- How Has Automation in Healthcare Become a Strategic Priority for Enterprise Health Systems?
- Use Cases of Automation in Healthcare: Transforming Enterprise Health Systems
- Core Technologies Powering Healthcare Automation Systems
- Healthcare Workflow Automation: How Clinical Workflows Are Being Redesigned Through Automation
- Benefits of Automation in the Healthcare Industry for Enterprise Health Systems
- What Is the ROI of Automation in Healthcare?
- Challenges Healthcare Organizations Face When Implementing Automation
- How Enterprises Can Successfully Implement Healthcare Automation
- Future of Healthcare Automation: From Task Automation to Autonomous Health Systems
- How Appinventiv Helps Healthcare Enterprises Implement Scalable Automation Systems
- Frequently Asked Questions
Key Takeaways
- Healthcare automation helps enterprise health systems reduce administrative overhead while improving clinical workflow efficiency.
- Intelligent automation platforms enable hospitals to manage complex operations without increasing staffing or operational costs.
- AI-powered automation improves care coordination, accelerates decision-making, and strengthens enterprise healthcare system resilience.
- Integrated automation across EHRs, billing systems, and patient platforms eliminates fragmented workflows across hospital operations.
- Enterprise healthcare automation enables scalable digital transformation while maintaining compliance, data security, and operational reliability.
Most healthcare leaders start thinking about automation during very practical moments. An administrator is reviewing late-night operational reports. A physician finishes documentation long after the last patient has left. Finance teams reconciling claims across multiple systems. Small inefficiencies slowly build up until they begin slowing the entire organization down.
Healthcare operations today are far more complex than they were a decade ago. Health systems manage massive volumes of patient data, coordinate care across departments, maintain regulatory compliance, and still deliver timely care. Your teams are expected to handle all of this while working across fragmented platforms and growing documentation requirements.
The strain shows up across the organization. Clinicians spend hours weekly on administrative work. Compliance teams track constantly evolving regulations. IT departments support an expanding network of digital systems. At the same time, hospital margins remain under pressure.
This is why many organizations are now investing in automation in healthcare to simplify how work moves across departments. Hospitals are deploying automated systems to handle repetitive tasks, reduce administrative overhead, and improve operational accuracy. In many cases, healthcare process automation combined with intelligent automation for healthcare is helping teams manage complex workflows without increasing staff workload.
For healthcare leaders, automation is no longer a minor efficiency upgrade. It is rapidly becoming a foundational capability for running modern health systems at scale.
86% of healthcare organizations already use AI technologies across operational workflows
How Has Automation in Healthcare Become a Strategic Priority for Enterprise Health Systems?
Automation in healthcare is now essential as large health systems can no longer rely on manual coordination across fragmented platforms.
With nearly 86% of organizations adopting artificial intelligence, AI and automation in healthcare are becoming foundational to enterprise operations.
Why this shift is happening:
- Fragmented healthcare workflow: Data moves across EHRs, billing, and scheduling, often manually
- Workforce pressure: Staff manage rising patient volumes with limited capacity
- Operational inefficiencies: Repetitive tasks slow down clinical workflows in healthcare
- Regulatory complexity: Compliance increases administrative burden
- Rising expectations: Patients expect faster, digital-first experiences
Where automation is being applied:
- Care coordination and workflow automation in healthcare
- Patient engagement and communication
- Clinical documentation and updates
- Revenue cycle and billing processes
- Hospital administration via ERP in healthcare systems
Together, these healthcare automation solutions reduce manual work, streamline healthcare process automation, and help enterprises scale operations without increasing workload.
Use Cases of Automation in Healthcare: Transforming Enterprise Health Systems
In most hospitals, automation is introduced, where daily work slows down because staff must repeat the same digital tasks again and again.
Leaders usually start with operational areas where delays are easiest to measure. Billing backlogs, long intake queues, documentation overload, or bed allocation issues. Once those problems improve, automation gradually spreads across departments.
Below are the top use case examples of automation in healthcare.
Revenue Cycle Automation
Revenue cycle teams handle a steady stream of administrative work. Insurance verification, claims submission, and coding checks all require accuracy, and small errors can delay payments for weeks.
Many hospitals now use RPA in healthcare to handle these revenue cycle tasks with greater speed and fewer errors.
Typical areas include:
- Insurance eligibility verification
- Claims submission and tracking
- Coding validation
- Billing reconciliation
A real example comes from Phelps Memorial Health Center, which introduced automated analytics tools to improve revenue cycle performance and identify claim issues earlier.
Automation tools can also flag claim errors before submission, reducing denial rates.
Patient Intake and Digital Front Door Automation
Patient intake used to involve stacks of forms at the reception desk. Many hospitals now deploy the right healthcare software types to enable patients to complete intake steps digitally before they even arrive.
Common examples include:
- Online appointment scheduling
- Digital registration forms
- Automated triage questionnaires
- Insurance verification during intake
These changes reduce wait times and enable front desk teams to focus on assisting patients instead of entering paperwork.
Clinical Documentation Automation
Documentation is one of the most time-consuming parts of clinical work. Some hospitals are experimenting with tools that capture conversations and transform them into notes.
For instance, Apollo Hospitals has explored AI tools that transcribe physician discussions and generate discharge summaries.
AI Scribes for Clinical Documentation
Clinical documentation takes up a significant portion of a clinician’s time. AI scribes are emerging as a practical solution to reduce this burden.
These systems use speech recognition and natural language processing to:
- Capture doctor-patient conversations in real time
- Generate structured clinical notes automatically
- Update EHR systems without manual input
- Reduce post-consultation documentation workload
By minimizing time spent on documentation, AI scribes allow clinicians to focus more on patient interaction while improving documentation accuracy and consistency.
Prior Authorization Automation
Prior authorizations are one of the most time-consuming administrative tasks in healthcare. Staff often spend hours coordinating with insurers, submitting documentation, and following up on approvals.
Automation helps streamline this process by:
- Extracting required clinical and insurance data automatically
- Submitting authorization requests without manual intervention
- Tracking approval status in real time
- Flagging missing documentation before submission
This reduces delays in patient care, lowers administrative burden, and accelerates treatment timelines.
Hospital Operations Automation
Automation is also helping hospitals manage operational logistics, with tools like predictive analytics enabling smarter bed allocation, staffing, and discharge planning.
Examples include:
- Bed allocation systems that track patient movement
- Discharge coordination tools
- Supply inventory monitoring
A UK government project involving Kettering General Hospital tested technology to support hospital staff when allocating beds based on patient needs and available capacity.
Across these examples, automation in hospitals is less about replacing people and more about removing repetitive digital work that slows teams down.
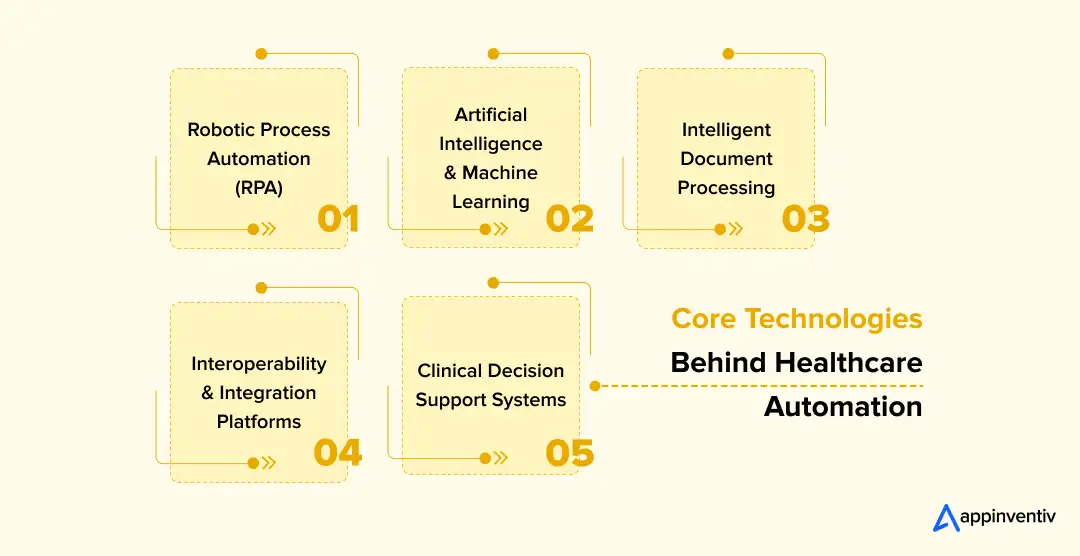
Core Technologies Powering Healthcare Automation Systems
Healthcare automation reduces the need for staff to move data across disconnected systems like EHRs, billing, and scheduling tools. By handling routine digital tasks in the background, it minimizes manual effort. Hospitals adopting automation across workflows have reported up to 45% efficiency gains, especially in administrative and revenue cycle operations.
Below are the technologies that usually make healthcare automation possible.
Robotic Process Automation (RPA)
Robotic Process Automation is often where hospitals begin. It focuses on routine tasks that follow clear steps.
Think about activities that administrative teams repeat throughout the day. Insurance checks, claim submissions, and billing updates. These tasks rarely change and usually follow a fixed process.
RPA tools can perform many of those actions automatically.
Typical examples include:
- Verifying patient insurance eligibility
- Submitting insurance claims
- Updating billing records
- Entering patient registration data
A task that once required staff to open several portals can often be completed automatically in seconds.
Artificial Intelligence and Machine Learning
Some healthcare processes involve more than repeating steps. They require analyzing large amounts of information. This is where AI and machine learning automation begin to work together to handle what automation alone cannot.
Hospitals generate huge volumes of clinical data every day through imaging systems, lab reports, and electronic health records. Artificial intelligence helps interpret that information faster.
Healthcare AI automation is now used in areas such as:
- Identifying high-risk patients through predictive analytics
- Supporting clinicians reviewing medical images
- Detecting patterns in population health data
- Predicting potential readmissions
These systems do not replace medical expertise. They simply help clinicians notice patterns earlier.
Intelligent Document Processing
Healthcare still runs on a surprising amount of paperwork. Patient histories, insurance forms, discharge summaries, referral documents. Administrative teams spend a lot of time reviewing and entering this information into digital systems.
Some hospitals are now also using Natural Language Processing to transform physician conversations into structured medical notes automatically.
Intelligent document processing helps reduce that manual work.
Common uses include:
- Extracting information from medical records
- Processing insurance documentation
- Handling prior authorization forms
- Converting scanned records into structured data
This type of process automation in healthcare can save hours of administrative effort every week.
Interoperability and Integration Platforms
Automation becomes much more useful when healthcare interoperability is in place, allowing systems to share information without manual bridges. Hospitals rely on several standards and integration tools to make that possible.
| Technology | Why It Matters |
|---|---|
| HL7 | Allows clinical systems to exchange patient data |
| FHIR | A modern framework designed for healthcare data sharing |
| Healthcare APIs | Secure connections between digital health platforms |
| Integration Engines | Tools that route information between multiple systems |
These technologies allow automated systems in healthcare to operate across fragmented IT environments.
Clinical Decision Support Systems
Automation is also starting to assist clinicians directly.
Clinical decision support systems analyze patient data and provide helpful prompts during care delivery. A physician reviewing a patient’s chart might receive a medication safety alert or a suggestion based on treatment history.
Examples include:
- Medication interaction alerts
- Treatment recommendations based on patient records
- Predictive insights highlighting possible complications
When implemented carefully, these systems support clinical workflows without adding extra steps for clinicians.
Healthcare Workflow Automation: How Clinical Workflows Are Being Redesigned Through Automation
Healthcare workflow automation transforms stagnant, manual processes into synchronized digital streams that eliminate the “human middleware” responsible for clinical delays and administrative burnout.
Workflow automation in healthcare is essentially the lifeblood of your facility. It represents every step taken from the moment a patient books an appointment to the day their final bill is settled. In most large enterprises, these clinical workflows in healthcare are currently fragmented.
You likely see this in your own operations when a specialist referral sits in an inbox for three days or a nurse spends forty minutes hunting down a discharge summary.
The Friction in Traditional Workflows
Manual handoffs don’t just frustrate staff. They create dangerous bottlenecks that stall care and erode your margins. Common pain points include:
- Fragmented Care Coordination: Information gaps between departments that lead to redundant testing.
- Manual Documentation: Clinicians spend more time on keyboards than on patients.
- Approval Delays: Prior authorizations and referrals are stuck in administrative loops.
- Inefficient Handoffs: Lack of real-time data when transitioning patients from the ER to inpatient beds.
Modern workflow automation for healthcare works by connecting your disparate systems so that data moves even when people are busy. It replaces the “check and double-check” culture with a “notify by exception” model. Your team only steps in when the system flags a deviation. This keeps the routine moving without constant oversight.
Types of Workflow Automation in the Healthcare Industry
When you look at automation in the healthcare industry, three main categories usually emerge as high-impact areas for investment:
| Workflow Type | Focus Area | Examples of Workflow Analysis in Healthcare |
|---|---|---|
| Clinical | Patient’s medical journey | Discharge Planning: Auto-coordinating home care the moment a doctor enters a discharge date. |
| Administrative | Back-office operations | Referral Management: Triggering a scheduling link to a patient’s phone as soon as a referral is received. |
| Patient Engagement | External communication | Digital Onboarding: Automating patient intake forms and insurance verification before the visit. |
Redesigning the Patient Journey
Data-driven workflow redesign allows hospitals to move from anecdotal problem-solving to precise operational engineering. This is the foundation of smart technology in healthcare, one that uses data-driven insight rather than gut feeling to manage operations.
You cannot fix what you cannot see. Most systems rely on gut feelings about why patients wait too long in the ER, but those guesses rarely solve the root cause.
This is where examples of workflow analysis in healthcare become vital for your strategy. Using process mining and digital twins, your team can map the actual path a patient takes.
How workflow analysis improves care coordination:
- Identifying “Dead Time”: Pinpointing exactly how long a patient waits between a “physician ready” status and the actual start of a consultation.
- Analyzing EHR Audit Logs: Using data mining to track a patient’s digital footprint and identify where documentation steps are duplicated across departments.
- Bottleneck Detection: Finding specific points where human intervention is slow, such as the 45-minute lag between a discharge order and the transport team notification.
- Simulation: Testing how a new clinical workflow automation would perform before rolling it out to the entire hospital floor.
Still, the goal isn’t just to make things faster. It is creating a predictable environment. When a patient admission workflow is automated, the intake data flows directly into the clinical record without a single keystroke from the nursing staff.
This small detail saves minutes per patient. Across a large enterprise health system, those minutes scale into thousands of hours of recovered clinical capacity every year.
Identify automation opportunities across clinical workflows and fragmented healthcare systems.
Benefits of Automation in the Healthcare Industry for Enterprise Health Systems
Automation helps health systems remove routine digital work so teams can spend more time on care and less on coordination.
In most hospitals, the benefits show up quietly in everyday operations rather than through one major change.
Below are the advantages of adopting healthcare automation.
Reduced Administrative Burden
Hospital staff handle a large amount of background work every day. Automation reduces some of that repetition.
- Insurance eligibility checks completed without manual lookup
- Claims and billing tasks are processed more quickly
- Patient information is shared across systems without retyping
Improved Clinical Efficiency
When fewer manual steps are involved, clinicians spend less time navigating software. This is where intelligent automation makes the biggest difference, removing the repetitive steps that slow down clinical teams.
- Lab results reaching physicians as soon as they are available
- Patient records are updated across systems automatically
- Care teams receive alerts when patient information changes
Enhanced Patient Experience
Automation also improves how patients interact with healthcare providers.
- Online appointment booking instead of waiting on phone lines
- Digital intake forms completed before arrival
- Appointment reminders are sent automatically
Improved Compliance and Data Accuracy
Healthcare organizations must maintain reliable records.
- Audit trails are created automatically
- Consistent patient data across hospital systems
- Fewer errors caused by manual data entry
What Is the ROI of Automation in Healthcare?
Investing in automation in healthcare typically starts with focused workflows and scales over time. Costs vary based on system complexity, integrations, and compliance requirements, but most enterprises see measurable efficiency gains within months.
Estimated Cost Breakdown
| Component | Cost Range (USD) | What It Covers |
|---|---|---|
| Process Assessment & Planning | $10,000 – $30,000 | Workflow analysis, use-case identification |
| RPA / Workflow Automation Setup | $25,000 – $100,000 | Bot development, rule-based automation |
| AI / Advanced Automation | $50,000 – $200,000+ | Predictive models, intelligent automation |
| Integration & Interoperability | $30,000 – $120,000 | EHR, billing, APIs, data exchange |
| Compliance & Security Setup | $15,000 – $50,000 | Audit logs, encryption, access control |
| Maintenance & Optimization (Annual) | $20,000 – $80,000 | Monitoring, updates, scaling |
ROI and Business Impact
- 30–45% efficiency improvement in administrative and revenue cycle workflows
- Reduced operational costs through fewer manual processes
- Faster turn around times for patient intake, billing, and documentation
- Improved data accuracy and compliance readiness
- Better resource utilization without increasing staff
Well-implemented healthcare automation solutions typically deliver ROI within 6–12 months, especially in high-volume operational areas.
Challenges Healthcare Organizations Face When Implementing Automation
Automation promises efficiency, but most hospitals discover the hard part begins during implementation. The challenges in clinical workflow automation usually appear where modern automation tools meet older systems and established clinical routines.
Legacy Healthcare IT Infrastructure
Many health systems still run legacy systems introduced years ago, including EHRs, imaging tools, and billing platforms that were never designed to integrate with modern automation layers. An EHR might manage patient records while separate tools handle imaging, billing, or scheduling. These platforms were not always designed to integrate with automation layers.
Connecting them often requires additional engineering work.
- introduce middleware that connects older hospital systems,
- modernize infrastructure in phases rather than replacing everything,
- move selected workloads to cloud computing environments where automation tools integrate more easily, and infrastructure scales with demand.
Interoperability Challenges
Hospital software environments are rarely unified. Lab platforms, radiology systems, and EHR tools frequently store data in different formats. When systems cannot exchange information easily, automated workflows stall.
- Implement interoperability standards such as HL7 or FHIR
- expose clinical data through secure healthcare APIs
- Deploy integration engines that synchronize data across platforms
Data Security and Regulatory Compliance
Healthcare data carries strict regulatory obligations. Automation systems must still follow frameworks like HIPAA in the United States or GDPR in Europe.
Any new workflow that moves patient information across systems must treat automation and compliance as core design considerations and not afterthoughts.
- Encrypt sensitive health data during storage and transfer
- Maintain detailed audit logs for compliance reviews
- Apply identity and access management controls across automated workflows to ensure only authorized personnel can interact with sensitive patient data.
Clinical Adoption Resistance
Technology changes rarely succeed without clinical support. Physicians and nurses sometimes hesitate when new tools alter familiar workflows.
Even small workflow changes can create friction during busy shifts.
- involve clinical teams when designing automation workflows
- Provide hands-on training before deployment
- introduce automation through smaller pilot programs first
Automation Governance
Once automation spreads across departments, oversight becomes essential. Without monitoring, automated workflows can scale errors as quickly as they scale efficiency.
- Create governance teams responsible for automation oversight
- Monitor workflow performance continuously
- Assign clear ownership for system management or consider managed IT services that specialize in keeping healthcare automation environments stable.
How Enterprises Can Successfully Implement Healthcare Automation
Successful healthcare automation implementation is a key pillar of Healthcare 4.0, requiring a phased framework that prioritizes high-impact clinical bottlenecks while ensuring data remains interoperable across the entire enterprise ecosystem.
The essential steps for a resilient implementation include:
- Identify High-Impact Opportunities: Look for “high-volume, low-complexity” tasks first, like automating the 500 eligibility checks your staff performs every Monday morning.
- Conduct Healthcare Workflow and Process Analysis: Use process mining to find out why a simple specialist referral takes three days to clear your system.
- Build Interoperable Healthcare Data Platforms: Ensure your automation tools speak FHIR and HL7 fluently so they don’t just create another data silo.
- Introduce Intelligent Automation Gradually: Start with administrative “assists” before moving into cognitive clinical decision support.
- Establish Governance and Monitoring Systems: Create a central dashboard to track bot performance and ensure clinical safety stays at the forefront.
Even so, the most technically perfect system will fail if your doctors feel it complicates their day. End-user design is just as important as the backend code.
Design scalable healthcare automation frameworks aligned with enterprise clinical operations
Future of Healthcare Automation: From Task Automation to Autonomous Health Systems
The future of healthcare automation is evolving from task-based bots to autonomous systems that manage capacity and patient risks in real time. Enterprises are moving toward self-healing operations powered by AI and intelligent workflows. With the market projected to reach $96 billion by 2034, adoption is accelerating rapidly.
Key trends defining the future of healthcare automation include:
- Intelligent Automation Platforms: These systems unify GenAI, RPA, and predictive analytics to handle unstructured data—like patient voice recordings—and convert them into actionable clinical orders.
- Autonomous Hospital Operations: AI-driven “Command Centers” rely on business intelligence to optimize resource allocation, automatically adjusting staffing levels and operating room schedules based on real-time inflow.
- Predictive and Preventive Care Systems: The next generation of intelligent automation will use wearable data to flag chronic health risks early, driving personalization in healthcare months before hospitalization becomes necessary.
- AI-Augmented Decision Making: Automation will act as a “Co-pilot” for specialists, providing evidence-based treatment suggestions and complex diagnostic support during the live patient encounter.
- Agentic AI Systems: Enabling autonomous decision-making across clinical and operational workflows, with systems that can initiate actions, coordinate tasks, and adapt in real time with minimal human intervention.
How Appinventiv Helps Healthcare Enterprises Implement Scalable Automation Systems
Healthcare automation works best when it fits the daily rhythm of hospitals. In many conversations with healthcare leaders, the first step is simply identifying where teams lose time across clinical, operational, or administrative workflows.
At Appinventiv, we start by mapping those pressure points and designing automation strategies around them as part of our broader healthcare software development services. Over the past 10+ years working in HealthTech, our teams have helped healthcare organizations deploy 500+ digital health platforms while supporting more than 450 healthcare clients globally.
From there, we build intelligent automation solutions using AI, machine learning, RPA, and predictive analytics. These systems are designed to integrate smoothly with EHR platforms, hospital management systems, patient engagement tools, and interoperability standards like FHIR and HL7. Our engineers have also integrated 300+ connected medical devices into healthcare environments.
The goal is measurable improvement. Many hospital partners see up to 45% operational efficiency gains, 90%+ clinical data accuracy, and patient-facing applications that maintain 95% satisfaction, all supported by infrastructure designed for 99.9% uptime.
Let’s connect and plan your intelligent healthcare automation strategy.
Frequently Asked Questions
Q. What is automation in healthcare?
A. Automation in healthcare means using technology to handle routine clinical, administrative, or operational tasks that once required manual effort. Think of appointment scheduling, claims processing, or clinical documentation happening automatically through software. The goal is simple: reduce repetitive work so healthcare teams can spend more time focusing on patient care.
Q. How can healthcare automation help patients?
A. For patients, automation often appears as a smoother medical experience. Appointment reminders arrive automatically, prescriptions move quickly through systems, and test results reach physicians faster. This reduces waiting times and confusion, helping patients receive care more efficiently while staying better informed about their treatment journey.
Q. How can healthcare automation help health systems?
A. Health systems use automation to manage complex operations more efficiently. Hospitals handle thousands of daily processes across departments, and automation helps coordinate them. From optimizing staff schedules to processing insurance claims, automation reduces operational pressure and helps healthcare organizations manage resources more effectively.
Q. How long does it take to implement healthcare automation?
A. Implementation timelines depend on scope and system complexity.
- Basic automation (RPA for admin tasks): 4–8 weeks
- Workflow-level automation (integrations + multiple use cases): 2–4 months
- Enterprise-scale automation (AI + interoperability + governance): 6–12+ months
Most organizations start with high-impact workflows and expand gradually to reduce risk and accelerate early ROI.
Q. How do you build a governance framework for AI automation in healthcare?
A. A strong governance framework ensures automation remains compliant, safe, and scalable. Key components include:
- Data governance: Ensure data quality, access control, and audit trails
- Compliance alignment: Adhere to regulations like HIPAA/GDPR with built-in safeguards
- Model oversight: Monitor AI performance, bias, and drift over time
- Human-in-the-loop controls: Enable clinical validation for critical decisions
- Centralized monitoring: Track workflow performance and system reliability
Governance should be embedded from the start, not added after deployment.
Q. What is the difference between RPA and intelligent automation in healthcare?
A. RPA (Robotic Process Automation) handles repetitive, rule-based tasks such as claims processing, data entry, and appointment scheduling. It follows predefined workflows without decision-making capability.
Intelligent Automation combines RPA with AI, machine learning, and analytics to handle complex, data-driven tasks. It can interpret clinical data, generate insights, and support decision-making across workflows.
In practice, RPA is often the starting point, while intelligent automation enables end-to-end transformation across clinical and operational systems.
Q. Does automation replace healthcare professionals?
A. No, automation is designed to support healthcare professionals, not replace them. Medicine relies heavily on human judgment, empathy, and clinical expertise. Automation handles repetitive administrative tasks, allowing doctors, nurses, and staff to focus on diagnosis, treatment decisions, and patient interaction where human care truly matters.
Q. How does healthcare workflow automation actually work?
A. Healthcare workflow automation connects different systems, so information moves automatically between them. For example, when a patient registers, their details can flow from intake systems to billing, clinical records, and scheduling platforms. These automated connections reduce manual data entry and ensure information stays consistent across departments.
Q. How much time can healthcare providers save with automation?
A. Many healthcare providers recover several hours each week by automating administrative tasks such as documentation, appointment coordination, and billing workflows. While the exact numbers vary by organization, even small improvements can significantly reduce workload, giving clinicians more time to focus on patient care.
Q. What should healthcare organizations evaluate before implementing automation?
A. Before adopting intelligent automation and robotics, healthcare organizations should assess data readiness, integration capabilities, and scalable infrastructure. Identifying workflow inefficiencies and prioritizing administrative processes for automation is essential. Leaders must also ensure strong governance, data integrity, and compliance alignment with regulatory compliance requirements. Building systems that generate audit-ready reports helps maintain transparency, security, and long-term operational reliability.


- In just 2 mins you will get a response
- Your idea is 100% protected by our Non Disclosure Agreement.

Telehealth Business Ideas for 2026: Models, Technology Stack, and Growth Strategy
Key Takeaways Choose what people will keep using: The strongest telehealth models solve ongoing needs, not one-time problems. Integration matters more than features: Platforms that fit into real care workflows tend to scale without friction. Recurring care drives stable revenue: Chronic care, employer-led models, and guided programs create consistent usage. Partnerships accelerate growth: B2B and…
How Much Does EHR Software Development Cost? Enterprise Pricing, Hidden Costs, and ROI Analysis
Key Takeaways EHR implementation costs vary widely, from $20,000 for small clinics to $900,000+ for enterprise systems, based on scope, complexity, and customization. Whereas EHR software development costs between $30,000 to $1M+, depending on the complexity of development, choice of technologies and advanced features. Hidden costs like data migration, workflow disruption, training, and compliance can…

Key Takeaways Fitness app cost ranges from $40,000 to $400,000, based on features and scale Real cost includes build, scaling, maintenance, and integrations Business model drives backend complexity and overall pricing Strong retention matters more than downloads for ROI Early tech and monetization choices prevent costly rework If you’ve started putting numbers around your fitness…