- Importance and Role of Change Management in the Healthcare Industry
- Core Components of Healthcare Change Management
- Change Management Theory and Models in Healthcare
- Change Management Process in Healthcare Transformation
- Governance, Roles, and Accountability in Healthcare Change Management
- Change Management Tools and Techniques Used in Healthcare
- Barriers to Change Management in Healthcare and How to Work Through Them
- Change Management in Healthcare: Real-World Examples
- Best Practices for Effective Change Management in Healthcare
- Future Trends in Healthcare Change Management
- How Appinventiv Supports Healthcare Transformation
Key Takeaways
- Change in healthcare fails quietly when ownership, workflow alignment, and follow-through are missing.
- Successful change management in healthcare focuses on adoption, not just system implementation.
- Clinical workflows and workforce capacity determine whether transformation sticks or stalls.
- Governance, clear accountability, and post-go-live support matter more than the model used.
- Sustainable healthcare transformation depends on steady leadership, realistic pacing, and measurable outcomes.
Healthcare rarely stands still. New systems, new policies, and rising expectations from patients, regulators, and payers are constant. On paper, most of these changes are well-intentioned. In practice, many struggle to take hold, not because teams lack commitment, but because the change itself is poorly managed. This is especially critical in change management in healthcare IT, where system upgrades and digital rollouts directly reshape clinical workflows and data flow.
By 2026, more than 30% of healthcare leaders globally expect AI to materially transform roles and workflows in their organizations, reshaping how clinical and administrative tasks are performed, a shift that highlights why human‑centered change management is now essential, not optional, in the industry.
This is where healthcare change management processes become critical. Unlike other industries, change here affects real people in real moments. A new workflow can slow a clinician. A poorly timed rollout can disrupt care. What looks efficient in a boardroom can feel unworkable on the floor. That is why healthcare change management cannot be treated as a checklist or a communication plan. It has to account for behavior, pressure, safety, and trust.
As organizations move toward modernization, change management processes in healthcare transformation are no longer optional. Digital tools, care redesign, and operational shifts depend on adoption, not just implementation. When change is rushed, it adds to burnout and resistance. When it is handled with intent, it becomes a stabilizing force rather than another disruption.
This guide looks at how change management healthcare teams can move from planning change to making it stick in everyday operations.
Align leadership, clinical workflows, and digital systems with a structured change management framework designed for enterprise healthcare environments
Importance and Role of Change Management in the Healthcare Industry
The value of change management processes in healthcare usually becomes clear after a problem surfaces. A new system rolls out, slowing clinics down. A policy update lands without enough explanation. People adjust in their own ways, and not always in the ways leaders expected. Care still happens, but it feels harder than it should.
That is where the role of change management in the healthcare industry really sits. Healthcare organizations cannot stop delivering care while they figure things out. Patients still arrive. Clinicians still carry responsibility. Regulations do not ease up. Change management healthcare teams help organizations move forward without losing control of everyday operations. Their job is not to push change faster, but to introduce it in a way people can realistically absorb.
In practice, change management shows up in small but important ways:
- Giving teams context before change, not after
- Allowing clinicians time to adapt instead of forcing overnight shifts
- Reducing confusion by clarifying what is changing and what is not
- Supporting new ways of working until they become routine
- Keeping care delivery stable while improvements take place
When they work, change management processes go unnoticed. There is less friction. Fewer workarounds and fewer frustrated conversations in hallways. Change feels manageable rather than disruptive. That is why it plays such a critical role today, not as an extra layer of process, but as a way to protect both people and care while organizations evolve.
Also Read: Healthcare Workforce Management Software
Core Components of Healthcare Change Management
In healthcare, change rarely fails all at once, and it drifts. A new system is introduced, but ownership feels unclear. Training is delivered, yet when shifts get busy, teams fall back on familiar routines. Over time, confidence weakens. This is where change management in healthcare organizations either create stability or slowly loses ground. These core elements reflect broader change management principles in healthcare, where accountability, clinical safety, clear communication, and sustained reinforcement matter more than speed.
What matters most is not which model is used, but whether the basics hold under pressure. When leadership stays visible, and clinicians are part of real decisions, change management feels grounded in daily work rather than layered on top of it.

Below are the components and aspects of change management in healthcare transformation that consistently make a difference.
1. Clear Ownership and Decision Paths
Someone has to own the change beyond approval meetings. In effective change management strategies in healthcare organizations, accountability is visible. Teams know who makes the call when trade-offs appear, how issues are escalated, and who stays engaged after go-live.
From a technical perspective, this includes clear control over system configurations, integrations, and risk approvals to ensure decisions do not stall.
2. Clinical Guardrails and Risk Awareness
Healthcare change affects patient safety. Even small workflow adjustments can alter documentation timing, handoffs, or alert patterns. Strong change management processes in healthcare transformation build in risk checks, clinical validation of redesigned workflows, and monitoring for unintended consequences. Guardrails prevent speed from overriding safety.
3. Real Communication and Workflow-Based Training
Generic communication rarely works. People want to understand why change is happening and how their roles are shifting. In strong change management efforts, communication is role-specific and transparent about trade-offs.
Training also mirrors real scenarios. Instead of ideal walkthroughs, teams practice documentation, order entry, or patient interactions in realistic conditions. This reduces friction once systems go live.
4. Post-Go-Live Support and Adjustment
Launch is not the finish line. It is when reality sets in. Effective change management in healthcare organizaitons include short stabilization windows, rapid issue tracking, and close monitoring of usage patterns. When workflows do not hold up, adjustments are made quickly rather than expecting staff to absorb the strain.
When these elements stay active, change management in organizations feels steadier. Change still requires effort, but it no longer feels careless or disconnected from how care is delivered. That steady approach is what allows transformation to last.
Also Read: The Essential Guide to Healthcare Mobile App Development
Change Management Theory and Models in Healthcare
Most healthcare leaders have heard the names of common change models. They show up in planning sessions, slide decks, and transformation roadmaps. The issue is rarely the theory itself. It is how that theory is used. Change management theory in healthcare only creates value when it is shaped around clinical realities, not applied as a fixed formula.
Healthcare does not operate in clean phases. Change happens alongside patient care, staffing shortages, regulatory demands, and technology limitations. A model that assumes steady conditions can fall apart quickly on the floor. That is why change management models in healthcare work best as guides, not instructions.
A few models appear most often in healthcare settings:
- Lewin’s model, which emphasizes preparing people before change, can feel too linear for environments where change never really pauses.
- Kotter’s model is useful for building leadership alignment and momentum during large programs, such as mergers or system-wide digital upgrades.
- ADKAR, which focuses on individual adoption and aligns well with the varied roles and responsibilities across healthcare teams.
In practice, change management in healthcare transformation teams rarely follows one model end to end. They blend elements based on context. ADKAR may shape clinician adoption, while Kotter supports executive sponsorship and funding decisions. Lewin’s idea of stabilization often becomes ongoing optimization rather than a final endpoint.
The real value of change management theory in healthcare is not in the steps themselves, but in what they help leaders notice. Where resistance is forming. Where adoption is stalling. When support is needed. Used this way, models stop feeling academic and start supporting real, technology-driven change without disrupting care.
Also Read: Importance of Digital Transformation in Healthcare
Change Management Process in Healthcare Transformation
In healthcare, transformation almost never fails because the idea was bad or the technology was weak. It struggles because people are asked to change while everything else stays just as demanding as before. Patients still need care. Shifts are still full. Systems still have limits. A workable change management process in healthcare accepts this reality instead of fighting it.
When change management processes in healthcare transformation work, it does not feel like a big “moment.” It feels like a series of deliberate, well-timed decisions that respect how work actually happens.
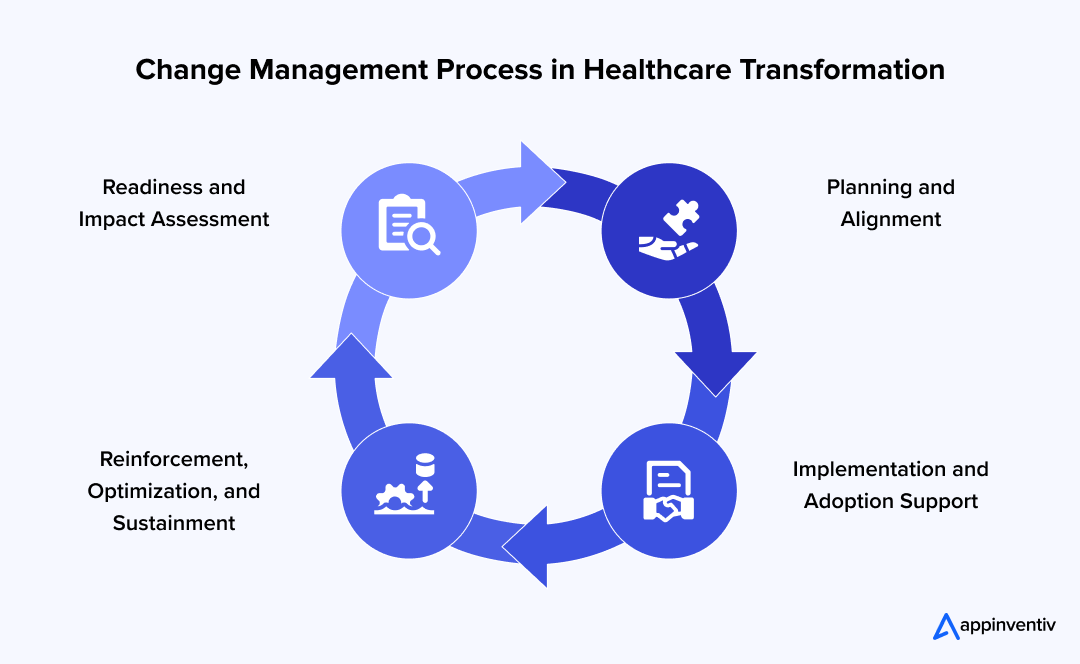
1. Readiness and Impact Assessment
This is the part many teams rush through, and later regret. Before timelines, vendors, or configurations are locked in, someone has to pause and ask hard questions about readiness.
At this stage, change management efforts focus on understanding:
- How work really flows during a busy day, not how it looks in process documents
- Where existing systems already slow people down or force workarounds
- Whether staff have the capacity to absorb another change right now
- What clinical, data, or compliance risks could surface once things shift
For technology-led initiatives, this also means carefully reviewing integrations, data quality, and dependencies. Skipping this step often turns small changes into big problems later.
2. Planning and Alignment
Once the starting point is clear, planning becomes less abstract and more practical. This is where change management processes in healthcare transformation move from intention to coordination.
Good planning is not about perfect timelines. It is about shared understanding:
- What is changing, what is not, and what is still uncertain
- How new systems or processes will affect real workflows
- Where leadership, IT, compliance, and frontline teams need to stay aligned
- Whether change should happen in phases or in smaller, controlled steps
Plans that ignore day-to-day realities tend to create quiet resistance, even if no one says it out loud.
3. Implementation and Adoption Support
This is where change becomes real. Systems go live, and processes shift. People try to do their jobs in new ways while the pressure stays the same.
During implementation, effective change management solutions for healthcare pays close attention to:
- Training that is tied directly to real tasks, not generic walkthroughs
- Clear ways for staff to raise issues when something does not work
- Support on the ground during early use, not just at launch
- Early warning signs like workarounds, delays, or frustration
For digital change, this often means short hypercare periods and tight feedback loops between IT teams and clinical leaders.
4. Reinforcement, Optimization, and Sustainment
In healthcare, go-live is not the end. It is when reality fully sets in. Edge cases appear. Teams adapt workflows. Systems are used in ways no one predicted.
This stage of the change management process in healthcare is about paying attention:
- Watching how adoption holds up weeks and months later
- Making small adjustments based on how work is actually done
- Folding changes into policies, onboarding, and daily routines
- Preventing a slow slide back to old habits once attention shifts
Handled well, change management solutions for healthcare transformation stop feeling like disruption piled on top of already hard work. Change still takes effort, but it feels supported, paced, and realistic. That is what makes it stick.
Implement healthcare transformation with clear governance, adoption tracking, and post-go-live optimization built for large-scale operations.
Governance, Roles, and Accountability in Healthcare Change Management
In healthcare, change rarely breaks during planning. It breaks later, when real work exposes gaps no one anticipated. A workflow does not hold up under pressure. A system behaves differently on a busy shift. Someone raises a concern, but it is unclear who should act. That moment of hesitation is where change management solutions for healthcare often lose momentum.
When governance works in healthcare system change management, it is almost invisible. People know where to take issues and trust that someone will respond. When roles are unclear, the opposite happens. Teams stop escalating problems and quietly build workarounds. Over time, those workarounds become the real process.
Most change management solutions for healthcare organizations already have the right roles in place. What matters is whether they stay present once things get uncomfortable:
- An executive sponsor who remains involved when priorities clash
- A clinical champion who speaks up when plans do not match real care delivery
- Someone is coordinating the change day to day, so messages do not drift
- IT and informatics teams staying close to how systems affect workflows
- Risk and compliance partners are involved early enough to prevent issues
Accountability is what gives these roles weight. In healthcare system change management, accountability is not about blame. It is about knowing who decides when trade-offs appear, where concerns go, and who stays responsible after go-live.
When governance and accountability are handled well, change management solutions for healthcare feel steadier. Decisions move with less friction. Issues surface earlier. Change is still hard, but it feels managed rather than dropped on teams already under pressure.
Also Read: A Complete Guide on HealthTech Regulations for CTOs
Change Management Tools and Techniques Used in Healthcare
In healthcare, no tool can “manage” change for you. A checklist will not calm a stressed unit. A dashboard will not convince a skeptical clinician. Tools only help if they reflect how work actually happens. That is where most efforts go wrong. The focus shifts from the people to the platform.
The most effective change management tools in healthcare are usually simple and grounded. They create visibility and surface friction early. They make conversations easier, not replace them.
In real-world settings, change management techniques in healthcare often look like this:
- Shadowing frontline staff before redesigning anything. Sitting in during a shift tells you more than any process document ever will. You see where delays happen and where people quietly compensate for system gaps.
- Role-specific impact sessions. Instead of announcing a change to everyone at once, leaders sit down with different groups and ask a direct question: “How will this affect your day?” The answers are rarely the same.
- Scenario-based training. Teaching through real patient cases, real documentation examples, and real-time pressure tends to land better than feature demonstrations.
- Short feedback cycles after go-live. A daily huddle, a shared issue log, or quick check-ins help teams speak up before frustration hardens into resistance.
- Looking at behavior, not just metrics. If a new feature is ignored or work slows down, it usually signals a workflow mismatch, not laziness.
In strong change management efforts in healthcare, tools support judgment. They help leaders notice what is happening beneath the surface. When change management solutions for healthcare relies only on polished emails and training slides, adoption feels forced. When practical tools are paired with listening and follow-up, change feels more manageable.
The point is not to gather more tools. It is to choose a few that make real work easier while everything else is shifting.
Barriers to Change Management in Healthcare and How to Work Through Them
Most healthcare changes do not fail because people reject them outright. They struggle because something underneath the surface is not addressed. The barriers to change management solutions for healthcare are rarely dramatic. They are subtle. A team nods in agreement during a meeting, but hesitates once the change affects their shift. A system goes live, but people quietly stick to old habits. That is where change management in healthcare either adapts or loses ground.
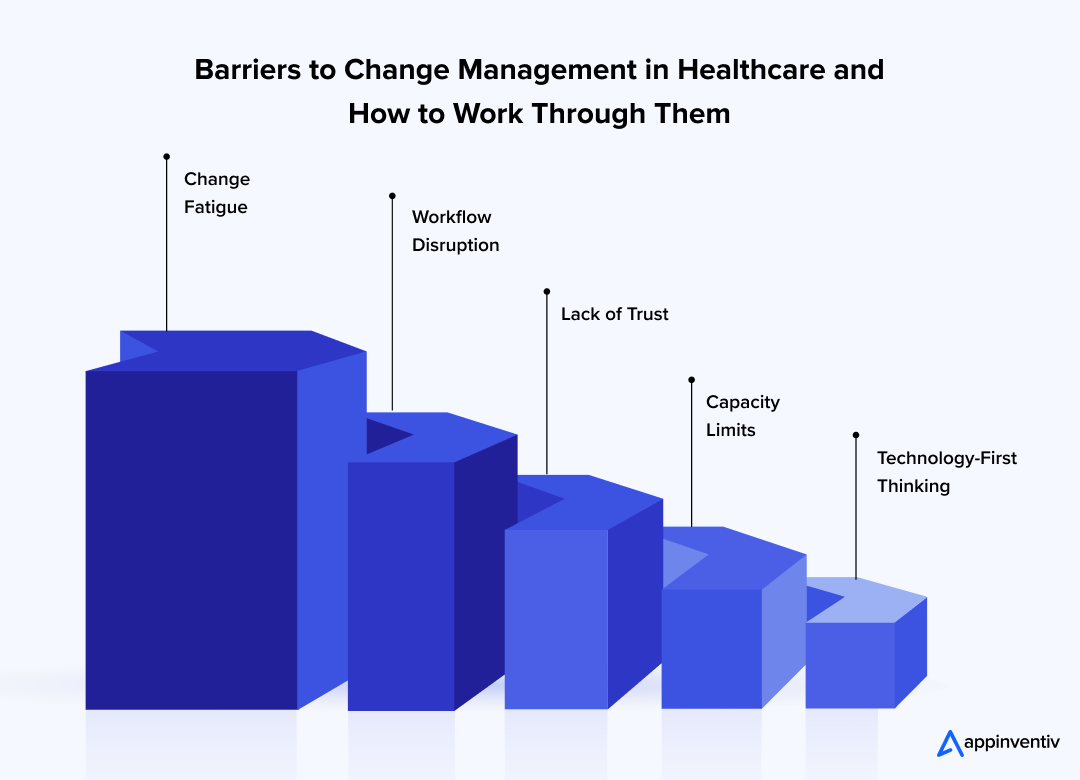
Here are some of the most common barriers and what tends to help in real settings.
1. Change Fatigue
Healthcare teams rarely deal with a single initiative at a time. When several projects overlap, even meaningful improvements can feel like one more demand.
What helps:
- Being honest about what can realistically be handled at once
- Spacing initiatives instead of stacking them
- Acknowledging workload strain instead of dismissing it
In healthcare system change management, pacing often determines whether people engage or withdraw.
2. Workflow Disruption
A change might be technically sound and still disrupt care. When a new system adds extra steps or slows documentation, frustration builds quickly.
What helps:
- Watching how work unfolds before redesigning it
- Testing changes during real, busy conditions
- Adjusting systems when they create friction instead of forcing adaptation
Effective change management efforts respect how work actually gets done.
3. Lack of Trust
If staff feel decisions were made without input or explanation, skepticism grows. Even well-intended change can feel imposed.
What helps:
- Explaining the reasoning behind decisions
- Involving frontline voices early
- Admitting trade-offs rather than presenting change as flawless
Trust is often the difference between compliance and real adoption in change management solutions for healthcare.
4. Capacity Limits
Many teams are expected to learn new systems while maintaining full patient loads. Over time, that pressure leads to quiet resistance.
What helps:
- Protecting time for training
- Watching for early signs of overload
- Accepting that slowing down briefly may prevent larger problems later
5. Technology-First Thinking
When digital initiatives focus only on features and timelines, the human side gets overlooked.
What helps:
- Pairing system rollouts with behavioral support
- Tracking how people actually use new tools
- Keeping clinical champions close to implementation decisions
In the end, barriers are not signs that change is impossible. They are reminders that people carry most of the weight in any transformation. When change management solutions for healthcare acknowledge those pressures and adjust accordingly, change feels less forced and more workable.
Also Read: Medical Practice Management Software Development
Change Management in Healthcare: Real-World Examples
Change in healthcare rarely looks dramatic from the outside. It usually unfolds in quiet ways, in how clinicians document, how teams coordinate, and how responsibilities shift. The following examples show that change management succeeds not because the idea was bold, but because leaders stayed involved long enough for the change to take root. Each example below functions as a practical change management in healthcare case study, showing how leadership, workflow alignment, and accountability influence real outcomes.
1. Mayo Clinic’s Enterprise EHR Transition
Mayo Clinic moved from hundreds of record systems to one enterprise-wide EHR. That decision meant reworking documentation practices, coordinating across sites, and overhauling daily workflows for thousands of clinicians.
What stands out is that this was not treated as a software install. It was a long-term change management transformation effort that required sustained alignment.
2. Mercy Health’s Scheduling Redesign
Mercy Health reworked its scheduling structure to improve satisfaction and efficiency. Rather than centralizing more control, responsibilities were redistributed to local offices.
This operational shift shows that hange management is not only about digital systems. Even process changes require clarity, communication, and accountability.
3. EHR Implementation Challenges in South Africa
A study of EHR implementation at Inkosi Albert Luthuli Central Hospital found that unclear ownership and limited communication slowed adoption.
These change management in healthcare examples highlight a common theme in healthcare organizations: technology alone does not drive improvement. Without steady leadership and clear responsibility, progress stalls.
Best Practices for Effective Change Management in Healthcare
In healthcare, change does not fail because people are unwilling. It fails when the change ignores how hard the work already is. The difference between a smooth transition and a frustrating one usually comes down to a handful of grounded habits.
- Analyse your work: Before redesigning anything, spend time on the floor. Sit in on a shift. Watch how documentation actually happens. Most gaps become obvious when you stop relying on process charts.
- Invite real input, not symbolic input: Clinicians know where friction lives. Ask them early, listen without defending the plan, and show where their input shaped the outcome.
- Draw clear lines around what is changing: Vague messaging creates hallway speculation. Clear, simple explanations reduce unnecessary stress.
- Be honest about workload: If teams are already stretched, acknowledge it. Adjust the timeline if needed. Speed rarely fixes overload.
- Try it where it matters most: A quiet demo is not the same as a busy clinic day. Test changes in real conditions and expect small surprises.
- Stay visible when things get messy: The first few weeks after launch matter more than the kickoff meeting. Quick responses and visible leadership calm uncertainty.
- Notice what people actually do: If staff create workarounds, it usually means the change does not fully fit. That is feedback, not defiance.
- Keep decision-making simple: When trade-offs come up, everyone should know who decides. Confusion slows momentum faster than resistance.
- Adjust early, not later: Small fixes made quickly prevent bigger problems from forming quietly in the background.
At its best, successful change management feels steady and deliberate rather than dramatic or rushed. It is paced thoughtfully, so people feel supported as they adjust instead of pressured to keep up.
Future Trends in Healthcare Change Management
Change in healthcare shows no signs of slowing, and in many ways, it is becoming more continuous and less predictable than before. The future of change management in healthcare transformation will rely less on overseeing isolated initiatives and more on strengthening an organization’s ability to adapt steadily over time without exhausting the people who deliver care.
A few shifts are already noticeable.
- Change is becoming part of normal operations. Instead of treating transformation as a major event with a clear start and finish, many organizations are accepting that adjustment is ongoing. The focus is shifting toward building internal capability so teams can handle steady, smaller changes without feeling destabilized.
- Technology is reshaping clinical behavior in deeper ways. Digital systems in healthcare are no longer just back-office tools. They influence how clinicians document, make decisions, and communicate. Future healthcare system change management will likely pay closer attention to how systems alter thinking patterns, not just workflows.
- Adoption is being monitored more closely. Leaders are looking beyond training completion rates. In change management transformation, data from usage logs and workflow metrics is increasingly used to see whether people are actually working differently, not just logging in.
- Workforce limits are finally being acknowledged. Many organizations have learned the hard way that pushing too much change at once leads to fatigue. Sustainable pacing is becoming central to change management in organizations, especially as staffing pressures continue.
- Accountability is expected to extend beyond launch. There is growing recognition that go-live is not success. In strong change management healthcare efforts, leadership remains engaged long enough to refine and stabilize the change.
What all of this suggests is fairly simple. Change is not slowing down. The organizations that navigate it well will not be the ones with the most ambitious timelines. They will be the ones who handle change steadily, pay attention to how it feels on the ground, and adjust before small strains become bigger problems.
Also Read: Healthcare Technology Trends Redefining 2026
Partner with experts in healthcare software development services to design scalable systems that drive adoption, stability, and long-term impact.
How Appinventiv Supports Healthcare Transformation
At Appinventiv, we recognize that successful healthcare transformation goes beyond implementing new technologies. It requires thoughtful integration with existing workflows and a focus on ensuring that teams fully adopt and utilize the new systems. This is where we come in.
Our healthcare software development services are tailored to help healthcare organizations bridge the gap between technological advancements and real-world clinical operations. With our extensive experience, we focus on building solutions that not only meet technical requirements but also seamlessly align with clinical workflows, making adoption smoother and more effective.
For example, in projects like the Soniphi Vitality Health App and Health e People Health Assessment App, we didn’t just focus on building the software—we ensured that these solutions fit into existing workflows. By working closely with our clients, we create technology that fits naturally into daily operations, ultimately enhancing the patient care experience.
With over 500+ digital health platforms and a proven track record of supporting 450+ healthcare clients, we understand that every step of the healthcare transformation process requires a strategic, well-coordinated approach.
Our goal is to ensure your healthcare organization not only implements new systems but also successfully adopts them for long-term success. Let’s talk!
FAQs
Q. What is change management in healthcare?
A. Change management in healthcare is simply the way hospitals and care organizations move from the old way of working to a new one without losing control in the process. It is about preparing people, adjusting workflows, clarifying ownership, and staying involved long enough for the change to feel normal rather than forced.
Q. Why is change management important in healthcare?
A. The importance of change management solutions for healthcare becomes clear when it is missing. Systems get installed, but staff avoid using them. Policies are updated, but practice remains unchanged. A structured change management process in healthcare helps modernization efforts avoid confusion, fatigue, or patient risk.
Q. How does change management affect patient outcomes?
A. Care quality depends on coordination and clarity. When change management solutions for healthcare transformation are handled well, documentation improves, communication tightens, and errors decrease. When it is rushed or poorly guided, delays and workarounds creep in. The way change is managed directly affects the safety of care delivery.
Q. How can nurse leaders contribute to successful change management?
A. Nurse leaders see where plans meet reality. In settings like change management in mental health nursing, they often recognize strain before anyone else. By validating workflows, flagging risks early, and supporting peers during transitions, they make healthcare system change management more practical and grounded.
Q. How do AI and technology drive change in healthcare?
A. AI, automation, and digital platforms are reshaping how care is delivered. That shift is pushing change management solutions for healthcare organizations to become more deliberate. The right change management tools in healthcare help teams adopt new technology without overwhelming them, especially as organizations work through common barriers to change.
Q. What are the benefits of effective change management in healthcare?
A. Effective change management in healthcare ensures smoother transitions, improves staff adoption of new systems, and enhances operational efficiency. By minimizing disruptions and aligning clinical workflows with new technologies, organizations can maintain patient care quality while implementing transformative changes. This leads to better outcomes, reduced resistance, and a sustainable long-term impact.


- In just 2 mins you will get a response
- Your idea is 100% protected by our Non Disclosure Agreement.
How to Build a Custom Pediatric EMR and EHR System?
Key takeaways: Clinical Precision: Custom systems accommodate pediatric-specific data points like percentile curves and weight-based longitudinal dosing. Interoperability: Seamless data exchange via HL7 FHIR ensures your practice stays connected to pharmacies, labs, and state registries. Regulatory Resilience: Built-in compliance with HIPAA, HITECH, and MACRA/MIPS reduces legal friction. Enhanced Engagement: Parent portals reduce administrative overhead by…

A Practical Guide to Building Your Mental Health Chatbot - Use Cases, Cost, & ROI
Key takeaways: Mental health chatbots work when they know their limits. They’re most useful as a gentle first step, not as a stand-in for real care. Good chatbot design is more about judgment than AI. Clear boundaries, calm responses, and safety matter more than smart language models. Enterprises invest in chatbots to make support easier…

How To Hire the Right Healthcare Developers As Per Your Business Needs?
Key Takeaways The guide to the step-by-step approach to recruiting the right healthcare software developers to meet your business requirements. In-depth dissection of the major technical skills, certifications and healthcare-specific expertise required in developers. Guidelines for carrying out the evaluation of candidates using portfolios, technical interviews, and trial projects. Industry-specific ERM approaches help address regulatory,…