digital product engineering partner.
Use sustainable digital systems to bend your cost curve, not just negotiate it.
Key Principles of Sustainable Healthcare Systems
Healthcare is already one of the most expensive lines on the national P&L. The United States spends about 16.6% of its GDP on healthcare, compared to 12.7% in Germany, the next highest spender. That gap is not just a policy problem; it is a signal that current models are structurally inefficient.
For C-level leaders, a sustainable healthcare system is not a slogan. It is a set of operating principles that brings clinical outcomes, financial performance, environmental impact, and social responsibility into one strategy.
Before talking about technology rollouts or new facilities, these principles form the blueprint for sustainable system development. Below are the core pillars you need to pressure test your current healthcare sustainability strategy against.

1. Core Principles
At the foundation of any sustainable system are non-negotiable ways of thinking about care and operations.
1. Prevention and Proactive Care
A sustainable healthcare system shifts focus from reactive treatment to prevention and early intervention. Enterprise leaders are increasingly using Social Determinants of Health (SDOH) data, such as housing, income, nutrition, and transportation, to uncover non-clinical risk factors behind readmissions.
By combining SDOH insights with clinical and population health data, AI models build whole-person risk profiles and enable targeted interventions before conditions escalate. This approach reduces avoidable admissions, improves value-based care performance, and supports innovative healthcare business models.
2. Efficiency and Resource Optimization
Once prevention becomes a focus, the next question is how efficiently the system uses its resources.
Most health systems lose value in silent pockets of waste. Duplicate tests, idle capacity, unnecessary admissions, manual reconciliations, and poorly planned purchasing all erode margins.
Sustainable healthcare practices focus on process redesign and better use of data. The goal is to cut waste in energy, consumables, and administrative effort without compromising care quality. This is where lean thinking and predictive analytics-driven healthcare operations become central to healthcare sustainability.
2. Sustainability in Healthcare
Building on those foundations, healthcare sustainability shows up in how you design infrastructure, care journeys, and financing logic.
1. Environmental Stewardship
Hospitals are among the most resource-intensive buildings in any city, making a sustainable system for hospitals essential. They consume large amounts of energy, water, and single-use materials. Healthcare sustainability through environmental stewardship is now a board-level topic, not an engineering footnote.
A sustainable healthcare model prioritizes energy-efficient facilities, smarter supply chains, and structured waste management. That includes everything from HVAC upgrades and smart lighting to better operating room scheduling and reduced reliance on disposable items where safe alternatives exist.
Many healthcare providers are also aligning with standards such as ISO 14001 to formalize environmental management practices across energy use, waste handling, and resource efficiency.
2. Patient Centric Care
Once the physical footprint is addressed, the next layer is how patients actually experience the system.
Healthcare sustainability is also about making it easier and safer for people to get care. Telemedicine, EHR systems, remote monitoring, and digital triage tools reduce unnecessary travel and waiting and free clinical teams to focus on higher-value interactions.
When care journeys are designed around patient needs and context, you see fewer avoidable complications, faster interventions, and higher engagement.
3. Financial Sustainability (Principle Level)
Even the best-designed initiative fails if it cannot be funded over time. Financial sustainability is about building a system that can maintain reach and quality under real-world budget pressure.
At a principal level, this means transparently understanding cost drivers, shifting spend from late-stage acute care to earlier, lower-cost interventions, and avoiding technical debt from short-term fixes. Detailed ROI comes later, but the direction of travel must be clear.
3. Key Pillars of a Sustainable Healthcare Model
Translating principles into a working model requires a few structural pillars that shape every major decision.
1. Equity and Access
If sustainability only works for urban, well-insured populations, it is not sustainable. Equity and access are structural pillars. Models must be designed to reach underserved communities, rural regions, and vulnerable groups in a viable way.
This can mean decentralized care hubs, mobile clinics, virtual care models, and language or culture-aware digital experiences. For leadership teams, equity is no longer just policy language; it is a design constraint for any serious healthcare sustainability initiative.
2. Technological Integration
A sustainable healthcare system treats technology as core infrastructure, not an add-on. Using interoperable platforms, AI, and secure data layers, enterprises embed digital capabilities directly into care and operations.
Utilizing FHIR R4/R5 and HL7 standards ensures data liquidity, seamless system interoperability, and reduces the technical debt created by fragmented legacy environments. This enables scalable digital health solutions, strengthens compliance, and allows new services to be deployed faster without rebuilding foundational architecture.
3. System Sustainability
System sustainability focuses on building healthcare models that remain stable, adaptable, and cost-efficient under long-term pressure. It requires interoperable architectures, resilient supply chains, and governance frameworks that can scale across facilities without increasing complexity.
For enterprises, this ensures continuity of care, financial predictability, and the ability to absorb shocks such as demand spikes, policy shifts, or public health crises.
4. Social Sustainability
Beyond infrastructure and technology, sustainable healthcare also depends on the health of the social fabric around the system.
1. Community Well Being and Inclusion
Social sustainability in healthcare is about the relationship between the system and the communities it serves. It requires involving local stakeholders in how services are designed, delivered, and communicated.
That may include community advisory groups, listening programs, co-designed care pathways, and services adapted to local realities. When communities see their priorities reflected, trust increases, and care plans are more likely to be followed, which strengthens long-term system sustainability.
2. Staff Well-Being and Capacity Building
The other half of the social equation sits inside the walls of the organization.
No sustainable healthcare system can be built on an exhausted workforce. Staff well-being, career development, and local employment are not HR side topics; they are sustainability levers.
This principle covers reducing burnout through better staffing models and tooling, creating clear upskilling paths for digital care, and investing in local talent rather than relying only on imports.
For executives, treating workforce health as part of healthcare sustainability is often the difference between a strategy that looks good on slides and one that can actually scale.
Business Benefits of Building a Sustainable Healthcare System
With sustainability in healthcare industry becoming critical as healthcare spending climbs to 20.3 percent of GDP by 2033, cost control by negotiation alone will not be enough. Leaders will need sustainable healthcare solutions that bend the curve structurally, not just cosmetically. That is where the benefits of developing sustainable healthcare software and systems start to show up.
1. Cost Optimization and Long-Term Savings
Sustainability in hospitals is enabled by resource orchestration. AI-driven predictive staffing aligns workforce supply with patient demand, reducing overstaffing and reliance on expensive locum and agency staff — a major P&L drain for hospital chains. Smarter facilities, connected assets, and automated workflows further reduce energy, infrastructure, and administrative costs without affecting clinical quality.
2. Higher Quality of Care and Better Outcomes
Sustainable models emphasize predictive analytics, early interventions, and continuous monitoring. That reduces avoidable admissions and complications, while giving clinicians a more complete view of each patient at the point of decision.
3. Stronger Patient Trust and Brand Reputation
Patients and payers notice organizations that take healthcare sustainability seriously and make access easier through digital channels. Consistent experiences, shorter journeys, and transparent communication translate into higher loyalty and better word of mouth.
4. Workforce Stability and Staff Well-being
When digital tools remove repetitive admin and clarify workflows, clinicians get more time for actual care. That improves engagement, reduces burnout, and makes the organization more attractive to scarce talent.
5. Regulatory, ESG, and Scalability Advantages
Sustainable digital healthcare systems simplify compliance with CSRD (Corporate Sustainability Reporting Directive) and local ESG mandates by automating sustainability data collection and generating audit-ready reports. Standardized digital platforms also enable enterprises to scale across facilities and service lines without proportionally increasing cost, risk, or operational complexity.
6. Talent Attraction and Retention Through Sustainability Commitments
Public sustainability commitments, such as the U.S. Department of Health and Human Services Climate Pledge and net-zero targets, signal purpose and stability to clinical talent.
Organizations that embed sustainability into operations see stronger attraction, lower burnout, and improved long-term retention.
Sustainable Healthcare System Cost: What Should Enterprises Plan For?
When you start planning a sustainable system, the sticker shock usually comes first. For a mid to large healthcare enterprise, initial programs often start in the $500,000 to $2 million range for focused pilots, and can reach $5 to $15 million or more for multi-year, multi-site rollouts.
These are not fixed prices. The Cost of sustainable healthcare system depends heavily on your digital maturity, number of facilities, regulatory landscape, and how ambitious your roadmap is. But most budgets break down into a similar set of components.
Key cost components and indicative ranges
Ranges below are directional, for mid to large enterprises, and assume a multi-year horizon.
| Cost Component | Indicative Cost Range ($) |
|---|---|
| Digital platforms and data layer | $500,000 to $4,000,000 |
| Infrastructure and green IT | $1,000,000 to $8,000,000 |
| Care model redesign and clinical programs | $300,000 to $2,000,000 |
| Change management and workforce development | $250,000 to $1,500,000 |
| Governance, compliance, and measurement | $150,000 to $800,000 |
In the early stages, most of the spend sits in digital platforms, integration, and data. As your sustainable digital system in healthcare matures, more investment shifts toward care model redesign, workforce programs, and green infrastructure.
The right way to view the cost of the sustainable healthcare system is in net terms, not just as new spending. Over a three to five-year window, reductions in readmissions, energy use, paper-based processes, manual reconciliation, and turnover can offset a meaningful share of the upfront investment.
The real risk is not the spending itself, but spending in a fragmented way without a clear roadmap or governance, which is where most overruns and stalled programs happen.
Challenges and Solutions in Sustainable Healthcare Development
Even beyond the United States and Germany, 15 high-income countries, including Canada, France, and Japan, already spend more than 10 percent of their GDP on healthcare.
In that context, sustainable healthcare system development is easy to discuss but harder to fund, execute, and maintain.
Below are the main barriers most enterprises face, with practical ways to offset each one.
1. Cost of Transition
The shift to a sustainable healthcare system demands upfront spend on digital platforms, data infrastructure, facility upgrades, and change management. For many boards, this looks like a new cost layer on top of an already heavy P&L.
A pragmatic path is to treat sustainability as an investment portfolio, not a single mega program. Start with high-impact, low-friction pilots, link each to clear efficiency or revenue metrics, and gradually recycle savings into the next wave. Cloud-based sustainable healthcare solutions and managed services can also convert large CapEx into more predictable OpEx.
2. Fragmented Healthcare Systems
Many enterprises still operate as disconnected units. Data sits in silos, processes vary by site, and patients feel the fragmentation across every transition of care. This multiplies cost and makes sustainability initiatives difficult to scale.
The solution is coordinated digital transformation and legacy system modernization, not new standalone tools. Most healthcare enterprises are not rebuilding from scratch. They are strangling the monolith by incrementally modernizing legacy cores, adopting shared data standards, and implementing platform-based architectures that allow new solutions to plug in without repeatedly rebuilding the foundation.
3. Regulatory Complexity
Sustainability in the healthcare industry requires leaders to navigate a maze of privacy, security, and environmental regulations. HIPAA, GDPR, local data residency rules, and green building standards can make transformation feel risky and slow. The result is often defensive decision-making and stalled projects.
Embedding compliance into the architecture from day one changes the equation. Privacy by design, standardized security frameworks, audit-ready logging, and automated reporting reduce risk while speeding approvals. Partnering with teams that understand both digital health and regulatory environments helps you move faster without surprises later.
4. Community Engagement Gaps
Sustainability efforts can fail if communities see them as imposed from outside. Low trust, cultural mismatch, or poor communication can lead to low adoption of new care models, especially in rural or underserved areas.
Treat communities as co-designers, not just recipients. Use local advisory panels, patient councils, and targeted digital channels to listen before you deploy. Co-created services, localized content, and decentralised touchpoints make sustainable models more relevant and much more likely to stick.
5. Workforce Issues
High turnover, burnout, and limited training capacity are already hurting many health systems. Adding new technology and processes on top of this reality can increase resistance and fatigue rather than solving the problem.
The answer is to put staff well-being at the center of the change plan. Choose tools that genuinely reduce cognitive load, redesign workflows with clinicians in the room, and invest in structured training and mentoring. When people see that sustainability also improves their day-to-day reality, adoption stops being a compliance exercise.
6. Access to Resources
Not every region has the same access to capital, talent, or infrastructure. Investing heavily in high-end technology while primary care, outreach, or local facilities remain underdeveloped can actually widen inequities.
A more balanced strategy pairs digital investments with support for primary and community care. Public–private partnerships, shared service centers, and regional “digital front doors” can extend specialist capacity without requiring a full hospital in every location. This keeps sustainability grounded in real access, not just better numbers on a dashboard.
In the next section, we will look at how specific technologies – AI, analytics, cloud, and digital care platforms – can directly address these challenges and enable a more sustainable operating model.
The Role of Technology in Sustainable Healthcare Systems
The Centers for Medicare & Medicaid Services are already pushing care into lower-cost settings.
McKinsey estimates these models can cut the total cost of care by 8 to 10 percent or more. That type of structural shift is almost impossible without technology doing the heavy lifting behind the scenes.
Digital sustainability in healthcare is not just about going paperless. It is about using data, software, and cloud infrastructure to redesign where and how care happens.
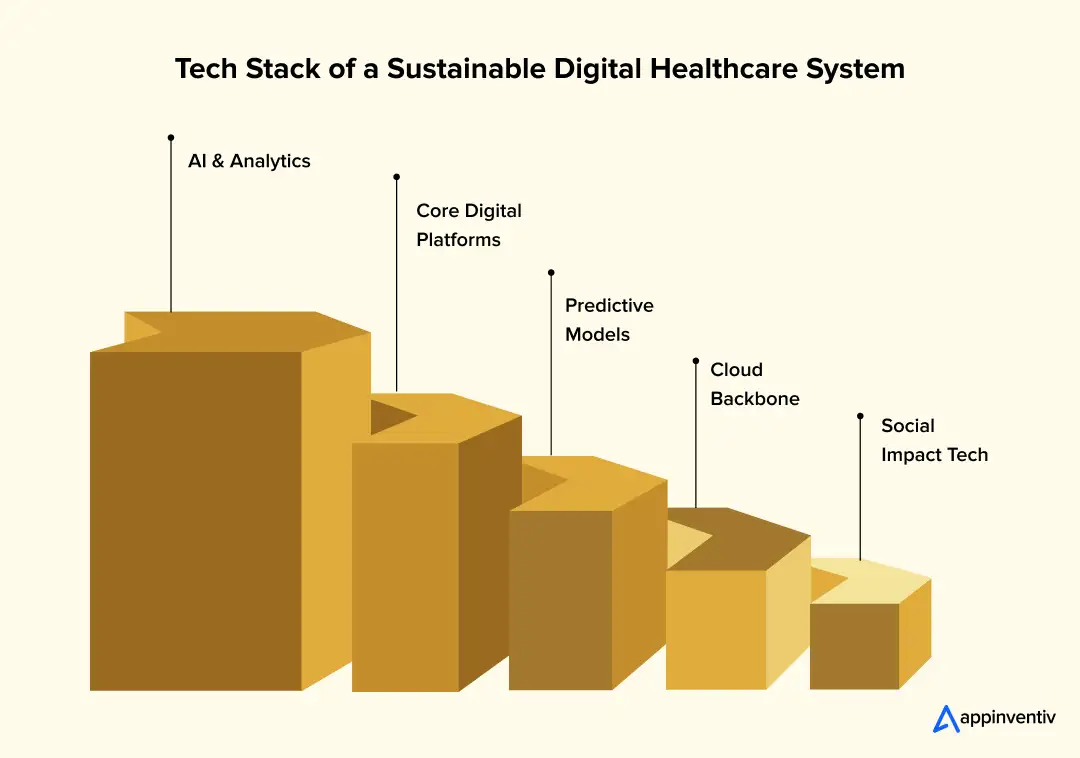
1. Technology As The Key Enabler
At the system scale, technology is the only way to make sustainable healthcare practices repeatable and measurable.
AI and Data Analytics
AI-powered risk scoring, digital triage, and capacity planning help you move patients into the right setting at the right time. Instead of waiting for deterioration, population health analytics flag rising risk early and guide proactive outreach.
This is where AI in healthcare sustainable systems becomes practical. It supports clinicians with better insight, reduces avoidable admissions, and helps planners match staffing and bed capacity to real demand.
Also Read: Navigating the AI Challenges in Healthcare – Insights and Success Strategies for Enterprises
Sustainable Digital Healthcare Systems
EHRs, AI-powered telemedicine platforms, remote monitoring tools, and patient apps form the backbone of a sustainable digital system in healthcare. They reduce friction in handoffs, cut down on repeat data entry, and shrink the need for physical visits when a virtual interaction is enough.
When these systems talk to each other, you reduce waste in time, travel, and materials. Care becomes more accessible, and the operational footprint gets lighter at the same time.
2. Specific Technologies Driving Change
Different technologies play different roles, but together they create the operating layer for sustainable healthcare.
Analytics and Machine Learning in Healthcare
Predictive models help identify which patients are likely to be readmitted, which pathways are prone to bottlenecks, and where inventory will run short.
Used well, they reduce preventable admissions, smooth care pathways, and support chronic disease management at scale. That is central to a sustainable healthcare system that does more upstream and less in crisis mode.
Cloud Solutions for Healthcare
Cloud platforms give you a common, secure foundation for applications, data, and analytics. They allow you to scale services across regions without replicating hardware in every facility.
From digital sustainability in healthcare perspective, consolidating infrastructure and using elastic capacity can reduce both cost and carbon intensity per transaction. It also makes it easier to roll out new services quickly, rather than waiting for long hardware cycles.
3. Social Sustainability Through Technology
Technology also has a social role to play, well beyond core efficiency metrics.
Community Engagement Strategies
A sustainable system for hospitals includes community health apps, regional telehealth hubs, and localized digital education that bring services closer to people. Two-way digital channels make it easier to listen, adapt services, and build trust over time.
When communities see that digital tools speak their language, reflect their reality, and reduce effort for them, adoption of new care models improves significantly.
Supporting Local Employment and Skills
Sustainable healthcare systems also create new roles in digital health operations, healthcare data management, and remote care coordination. With the right training, many of these roles can be based in local communities, not just central headquarters.
That combination of better access, stronger trust, and new career paths makes social sustainability more than a talking point.
These technologies are powerful, but they only deliver their full value when deployed in a clear, phased way. The next section looks at a practical roadmap for leaders who want to build a sustainable system without losing control of risk or cost.
From patient apps to data platforms, we build systems that support long-term healthcare sustainability.
Strategic Roadmap for Enterprises for Building a Sustainable Healthcare System
Deloitte estimates that healthcare accounts for 5% of global greenhouse gas emissions. In the meantime, clinical demand, regulatory pressure, and expectations regarding costs are also increasing.
Sustainable healthcare system development requires not a single flagship project but a collection of conscious, well-managed actions across technology, infrastructure, people, and data.
We are sharing here a practical roadmap that you may adjust; this is based on sustainability thinking and enterprise architecture thinking.
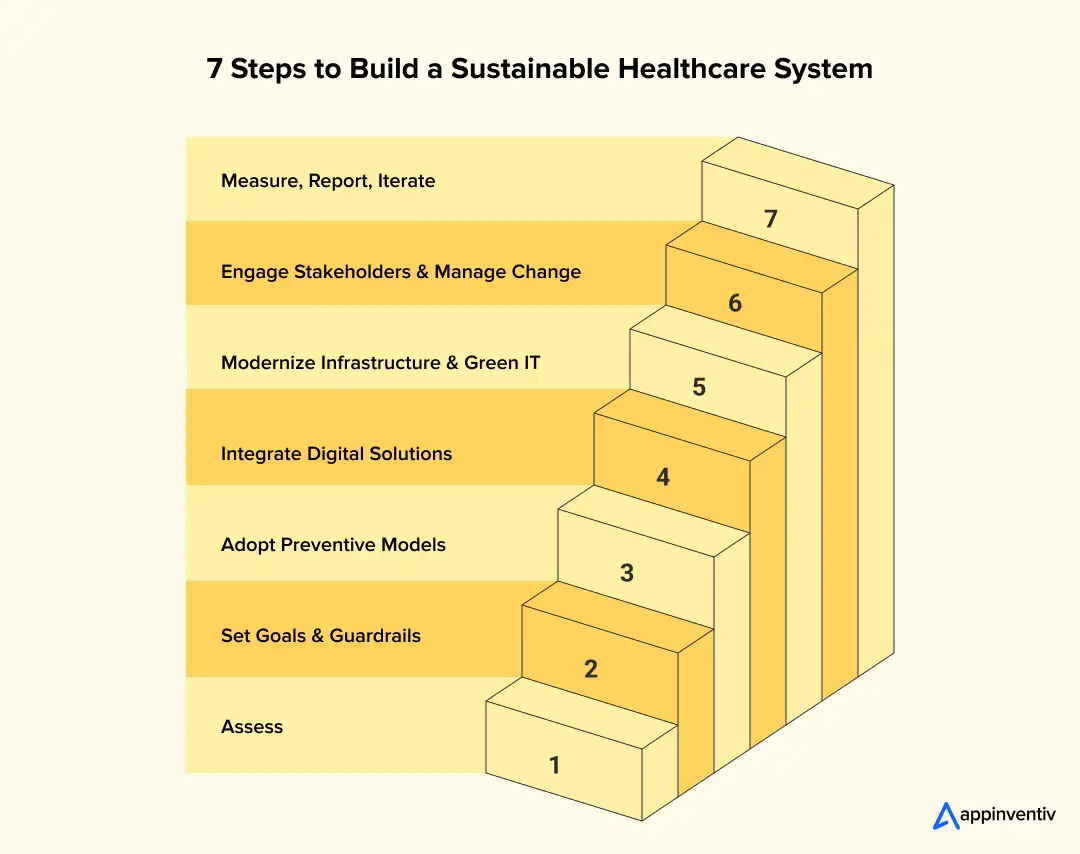
Step 1: Evaluate the Sustainability of the Existing System
Open with a systematic test, not independent audits. Combine operational, clinical, and technology perspectives into a single platform.
Asset map, application, data flows and facility profile. Develop a standardized model to record energy consumption, water use, waste, equipment age, computer maturity, employee experience, and community impact. System maps, data lineage diagrams, and process mining tools may indicate where the actual sources of waste and friction are located.
Step 2: Establish Effective Sustainability Objectives and Architecture Guardrails
Once baseline data is available, convert sustainability from a corporate message into an enterprise architecture discipline. Establish quantifiable environmental, financial, and social performance targets, such as energy use per bed, readmission rates, or staff overtime levels.
Simultaneously, define technical guardrails, including preferred cloud platforms, security baselines, interoperability standards in healthcare (FHIR/HL7), and data residency policies.
Add carbon-aware computing as a core principle: selecting cloud regions powered by greener energy grids and optimizing software architectures and code to reduce CPU cycles and energy consumption. These guardrails shape every future initiative.
Step 3: Adopt Preventive Care Models, Data, and AI-driven Approaches
The greatest structural benefits are associated with upstream care shifting. It refers to intervening earlier, using data and models, at a lower cost.
Implement population health analytics to stratify patients. Plug AI-generated risk scores of conditions such as heart failure, diabetes, or COPD in outreach workflows.
This could technically require a data platform that consolidates EHR data, claims, and remote monitoring feeds into a single controlled repository. The objective is simple: fewer emergencies, more managed, foreseeable treatment.
Step 4: Unite Sustainable Healthcare Solutions into a Single Most Logical Platform
The digital tools foster sustainability in a collaborative flow. This is where strategies fail most of the time.
Create a small hub of anchor platforms on which your sustainable digital health system will be established. This typically consists of an interoperable EHR, a telehealth offering, a remote monitoring feature, and a single interface for communicating with patients, such as a portal or an application.
Design integration patterns early, based on APIs, integration engines, and event-driven communication rather than point-to-point interconnections. Develop effective data management to ensure quality, rights to access, and lineage are visible.
Step 5: Pay Attention to Infrastructure and Green IT Issues
For sustainability in hospitals, digital programs and infrastructure improvements should not be treated as separate worlds; they influence each other.
Build a sustainable system for hospitals by modernizing with high-quality HVAC, lighting, and smart building technology that provides actionable information. On the IT front, centralize servers to more eco-friendly cloud or hybrid server implementations, streamline unnecessary applications and exploit virtualization and containerization to drive higher usage.
Plot these tracks on a shared roadmap so you do not waste money on physical infrastructure upgrades for systems that are going to be retired.
Step 6: Change Management and Stakeholder Intervention
The roadmap will not succeed if clinicians, staff, and communities in the local area feel they have been forced into changes. Change management is not an email campaign, and it requires a plan.
Form multidisciplinary design teams that contain clinical leaders, operations, IT, and community representatives; apply service design tools, journey mapping, and pilots to prototype new models at scale.
Adopt by training, build a network of super users, and provide a clear escalation path for non-functional issues. Benefits in sustainability that simplify the day-to-day work will gain traction faster more than formal communications alone.
Step 7: Operating Discipline Cycle of Measuring, Reporting, and Reiterating
Lastly, manage sustainability like quality or safety: it will need dashboards, governance and continuous improvement. Develop a small yet strong environment, cost, outcome, workforce, and community metrics.
Create key systems on instruments such that data automatically gets into your reporting layer. Consider those indicators regularly at the executive level, not only during project reviews. These are used to determine what to upscale, what to suspend and where to test out next.
Over time, this changes sustainability as a project portfolio into a property of the project: how your healthcare system is designed, engineered, and operated.
Future Trends of Sustainable Healthcare Systems Leaders Should Track
Healthcare sustainability is a moving target. To keep current investments relevant, leaders need a view of where sustainable healthcare systems are heading next. Some of the key future trends include:
- AI native operations: AI embedded into triage, capacity planning, documentation, and risk scoring, not just running as side pilots.
- Virtual first and decentralized care: Home hospital, remote monitoring, and community hubs reducing dependence on large central facilities.
- Climate resilient, low-carbon infrastructure: Hospitals and clinics planned around energy efficiency, resilience to climate events, and real-time building intelligence.
- Interoperable data ecosystems and ESG-linked models: FHIR first architectures, shared data platforms, and contracts or financing that increasingly reward measurable sustainability performance.
These trends will raise the bar on digital maturity and execution. Enterprises that invest now in a clear, scalable, sustainable system will be better positioned as these expectations become the norm rather than the exception.
Also Read: Top Healthcare Trends That Will Redefine The Industry in 2025
Share your current challenges and get a tailored blueprint for your enterprise health system.
How Appinventiv Can Help in Building a Sustainable Healthcare System?
Appinventiv, a top healthcare software development services company, partners with healthcare enterprises that want sustainable healthcare solutions to strengthen clinical outcomes, operational efficiency, and long-term sustainability in one shot.
- 500+ digital health platforms delivered
- 450+ healthcare clients served
- 10+ years in HealthTech projects
Our work spans patient platforms, provider tools, remote monitoring, and data products designed for scale, security, and compliance. Here are sustainable healthcare use cases with visible impact in real numbers:
- Health-e-People: A dynamic health data platform that aggregates records from 200+ devices and apps into a single view for users and caregivers, improving continuity of care and reducing fragmentation in data access.
- Soniphi: A voice-driven wellness app that uses 94% of vocal input for real-time analysis and has been adopted by millions of users for proactive health monitoring, reducing dependence on high-intensity in-person visits.
- Diabeticu: A HIPAA-compliant diabetes management platform that now supports tens of thousands of patients with AI-powered recommendations, prescription tracking, and remote consultations, shifting care from episodic to continuous
- YouComm: An in-hospital patient communication system now live across 5+ hospital chains in the US, delivering a 60% improvement in nurses’ real-time response time, easing staff load and improving bedside experience
These real-world sustainable healthcare examples touch core sustainability levers: better access without always expanding physical footprint, more efficient use of clinical capacity, and reduced strain on infrastructure and staff.
If your next step is to translate a high-level sustainability vision into concrete digital initiatives, we can help you design, build, and scale a sustainable healthcare system tailored to your enterprise.
Let’s connect and start a sustainability readiness conversation.
Frequently Asked Questions
Q. What is sustainable healthcare?
A. Sustainable healthcare refers to a system in which there is the management of clinical outcomes, costs, environmental impact, and social responsibility as a single system.
It is concerned with prevention, smarter resource use, greener infrastructures, and equitable access to care. It is not to achieve short-term fixes but long-term performance.
In practice, that implies the integration of sustainable healthcare practices with digital tools, data, and workforce strategies rather than viewing them as individual projects.
Q. What are the four pillars of sustainable healthcare?
A. A sustainable healthcare system is built on four pillars:
- Prevention – changing the late-stage therapy to early diagnosis and continuous treatment.
- Efficiency – eliminating wastes in processes, infrastructure and supply chains.
- Equity – accessibility and relevance to all populations, and not only the ones to serve with ease.
- Resilience – creating systems which can absorb shocks like pandemics, climate shocks or shifts in funding.
A sustainable healthcare model can only succeed when the four pillars are factored into its strategy, design, and technology choices.
Q. How can the healthcare system deliver sustainable performance?
A. Care, operations, and technology alignment are the sources of sustainable performance based on goals.
At the system level, that typically entails: investing in preventive and community-based care, integration of digital platforms, infrastructure modernization and data-centered workflow redesign.
Then executives consider sustainability a discipline of operation, complete with goals, responsibility, and periodic review, rather than a sequence of disparate activities.
Q. How to measure sustainability in healthcare?
A. It should be measured on the environmental, financial, clinical, workforce, and community dimensions.
Common measures are energy and water consumption per bed or visit, volumes of waste, cost per episode or per member, readmission and complication rates, staff turnover and burnout indicators and access measures of underserved populations.
An effective healthcare sustainability strategy will characterize a lean, stable KPI list, automate as much data capture as possible, and discuss performance on the board or executive level.
Q. What is regulatory compliance for a sustainable healthcare system?
A. It must not violate the rigid rules of privacy, security, clinical safety, or the environment.
On the digital front, that translates to the frameworks of HIPAA, GDPR, local legislation of data residency, medical device standards, and cybersecurity standards. Physically, it may involve the green building codes and emission targets.
The best is compliance by design. These requirements are integrated into architecture, data governance, and process design at the beginning, so sustainability, risk, and regulation cannot be directed towards each other.
Q. What is the typical ROI timeline for sustainable healthcare investments?
A. Typical ROI for sustainable healthcare investments is realized over 2 to 5 years, depending on scope and maturity. Early gains (6–18 months) come from operational efficiencies like reduced admin costs and energy savings, while larger returns from preventive care, workforce optimization, and infrastructure modernization compound over time, delivering sustained financial and clinical impact.


- In just 2 mins you will get a response
- Your idea is 100% protected by our Non Disclosure Agreement.

EHR Implementation for Healthcare Providers: Process, Features, and Total Cost Analysis
Key takeaways: A clear EHR implementation guide keeps teams on track and prevents delays. The full EHR implementation process includes planning, setup, moving data, training staff, and regular updates. The right features handle clinical work, billing, reports, and compliance for large healthcare organizations. EHR implementation costs vary based on design, integrations, data migration, training hours,…

Medical Device Software Integration: A Strategic Buyer’s Guide for Healthcare Enterprises
Key takeaways: Medical device software integration is a governance decision first. Define data ownership, clinical workflows, and regulatory scope before writing a single API. Build on recognized standards from the outset. FHIR, DICOM, and IEEE 11073 reduce ambiguity and simplify long-term scaling. Expect validation and security to drive real cost. Documentation, testing, and firmware controls…
How to Build a Custom Pediatric EMR and EHR System?
Key takeaways: Clinical Precision: Custom systems accommodate pediatric-specific data points like percentile curves and weight-based longitudinal dosing. Interoperability: Seamless data exchange via HL7 FHIR ensures your practice stays connected to pharmacies, labs, and state registries. Regulatory Resilience: Built-in compliance with HIPAA, HITECH, and MACRA/MIPS reduces legal friction. Enhanced Engagement: Parent portals reduce administrative overhead by…